GIANVI (drospirenone 3 mg ethinyl estradiol 0.02 mg) Dailymed
Generic: drospirenone and ethinyl estradiol is used for the treatment of Adrenal Insufficiency Aged Atrial Fibrillation Breast Neoplasms Cerebrovascular Disorders Coronary Disease Diabetic Angiopathies Endocarditis, Bacterial Headache Heart Valve Diseases Hypertension Jaundice Kidney Diseases Liver Diseases Liver Neoplasms Migraine Disorders Neoplasms, Hormone-Dependent Pregnancy Pulmonary Embolism Thromboembolism Thrombophlebitis Tobacco Use Disorder Uterine Hemorrhage Endometrial Neoplasms Venous Thrombosis Headache Disorders Cerebral Arterial Diseases Coronary Artery Disease Hypogonadism Menopause, Premature Menorrhagia Prostatic Neoplasms Osteoporosis, Postmenopausal Primary Ovarian Insufficiency Hot Flashes Tobacco Use
Go PRO for all pill images
Rx only
PATIENTS SHOULD BE COUNSELED THAT THIS PRODUCT DOES NOT PROTECT AGAINST HIV INFECTION (AIDS) AND OTHER SEXUALLY TRANSMITTED DISEASES
Description
Gianvi™ (drospirenone and ethinyl estradiol tablets) 3 mg/0.02 mg provides an oral contraceptive regimen consisting of 24 active film-coated tablets each containing 3 mg of drospirenone and 0.02 mg of ethinyl estradiol and 4 inert film-coated tablets. Other ingredients are anhydrous lactose, corn starch, crospovidone, FD&C red no. 40 aluminum lake, FD&C yellow no. 6 aluminum lake, hypromellose, magnesium stearate, polyethylene glycol, polysorbate 80, povidone, pregelatinized starch and titanium dioxide. The inert tablets contain anhydrous lactose, hypromellose, magnesium stearate, and microcrystalline cellulose.
Drospirenone (6R,7R,8R,9S,10R,13S,14S,15S,16S,17S)-1,3’,4’,6,6a,7,8,9,10,11, 12,13,14,15,15a,16-hexadecahydro-10,13-dimethylspiro-[17H-dicyclopropa-[6,7:15,16]cyclopenta[a]phenanthrene-17,2’(5H)-furan]-3,5’(2H)-dione) is a synthetic progestational compound. Ethinyl estradiol (19-nor-17α-pregna 1,3,5(10)-triene-20-yne-3, 17-diol) is a synthetic estrogenic compound. The structural formulas are as follows:
Drospirenone
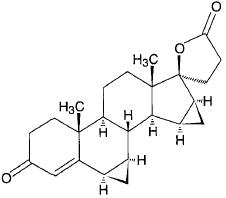
C24H30O3 Molecular Weight: 366.5
Ethinyl Estradiol
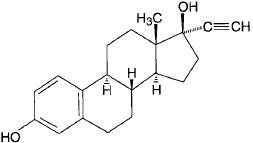
C20H24O2 Molecular Weight: 296.4
Clinical Pharmacology
Pharmacodynamics
Oral Contraception
Combination oral contraceptives (COCs) act by suppression of gonadotropins. Although the primary mechanism of this action is inhibition of ovulation, other alterations include changes in the cervical mucus (which increases the difficulty of sperm entry into the uterus) and the endometrium (which reduces the likelihood of implantation).
Drospirenone is a spironolactone analogue with antimineralocorticoid activity. Preclinical studies in animals and in vitro have shown that drospirenone has no androgenic, estrogenic, glucocorticoid, or antiglucocorticoid activity. Preclinical studies in animals have also shown that drospirenone has antiandrogenic activity.
Acne
Acne vulgaris is a skin condition with a multifactorial etiology including androgen stimulation of sebum production. While the combination of ethinyl estradiol and drospirenone increases sex hormone binding globulin (SHBG) and decreases free testosterone, the relationship between these changes and a decrease in the severity of facial acne in otherwise healthy women with this skin condition has not been established. The impact of the antiandrogenic activity of drospirenone on acne is not known.
Pharmacokinetics
Absorption
The absolute bioavailability of drospirenone (DRSP) from a single entity tablet is about 76%. The absolute bioavailability of ethinyl estradiol (EE) is approximately 40% as a result of presystemic conjugation and first-pass metabolism. The absolute bioavailability of drospirenone and ethinyl estradiol tablets, which is a combination tablet of drospirenone and ethinyl estradiol stabilized by betadex as a clathrate (molecular inclusion complex), has not been evaluated. The bioavailability of EE is similar when dosed via a betadex clathrate formulation compared to when it is dosed as a free steroid. Serum concentrations of DRSP and EE reached peak levels within 1 to 2 hours after administration of drospirenone and ethinyl estradiol tablets.
The pharmacokinetics of DRSP are dose proportional following single doses ranging from 1 to 10 mg. Following daily dosing of drospirenone and ethinyl estradiol tablets, steady-state DRSP concentrations were observed after 8 days. There was about 2 to 3 fold accumulation in serum Cmax and AUC (0-24h) values of DRSP following multiple dose administration of drospirenone and ethinyl estradiol tablets (see Table I).
For EE, steady-state conditions are reported during the second half of a treatment cycle. Following daily administration of drospirenone and ethinyl estradiol tablets serum Cmax and AUC (0-24h) values of EE accumulate by a factor of about 1.5 to 2 (see Table I).
TABLE I: TABLE OF PHARMACOKINETIC PARAMETERS OF DROSPIRENONE AND ETHINYL ESTRADIOL TABLETS (Drospirenone 3 mg and Ethinyl Estradiol 0.02 mg) Drospirenone
Cycle /
Day
No. of
Subjects
Cmax Âgeometric mean (geometric coefficient of variation) Â
(ng/mL)
Tmaxmedian (range)
(h)
AUC (0-24h)
(ng•h/mL)
t1/2
(h)1/1 23 38.4 (25) 1.5 (1 to 2) 268 (19) NA 1/21 23 70.3 (15) 1.5 (1 to 2) 763 (17) 30.8 (22) Ethinyl Estradiol
Cycle /
Day
No. of
Subjects
Cmax
(pg/mL)
Tmax
(h)
AUC (0-24h)
(pg•h/mL)
t1/2
(h)1/1 23 32.8 (45) 1.5 (1 to 2) 108 (52) NA 1/21 23 45.1 (35) 1.5 (1 to 2) 220 (57) NA NA = Not available Effect of Food
The rate of absorption of DRSP and EE following single administration of a formulation similar to drospirenone and ethinyl estradiol tablets was slower under fed (high fat meal) conditions with the serum Cmax being reduced about 40% for both components. The extent of absorption of DRSP, however, remained unchanged. In contrast, the extent of absorption of EE was reduced by about 20% under fed conditions.
Distribution
DRSP and EE serum levels decline in two phases. The apparent volume of distribution of DRSP is approximately 4 L/kg and that of EE is reported to be approximately 4 to 5 L/kg.
DRSP does not bind to sex hormone binding globulin (SHBG) or corticosteroid binding globulin (CBG) but binds about 97% to other serum proteins. Multiple dosing over 3 cycles resulted in no change in the free fraction (as measured at trough levels). EE is reported to be highly but non-specifically bound to serum albumin (approximately 98.5%) and induces an increase in the serum concentrations of both SHBG and CBG. EE induced effects on SHBG and CBG were not affected by variation of the DRSP dosage in the range of 2 to 3 mg.
Metabolism
The two main metabolites of DRSP found in human plasma were identified to be the acid form of DRSP generated by opening of the lactone ring and the 4,5-dihydrodrospirenone-3-sulfate. These metabolites were shown not to be pharmacologically active. In in vitro studies with human liver microsomes, DRSP was metabolized only to a minor extent mainly by Cytochrome P450 3A4 (CYP3A4).
EE has been reported to be subject to presystemic conjugation in both small bowel mucosa and the liver. Metabolism occurs primarily by aromatic hydroxylation but a wide variety of hydroxylated and methylated metabolites are formed. These are present as free metabolites and as conjugates with glucuronide and sulfate. CYP3A4 in the liver is responsible for the 2-hydroxylation which is the major oxidative reaction. The 2-hydroxy metabolite is further transformed by methylation and glucuronidation prior to urinary and fecal excretion.
Excretion
DRSP serum levels are characterized by a terminal disposition phase half-life of approximately 30 hours after both single and multiple dose regimens. Excretion of DRSP was nearly complete after ten days and amounts excreted were slightly higher in feces compared to urine. DRSP was extensively metabolized and only trace amounts of unchanged DRSP were excreted in urine and feces. At least 20 different metabolites were observed in urine and feces. About 38 to 47% of the metabolites in urine were glucuronide and sulfate conjugates. In feces, about 17 to 20% of the metabolites were excreted as glucuronides and sulfates.
For EE the terminal disposition phase half-life has been reported to be approximately 24 hours. EE is not excreted unchanged. EE is excreted in the urine and feces as glucuronide and sulfate conjugates and undergoes enterohepatic circulation.
Special Populations
No clinically significant difference was observed between the pharmacokinetics of DRSP or EE in Japanese versus Caucasian women (age 20 to 35) when drospirenone and ethinyl estradiol tablets were administered daily for 21 days. Other ethnic groups have not been studied.
Drospirenone and ethinyl estradiol tablets are contraindicated in patients with hepatic dysfunction (see CONTRAINDICATIONS and BOLDED WARNING). The mean exposure to DRSP in women with moderate liver impairment is approximately three times higher than the exposure in women with normal liver function. Drospirenone and ethinyl estradiol tablets have not been studied in women with severe hepatic impairment.
Drospirenone and ethinyl estradiol tablets are contraindicated in patients with renal insufficiency (see CONTRAINDICATIONS and BOLDED WARNING).
The effect of renal insufficiency on the pharmacokinetics of DRSP (3 mg daily for 14 days) and the effect of DRSP on serum potassium levels were investigated in female subjects (n = 28, age 30 to 65) with normal renal function and mild and moderate renal impairment. All subjects were on a low potassium diet. During the study 7 subjects continued the use of potassium sparing drugs for the treatment of the underlying illness. On the 14th day (steady-state) of DRSP treatment, serum DRSP levels in the group with mild renal impairment (creatinine clearance CLcr, 50 to 80 mL/min) were comparable to those in the group with normal renal function (CLcr, >80 mL/min). The serum DRSP levels were on average 37% higher in the group with moderate renal impairment (CLcr, 30 to 50 mL/min) compared to those in the group with normal renal function. DRSP treatment was well tolerated by all groups. DRSP treatment did not show any clinically significant effect on serum potassium concentration. Although hyperkalemia was not observed in the study, in five of the seven subjects who continued use of potassium sparing drugs during the study, mean serum potassium levels increased by up to 0.33 mEq/L. Therefore, potential exists for hyperkalemia to occur in subjects with renal impairment whose serum potassium is in the upper reference range, and who are concomitantly using potassium sparing drugs.
Indications And Usage
Gianvi™ (drospirenone and ethinyl estradiol tablets) 3 mg/0.02 mg is indicated for the prevention of pregnancy in women who elect to use an oral contraceptive.
Oral contraceptives are highly effective. Table II uls the typical unintended pregnancy rates for users of combination oral contraceptives and other methods of contraception. The efficacy of these contraceptive methods, except sterilization and contraceptive implants and IUDs, depends upon the reliability with which they are used. Correct and consistent use of methods can result in lower failure rates.
Gianvi™ (drospirenone and ethinyl estradiol tablets) is indicated for the treatment of moderate acne vulgaris in women at least 14 years of age, who have no known contraindications to oral contraceptive therapy and have achieved menarche. Gianvi™ (drospirenone and ethinyl estradiol tablets) should be used for the treatment of acne only if the patient desires an oral contraceptive for birth control.
TABLE II: PERCENTAGE OF WOMEN EXPERIENCING AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF TYPICAL USE AND FIRST YEAR OF PERFECT USE OF CONTRACEPTION AND THE PERCENTAGE CONTINUING USE AT THE END OF THE FIRST YEAR: UNITED STATES.
Â
Â% of Women Experiencing an Unintended Pregnancy Within the First Year of Use % of Women Continuing Use at One Year Method (1) Typical Use (2) Perfect Use (3) (4) Chance 85 85 40 Spermicides 26 6 63 Periodic abstinence 25 Calendar 9 Ovulation method 3 Sympto-thermal 2 Post-ovulation 1 Withdrawal 19 4 Cap With spermicidal cream or jelly. Parous women 40 26 42 Nulliparous women 20 9 56 Sponge Parous women 40 20 42 Nulliparous women 20 9 56 Diaphragm 20 6 56 Condom Female (Reality) 21 5 56 Male 14 3 61 Pill 5 71 progestin only 0.5 combined 0.1 IUD Progesterone T 2 1.5 81 Copper T 380A 0.8 0.6 78 Lng 20 0.1 0.1 81 Depo Provera 0.3 0.3 70 Norplant and Norplant-2 0.05 0.05 88 Female sterilization 0.5 0.5 100 Male sterilization 0.15 0.1 100 Emergency Contraceptive Pills: Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. Lactational Amenorrhea Method: LAM is a highly effective, temporary method of contraception. Source: Trussell J, Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Guest F, Kowal D, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998. Oral Contraceptive Clinical Trial
In the primary contraceptive efficacy study of drospirenone and ethinyl estradiol tablets (3 mg DRSP/0.02 mg EE) of up to 1 year duration, 1,027 subjects were enrolled and completed 11,480 28-day cycles of use. The age range was 17 to 36 years. The racial demographic was: 87.8% Caucasian, 4.6% Hispanic, 4.3% Black, 1.2% Asian, and 2.1% other. Women with a BMI greater than 35 were excluded from the trial. The pregnancy rate (Pearl Index) was 1.41 per 100 woman-years of use based on 12 pregnancies that occurred after the onset of treatment and within 14 days after the last dose of drospirenone and ethinyl estradiol tablets in women 35 years of age or younger during cycles in which no other form of contraception was used.
Acne Clinical Trials
In two multicenter, double blind, randomized, placebo-controlled studies, 889 subjects, ages 14 to 45 years, with moderate acne received drospirenone and ethinyl estradiol tablets or placebo for six 28 day cycles. The primary efficacy endpoints were the percent change in inflammatory lesions, non-inflammatory lesions, total lesions, and the percentage of subjects with a “clear” or “almost clear” rating on the Investigator’s Static Global Assessment (ISGA) scale on day 15 of cycle 6, as presented in Table III:
TABLE III: EFFICACY RESULTS FOR ACNE TRIALS* * Evaluated at day 15 of cycle 6, last observation carried forward for the Intent to treat population Study 1 Study 2 Drospirenone and Ethinyl Estradiol Tablets N=228 Placebo N=230 Drospirenone and Ethinyl Estradiol Tablets N=218 Placebo N=213 ISGA Success Rate 35 (15%) 10 (4%) 46 (21%) 19 (9%)
Inflammatory Lesions
Mean Baseline Count
Mean Absolute (%) Reduction
33
15 (48%)
33
11 (32%)
32
16 (51%)
32
11 (34%)
Non-inflammatory Lesions
Mean Baseline Count
Mean Absolute (%) Reduction
47
18 (39%)
47
10 (18%)
44
17 (42%)
44
11 (26%)
Total lesions
Mean Baseline Count
Mean Absolute (%) reduction
80
33 (42%)
80
21 (25%)
76
33 (46%)
76
22 (31%)
Contraindications
Gianvi™ (drospirenone and ethinyl estradiol tablets) should not be used in women who have the following:
- Renal insufficiency
- Hepatic dysfunction
- Adrenal insufficiency
- Thrombophlebitis or thromboembolic disorders
- A past history of deep-vein thrombophlebitis or thromboembolic disorders
- Cerebral-vascular or coronary-artery disease (current or history)
- Valvular heart disease with thrombogenic complications
- Severe hypertension
- Diabetes with vascular involvement
- Headaches with focal neurological symptoms
- Major surgery with prolonged immobilization
- Known or suspected carcinoma of the breast
- Carcinoma of the endometrium or other known or suspected estrogen-dependent neoplasia
- Undiagnosed abnormal genital bleeding
- Cholestatic jaundice of pregnancy or jaundice with prior pill use
- Known or suspected pregnancy
- Liver tumor (benign or malignant) or active liver disease
- Heavy smoking (≥ 15 cigarettes per day) and over age 35
- Hypersensitivity to any component of this product
Warnings
Boxed Warning section
Cigarette smoking increases the risk of serious cardiovascular side effects from oral contraceptive use. This risk increases with age and with heavy smoking (15 or more cigarettes per day) and is quite marked in women over 35 years of age. Women who use oral contraceptives should be strongly advised not to smoke.
Gianvi™ (drospirenone and ethinyl estradiol tablets) contains 3 mg of the progestin drospirenone that has antimineralocorticoid activity, including the potential for hyperkalemia in high-risk patients, comparable to a 25 mg dose of spironolactone. Gianvi™ (drospirenone and ethinyl estradiol tablets) should not be used in patients with conditions that predispose to hyperkalemia (i.e., renal insufficiency, hepatic dysfunction and adrenal insufficiency). Women receiving daily, long-term treatment for chronic conditions or diseases with medications that may increase serum potassium should have their serum potassium level checked during the first treatment cycle. Medications that may increase serum potassium include ACE inhibitors, angiotensin – II receptor antagonists, potassium-sparing diuretics, potassium supplementation, heparin, aldosterone antagonists, and NSAIDs.
The use of oral contraceptives is associated with increased risks of several serious conditions including venous and arterial thrombotic and thromboembolic events (such as myocardial infarction, thromboembolism, stroke), hepatic neoplasia, gallbladder disease, and hypertension. The risk of serious morbidity or mortality is very small in healthy women without underlying risk factors. The risk of morbidity and mortality increases significantly in the presence of other underlying risk factors such as hypertension, hyperlipidemias, obesity and diabetes.
Practitioners prescribing oral contraceptives should be familiar with the following information relating to these risks.
The information contained in this package insert is based principally on studies carried out in patients who used oral contraceptives with higher formulations of estrogens and progestogens than those in common use today. The effect of long-term use of the oral contraceptives with lower formulations of both estrogens and progestogens remains to be determined.
Throughout this labeling, epidemiologic studies reported are of two types: retrospective or case control studies and prospective or cohort studies. Case control studies provide a measure of the relative risk of a disease, namely, a ratio of the incidence of a disease among oral contraceptive users to that among nonusers. The relative risk does not provide information on the actual clinical occurrence of a disease. Cohort studies provide a measure of attributable risk, which is the difference in the incidence of disease between oral contraceptive users and nonusers. The attributable risk does provide information about the actual occurrence of a disease in the population. For further information, the reader is referred to a text on epidemiologic methods.
1. Thromboembolic Disorders and Other Vascular Problems
a. Myocardial Infarction
An increased risk of myocardial infarction has been attributed to oral contraceptive use. This risk is primarily in smokers or women with other underlying risk factors for coronary-artery disease such as hypertension, hypercholesterolemia, morbid obesity, and diabetes. The relative risk of heart attack for current oral contraceptive users has been estimated to be two to six. The risk is very low under the age of 30.
Smoking in combination with oral contraceptive use has been shown to contribute substantially to the incidence of myocardial infarctions in women in their mid-thirties or older with smoking accounting for the majority of excess cases. Mortality rates associated with circulatory disease have been shown to increase substantially in smokers over the age of 35 and nonsmokers over the age of 40 (Table IV) among women who use oral contraceptives.
TABLE IV: CIRCULATORY DISEASE MORTALITY RATES PER 100,000 WOMAN- YEARS BY AGE, SMOKING STATUS AND ORAL CONTRACEPTIVE USE (Adapted from P.M. Layde and V. Beral) AGE EVER-USERSNON-SMOKERS
EVER-USERS
SMOKERS
CONTROLS
NON-SMOKERS
CONTROL
SMOKERS15 to 24 0 10.5 0 0 25 to 34 4.4 14.2 2.7 4.2 35 to 44 21.5 63.4 6.4 15.2 45+ 52.4 206.7 11.4 27.9
Oral contraceptives may compound the effects of well-known risk factors, such as hypertension, diabetes, hyperlipidemias, age and obesity. In particular, some progestogens are known to decrease HDL cholesterol and cause glucose intolerance, while estrogens may create a state of hyperinsulinism. Oral contraceptives have been shown to increase blood pressure among users (see section 9 in WARNINGS). Similar effects on risk factors have been associated with an increased risk of heart disease. Oral contraceptives must be used with caution in women with cardiovascular disease risk factors.
b. Thromboembolism
An increased risk of thromboembolic and thrombotic disease associated with the use of oral contraceptives is well established. Case control studies have found the relative risk of users compared to nonusers to be 3 for the first episode of superficial venous thrombosis, 4 to 11 for deep vein thrombosis or pulmonary embolism, and 1.5 to 6 for women with predisposing conditions for venous thromboembolic disease. Cohort studies have shown the relative risk to be somewhat lower, about 3 for new cases and about 4.5 for new cases requiring hospitalization. The risk of thromboembolic disease due to oral contraceptives is not related to length of use and disappears after pill use is stopped.
A two- to four-fold increase in the relative risk of post-operative thromboembolic complications has been reported with the use of oral contraceptives. The relative risk of venous thrombosis in women who have predisposing conditions is twice that of women without such medical conditions. If feasible, oral contraceptives should be discontinued from at least four weeks prior to and for two weeks after elective surgery of a type associated with an increase in risk of thromboembolism and during and following prolonged immobilization. Since the immediate postpartum period is also associated with an increased risk of thromboembolism, combined oral contraceptives should be started no earlier than four to six weeks after delivery and at that time only in women who elect not to breast feed.
Several studies have investigated the relative risks of thromboembolism in women using a different drospirenone-containing COC (Yasmin, which contains 0.030 mg of ethinyl estradiol and 3 mg of drospirenone) compared to those in women using COCs containing other progestins. Two prospective cohort studies, both evaluating the risk of venous and arterial thromboembolism and death, were initiated at the time of Yasmin approval.1, 2 The first (EURAS) showed the risk of thromboembolism (particularly venous thromboembolism) and death in Yasmin users to be comparable to that of other oral contraceptive preparations, including those containing levonorgestrel (a so-called second generation COC). The second prospective cohort study (Ingenix) also showed a comparable risk of thromboembolism in Yasmin users compared to users of other COCs, including those containing levonorgestrel. In the second study, COC comparator groups were selected based on their having similar characteristics to those being prescribed Yasmin.
Two additional epidemiological studies, one case-control study (van Hylckama Vlieg et al.3) and one retrospective cohort study (Lidegaard et al.4) suggested that the risk of venous thromboembolism occurring in Yasmin users was higher than that for users of levonorgestrel-containing COCs and lower than that for users of desogestrel/gestodene-containing COCs (so-called third generation COCs). In the case-control study, however, the number of Yasmin cases was very small (1.2% of all cases) making the risk estimates unreliable. The relative risk for Yasmin users in the retrospective cohort study was greater than that for users of other COC products when considering women who used the products for less than one year. However, these one-year estimates may not be reliable because the analysis may include women of varying risk levels. Among women who used the product for 1 to 4 years, the relative risk was similar for users of Yasmin to that for users of other COC products.
c. Cerebrovascular Diseases
Oral contraceptives have been shown to increase both the relative and attributable risks of cerebrovascular events (thrombotic and hemorrhagic strokes), although, in general, the risk is greatest among older (>35 years), hypertensive women who also smoke. Hypertension was found to be a risk factor, for both users and nonusers, for both types of strokes, while smoking interacted to increase the risk for hemorrhagic strokes.
In a large study, the relative risk of thrombotic strokes has been shown to range from 3 for normotensive users to 14 for users with severe hypertension. The relative risk of hemorrhagic stroke is reported to be 1.2 for nonsmokers who used oral contraceptives, 2.6 for smokers who did not use oral contraceptives, 7.6 for smokers who used oral contraceptives, 1.8 for normotensive users and 25.7 for users with severe hypertension. The attributable risk is also greater in older women. Oral contraceptives also increase the risk for stroke in women with other underlying risk factors such as certain inherited or acquired thrombophilias, hyperlipidemias, and obesity. Women with migraine (particularly migraine with aura) who take combination oral contraceptives may be at an increased risk of stroke.
d. Dose-Related Risk of Vascular Disease From Oral Contraceptives
A positive association has been observed between the amount of estrogen and progestogen in oral contraceptives and the risk of vascular disease. A decline in serum high-density lipoproteins (HDL) has been reported with many progestational agents. A decline in serum high-density lipoproteins has been associated with an increased incidence of ischemic heart disease. Because estrogens increase HDL cholesterol, the net effect of an oral contraceptive depends on a balance achieved between doses of estrogen and progestogen and the nature and absolute amount of progestogen used in the contraceptive. The amount of both hormones should be considered in the choice of an oral contraceptive.
Minimizing exposure to estrogen and progestogen is in keeping with good principles of therapeutics. For any particular estrogen/progestogen combination, the dosage regimen prescribed should be one which contains the least amount of estrogen and progestogen that is compatible with a low failure rate and the needs of the individual patient. New acceptors of oral contraceptive agents should be started on preparations containing the lowest estrogen content that is judged appropriate for the individual patient.
e. Persistence of Risk of Vascular Disease
There are two studies which have shown persistence of risk of vascular disease for ever-users of oral contraceptives. In a study in the United States, the risk of developing myocardial infarction after discontinuing oral contraceptives persists for at least 9 years for women aged 40 to 49 years who had used oral contraceptives for five or more years, but this increased risk was not demonstrated in other age groups. In another study in Great Britain, the risk of developing cerebrovascular disease persisted for at least 6 years after discontinuation of oral contraceptives, although excess risk was very small. However, both studies were performed with oral contraceptive formulations containing 50 micrograms or higher of estrogens.
2. Estimates of Mortality From Contraceptive Use
One study gathered data from a variety of sources which have estimated the mortality rate associated with different methods of contraception at different ages (Table V). These estimates include the combined risk of death associated with contraceptive methods plus the risk attributable to pregnancy in the event of method failure. Each method of contraception has its specific benefits and risks. The study concluded that with the exception of oral contraceptive users 35 and older who smoke and 40 and older who do not smoke, mortality associated with all methods of birth control is below that associated with childbirth.
The observation of a possible increase in risk of mortality with age for oral contraceptive users is based on data gathered in the 1970's - but not reported until 1983. However, current clinical practice involves the use of lower estrogen dose formulations combined with careful restriction of oral contraceptive use to women who do not have the various risk factors uled in this labeling.
Because of these changes in practice and, also, because of some limited new data which suggest that the risk of cardiovascular disease with the use of oral contraceptives may now be less than previously observed, the Fertility and Maternal Health Drugs Advisory Committee was asked to review the topic in 1989. The Committee concluded that although cardiovascular disease risks may be increased with oral contraceptive use after age 40 in healthy nonsmoking women (even with the newer low-dose formulations), there are greater potential health risks associated with pregnancy in older women and with the alternative surgical and medical procedures which may be necessary if such women do not have access to effective and acceptable means of contraception.
Therefore, the Committee recommended that the benefits of oral contraceptive use by healthy nonsmoking women over 40 may outweigh the possible risks. Of course, women of all ages who take oral contraceptives should take the lowest possible dose formulation that is effective.
TABLE V: ANNUAL NUMBER OF BIRTH-RELATED OR METHOD-RELATED DEATHS ASSOCIATED WITH CONTROL OF FERTILITY PER 100,000 NONSTERILE WOMEN, BY FERTILITY-CONTROL METHOD ACCORDING TO AGE Adapted from H.W. Ory, Family Planning Perspectives, 15:57-63, 1983. Method of Control and Outcome 15 to 19 years 20 to 24 years 25 to 29 years 30 to 34 years 35 to 39 years 40 to 44 years No fertility control methods Deaths are birth-related 7 7.4 9.1 14.8 25.7 28.2 Oral contraceptives non-smoker Deaths are method-related 0.3 0.5 0.9 1.9 13.8 31.6 Oral contraceptives smoker 2.2 3.4 6.6 13.5 51.1 117.2 IUD 0.8 0.8 1 1 1.4 1.4 Condom 1.1 1.6 0.7 0.2 0.3 0.4 Diaphragm/spermicide 1.9 1.2 1.2 1.3 2.2 2.8 Periodic abstinence 2.5 1.6 1.6 1.7 2.9 3.6 3. Carcinoma of the Reproductive Organs and Breasts
Numerous epidemiological studies have been performed on the incidence of breast, endometrial, ovarian and cervical cancer in women using oral contraceptives.
Although the risk of having breast cancer diagnosed may be slightly increased among current and recent users of combined oral contraceptives (RR=1.24), this excess risk decreases over time after combination oral contraceptive discontinuation and by 10 years after cessation the increased risk disappears. The risk does not increase with duration of use and no consistent relationships have been found with dose or type of steroid. The patterns of risk are also similar regardless of a woman's reproductive history or her family breast cancer history. The subgroup for whom risk has been found to be significantly elevated is women who first used oral contraceptives before age 20, but because breast cancer is so rare at these young ages, the number of cases attributable to this early oral contraceptive use is extremely small.
Breast cancers diagnosed in current or previous OC users tend to be less clinically advanced than in never users.
Women who currently have or have had breast cancer should not use oral contraceptives because breast cancer is a hormonally-sensitive tumor.
Some studies suggest that oral contraceptive use has been associated with an increase in the risk of cervical intraepithelial neoplasia in some populations of women. However, there continues to be controversy about the extent to which such findings may be due to differences in sexual behavior and other factors.
In spite of many studies of the relationship between oral contraceptive use and breast and cervical cancers, a cause-and-effect relationship has not been established.
4. Hepatic Neoplasia
Benign hepatic adenomas are associated with oral contraceptive use, although the incidence of benign tumors is rare in the United States. Indirect calculations have estimated the attributable risk to be in the range of 3.3 cases/100,000 for users, a risk that increases after four or more years of use. Rupture of rare, benign, hepatic adenomas may cause death through intra-abdominal hemorrhage.
Studies from Britain have shown an increased risk of developing hepatocellular carcinoma in long-term (>8 years) oral contraceptive users. However, these cancers are extremely rare in the U.S. and the attributable risk (the excess incidence) of liver cancers in oral contraceptive users approaches less than one per million users.
5. Ocular Lesions
There have been clinical case reports of retinal thrombosis associated with the use of oral contraceptives, which may lead to partial or complete loss of vision. Oral contraceptives should be discontinued if there is unexplained partial or complete loss of vision; onset of proptosis or diplopia; papilledema; or retinal vascular lesions. Appropriate diagnostic and therapeutic measures should be undertaken immediately.
6. Oral Contraceptive Use Before or During Early Pregnancy
Extensive epidemiological studies have revealed no increased risk of birth defects in women who have used oral contraceptives prior to pregnancy. Studies also do not suggest a teratogenic effect, particularly in so far as cardiac anomalies and limb-reduction defects are concerned, when taken inadvertently during early pregnancy.
The administration of oral contraceptives to induce withdrawal bleeding should not be used as a test for pregnancy. Oral contraceptives should not be used during pregnancy to treat threatened or habitual abortion. (See CONTRAINDICATIONS)
It is recommended that for any patient who has missed two consecutive periods, pregnancy should be ruled out. If the patient has not adhered to the prescribed dosing schedule, the possibility of pregnancy should be considered at the time of the first missed period. Oral contraceptive use should be discontinued if pregnancy is confirmed.
7. Gallbladder Disease
Earlier studies have reported an increased lifetime relative risk of gallbladder surgery in users of oral contraceptives and estrogens. More recent studies, however, have shown that the relative risk of developing gallbladder disease among oral contraceptive users may be minimal. The recent findings of minimal risk may be related to the use of oral contraceptive formulations containing lower hormonal doses of estrogens and progestogens.
8. Carbohydrate and Lipid Metabolic Effects
Oral contraceptives have been shown to cause glucose intolerance in a significant percentage of users. Oral contraceptives containing greater than 75 micrograms of estrogens cause hyperinsulinism, while lower doses of estrogen cause less glucose intolerance. Progestogens increase insulin secretion and create insulin resistance, this effect varying with different progestational agents. However, in the nondiabetic woman, oral contraceptives appear to have no effect on fasting blood glucose. Because of these demonstrated effects, prediabetic and diabetic women should be carefully observed while taking oral contraceptives.
A small proportion of women will have persistent hypertriglyceridemia while on the pill. As discussed earlier (see WARNINGSÂ 1a. and 1d.), changes in serum triglycerides and lipoprotein levels have been reported in oral contraceptive users.
9. Elevated Blood Pressure
Women with severe hypertension should not be started on hormonal contraceptives (see CONTRAINDICATIONS).
An increase in blood pressure has been reported in women taking oral contraceptives and this increase is more likely in older oral contraceptive users and with continued use. Data from the Royal College of General Practitioners and subsequent randomized trials have shown that the incidence of hypertension increases with increasing concentrations of progestogens.
Women with a history of hypertension or hypertension-related diseases, or renal disease should be encouraged to use another method of contraception. If women with hypertension elect to use oral contraceptives, they should be monitored closely, and if significant elevation of blood pressure occurs, oral contraceptives should be discontinued. For most women, elevated blood pressure will return to normal after stopping oral contraceptives and there is no difference in the occurrence of hypertension among ever- and never-users.
10. Headache
The onset or exacerbation of migraine or development of headache with a new pattern which is recurrent, persistent or severe requires discontinuation of oral contraceptives and evaluation of the cause.
11. Bleeding Irregularities
Breakthrough bleeding and spotting are sometimes encountered in patients on oral contraceptives, especially during the first three months of use. Nonhormonal causes should be considered and adequate diagnostic measures taken to rule out malignancy or pregnancy in the event of breakthrough bleeding, as in the case of any abnormal vaginal bleeding. If pathology has been excluded, time or a change to another formulation may solve the problem. In the event of amenorrhea, pregnancy should be ruled out.
Some women may encounter post-pill amenorrhea or oligomenorrhea, especially when such a condition was pre-existent.
Precautions
1. General
Patients should be counseled that this product does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
2. Physical Examination and Follow-Up
A periodic personal and family medical history and complete physical examination are appropriate for all women, including women using oral contraceptives. The physical examination, however, may be deferred until after initiation of oral contraceptives if requested by the woman and judged appropriate by the clinician. The physical examination should include special reference to blood pressure, breasts, abdomen and pelvic organs, including cervical cytology and relevant laboratory tests. In case of undiagnosed, persistent or recurrent abnormal vaginal bleeding, appropriate measures should be conducted to rule out malignancy. Women with a strong family history of breast cancer or who have breast nodules should be monitored with particular care.
3. Lipid Disorders
Women who are being treated for hyperlipidemias should be followed closely if they elect to use oral contraceptives. Some progestogens may elevate LDL levels and may render the control of hyperlipidemias more difficult. (See WARNINGS 1d.)
In patients with familial defects of lipoprotein metabolism receiving estrogen-containing preparations, there have been case reports of significant elevations of plasma triglycerides leading to pancreatitis.
4. Liver Function
If jaundice develops in any woman receiving oral contraceptives, the medication should be discontinued. Steroid hormones may be poorly metabolized in patients with impaired liver function.
5. Fluid Retention
Oral contraceptives may cause some degree of fluid retention. They should be prescribed with caution, and only with careful monitoring, in patients with conditions which might be aggravated by fluid retention.
6. Emotional Disorders
Women with a history of depression should be carefully observed and the drug discontinued if depression recurs to a serious degree.
Patients becoming significantly depressed while taking oral contraceptives should stop the medication and use an alternate method of contraception in an attempt to determine whether the symptom is drug related.
7. Contact Lenses
Contact lens wearers who develop visual changes or changes in lens tolerance should be assessed by an ophthalmologist.
8. Drug Interactions
Effects of Other Drugs on Combined Hormonal Contraceptives
Rifampin: Metabolism of ethinyl estradiol and some progestins (e.g., norethindrone) is increased by rifampin. A reduction in contraceptive effectiveness and an increase in menstrual irregularities have been associated with concomitant use of rifampin.
Minocycline: Minocycline-related changes in estradiol, progesterone, FSH and LH plasma levels, breakthrough bleeding, or contraceptive failure cannot be ruled out.
Anticonvulsants: Anticonvulsants such as phenobarbital, phenytoin, and carbamazepine have been shown to increase the metabolism of ethinyl estradiol and/or some progestins, which could result in a reduction of contraceptive effectiveness.
Antibiotics: Pregnancy while taking combined hormonal contraceptives has been reported when the combined hormonal contraceptives were administered with antimicrobials such as ampicillin, tetracycline, and griseofulvin. However, clinical pharmacokinetic studies have not demonstrated any consistent effects of antibiotics (other than rifampin-see above) on plasma concentrations of synthetic steroids. See also separate discussion on minocycline (above).
Atorvastatin: Coadministration of atorvastatin and an oral contraceptive increased AUC values for norethindrone and ethinyl estradiol by approximately 30% and 20%, respectively.
St. John’s Wort: Herbal products containing St. John’s Wort (hypericum perforatum) may induce hepatic enzymes (cytochrome P450) and p-glycoprotein transporter and may reduce the effectiveness of oral contraceptives and emergency contraceptive pills. This may also result in breakthrough bleeding.
Other: Ascorbic acid and acetaminophen may increase plasma concentrations of some synthetic estrogens, possibly by inhibition of conjugation.
Effects of Drospirenone on Other Drugs
Metabolic Interactions
Metabolism of DRSP and potential effects of DRSP on hepatic cytochrome P450 (CYP) enzymes have been investigated in in vitro and in vivo studies (see Metabolism). In in vitro studies DRSP did not affect turnover of model substrates of CYP1A2 and CYP2D6, but had an inhibitory influence on the turnover of model substrates of CYP1A1, CYP2C9, CYP2C19 and CYP3A4 with CYP2C19 being the most sensitive enzyme. The potential effect of DRSP on CYP2C19 activity was investigated in a clinical pharmacokinetic study using omeprazole as a marker substrate. In the study with 24 postmenopausal women [including 12 women with homozygous (wild type) CYP2C19 genotype and 12 women with heterozygous CYP2C19 genotype] the daily oral administration of 3 mg DRSP for 14 days did not affect the oral clearance of omeprazole (40 mg, single oral dose) and the CYP2C19 product 5-hydroxy omeprazole. Furthermore, no significant effect of DRSP on the systemic clearance of the CYP3A4 product omeprazole sulfone was found. These results demonstrate that DRSP did not inhibit CYP2C19 and CYP3A4 in vivo.
Two additional clinical drug-drug interaction studies using simvastatin and midazolam as marker substrates for CYP3A4 were each performed in 24 healthy postmenopausal women. The results of these studies demonstrated that pharmacokinetics of the CYP3A4 substrates were not influenced by steady-state DRSP concentrations achieved after administration of 3 mg DRSP/day.
Interactions with Drugs that Have the Potential to Increase Serum Potassium
There is a potential for an increase in serum potassium in women taking drospirenone and ethinyl estradiol tablets with other drugs (see BOLDED WARNING). Of note, occasional or chronic use of NSAID medication was not restricted in any of the clinical trials with 3 mg DRSP/0.03 mg EE tablets.
A drug-drug interaction study of DRSP 3 mg/estradiol (E2) 1 mg versus placebo was performed in 24 mildly hypertensive postmenopausal women taking enalapril maleate 10 mg twice daily. Potassium levels were obtained every other day for a total of 2 weeks in all subjects. Mean serum potassium levels in the DRSP/E2 treatment group relative to baseline were 0.22 mEq/L higher than those in the placebo group. Serum potassium concentrations also were measured at multiple timepoints over 24 hours at baseline and on Day 14. On Day 14, the ratios for serum potassium Cmax and AUC in the DRSP/E2 group to those in the placebo group were 0.955 (90% CI: 0.914, 0.999) and 1.01 (90% CI: 0.944, 1.08), respectively. No patient in either treatment group developed hyperkalemia (serum potassium concentrations >5.5 mEq/L).
Effects of Combined Hormonal Contraceptives on Other Drugs
Combined oral contraceptives containing ethinyl estradiol may inhibit the metabolism of other compounds. Increased plasma concentrations of cyclosporine, prednisolone, and theophylline have been reported with concomitant administration of oral contraceptives. In addition, oral contraceptives may induce the conjugation of other compounds. Decreased plasma concentrations of acetaminophen and increased clearance on temazepam, salicylic acid, morphine, and clofibric acid have been noted when these drugs were administered with oral contraceptives.
9. Interactions with Laboratory Tests
Certain endocrine- and liver-function tests and blood components may be affected by oral contraceptives:
- Increased prothrombin and factors VII, VIII, IX and X; decreased antithrombin 3; increased norepinephrine-induced platelet aggregability.
- Increased thyroid-binding globulin (TBG) leading to increased circulating total thyroid hormone, as measured by protein-bound iodine (PBI), T4 by column or by radioimmunoassay. Free T3 resin uptake is decreased, reflecting the elevated TBG, free T4 concentration is unaltered.
- Other binding proteins may be elevated in serum.
- Sex-hormone-binding globulins are increased and result in elevated levels of total circulating sex steroids and corticoids; however, free or biologically active levels remain unchanged.
- Triglycerides may be increased.
- Glucose tolerance may be decreased.
- Serum folate levels may be depressed by oral contraceptive therapy. This may be of clinical significance if a woman becomes pregnant shortly after discontinuing oral contraceptives.
10. Carcinogenesis, Mutagenesis, Impairment of Fertility
In a 24 month oral carcinogenicity study in mice dosed with 10 mg/kg/day drospirenone alone or 1 + 0.01, 3 + 0.03 and 10 + 0.1 mg/kg/day of drospirenone and ethinyl estradiol, 0.1 to 2 times the exposure (AUC of drospirenone) of women taking a contraceptive dose, there was an increase in carcinomas of the harderian gland in the group that received the high dose of drospirenone alone. In a similar study in rats given 10 mg/kg/day drospirenone alone or 0.3 + 0.003, 3 + 0.03 and 10 + 0.1 mg/kg/day drospirenone and ethinyl estradiol, 0.8 to 10 times the exposure of women taking a contraceptive dose, there was an increased incidence of benign and total (benign and malignant) adrenal gland pheochromocytomas in the group receiving the high dose of drospirenone. Drospirenone was not mutagenic in a number of in vitro (Ames, Chinese Hamster Lung gene mutation and chromosomal damage in human lymphocytes) and in vivo (mouse micronucleus) genotoxicity tests. Drospirenone increased unscheduled DNA synthesis in rat hepatocytes and formed adducts with rodent liver DNA but not with human liver DNA. (See WARNINGS).
11. Pregnancy
Pregnancy Category X.
Estrogens and progestins should not be used during pregnancy. Fourteen pregnancies that occurred during exposure with 3 mg DRSP/0.03 mg EE tablets in utero (none with more than a single cycle of exposure) have been identified. One infant was born with esophageal atresia. A causal association with the 3 mg DRSP/0.03 mg EE tablet is unknown.
Twelve pregnancies that occurred with drospirenone and ethinyl estradiol tablets exposure in utero (none with more than a single cycle of exposure) have been identified. There were no known cases of congenital anomalies.
A teratology study in pregnant rats given drospirenone orally at doses of 5, 15 and 45 mg/kg/day, 6 to 50 times the human exposure based on AUC of drospirenone, resulted in an increased number of fetuses with delayed ossification of bones of the feet in the two higher doses. A similar study in rabbits dosed orally with 1, 30 and 100 mg/kg/day drospirenone, 2 to 27 times the human exposure, resulted in an increase in fetal loss and retardation of fetal development (delayed ossification of small bones, multiple fusions of ribs) at the high dose only. When drospirenone was administered with ethinyl estradiol (100:1) during late pregnancy (the period of genital development) at doses of 5, 15 and 45 mg/kg, there was a dose dependent increase in feminization of male rat fetuses. In a study in 36 cynomolgous monkeys, no teratogenic or feminization effects were observed with orally administered drospirenone and ethinyl estradiol (100:1) at doses up to 10 mg/kg/day drospirenone, 30 times the human exposure.
12. Nursing Mothers
Small amounts of oral contraceptive steroids have been identified in the milk of nursing mothers, and a few adverse effects on the child have been reported, including jaundice and breast enlargement. In addition, oral contraceptives given in the postpartum period may interfere with lactation by decreasing the quantity and quality of breast milk. If possible, the nursing mother should be advised not to use oral contraceptives but to use other forms of contraception until she has completely weaned her child.
After oral administration of 3 mg DRSP/0.03 mg EE tablets about 0.02% of the drospirenone dose was excreted into the breast milk of postpartum women within 24 hours. This results in a maximal daily dose of about 3 mcg drospirenone in an infant.
13. Pediatric Usage
Safety and efficacy of drospirenone and ethinyl estradiol tablets has been established in women of reproductive age. Safety and efficacy are expected to be the same for post-pubertal adolescents under the age of 16 and for users 16 years and older. Use of this product before menarche is not indicated.
Information for the Patient
See “Patient Labeling” printed below.
Adverse Reactions
An increased risk of the following serious adverse reactions has been associated with the use of oral contraceptives (see WARNINGS).
- Thrombophlebitis
- Arterial thromboembolism
- Pulmonary embolism
- Myocardial infarction
- Cerebral hemorrhage
- Cerebral thrombosis
- Hypertension
- Gallbladder disease
- Hepatic adenomas or benign liver tumors
There is evidence of an association between the following conditions and the use of oral contraceptives:
- Mesenteric thrombosis
- Retinal thrombosis
The following adverse reactions have been reported in patients receiving oral contraceptives and are believed to be drug-related:
- Nausea
- Vomiting
- Gastrointestinal symptoms (such as abdominal cramps and bloating)
- Breakthrough bleeding
- Spotting
- Change in menstrual flow
- Amenorrhea
- Temporary infertility after discontinuation of treatment
- Edema
- Melasma which may persist
- Breast changes: tenderness, enlargement, secretion
- Change in weight or appetite (increase or decrease)
- Change in cervical ectropion and secretion
- Possible diminution in lactation when given immediately postpartum
- Cholestatic jaundice
- Migraine
- Rash (allergic)
- Mood changes, including depression
- Reduced tolerance to carbohydrates
- Vaginitis, including candidiasis
- Change in corneal curvature (steepening)
- lntolerance to contact lenses
- Decrease in serum folate levels
- Exacerbation of systemic lupus erythematosus
- Exacerbation of porphyria
- Exacerbation of chorea
- Aggravation of varicose veins
- Anaphylactic/anaphylactoid reactions, including urticaria, angioedema, and severe reactions with respiratory and circulatory symptoms
The following adverse reactions have been reported in users of oral contraceptives and a causal association has been neither confirmed nor refuted:
- Acne
- Budd-Chiari syndrome
- Cataracts
- Changes in libido
- Colitis
- Cystitis-like syndrome
- Dizziness
- Dysmenorrhea
- Erythema multiforme
- Erythema nodosum
- Headache
- Hemolytic uremic syndrome
- Hemorrhagic eruption
- Hirsutism
- Impaired renal function
- Loss of scalp hair
- Nervousness
- Optic neuritis, which may lead to partial or complete loss of vision
- Pancreatitis
- Pre-menstrual syndrome
The most frequent (> 1%) treatment-emergent adverse events, uled in descending order, reported with the use of drospirenone and ethinyl estradiol tablets in the contraception clinical trials, which may or may not be drug related, included: upper respiratory infection, headache, breast pain, vaginal moniliasis, leukorrhea, diarrhea, nausea, vomiting, vaginitis, abdominal pain, flu syndrome, dysmenorrhea, moniliasis, allergic reaction, urinary tract infection, accidental injury, cystitis, tooth disorder, sore throat, infection, fever, surgery, sinusitis, back pain, emotional lability, migraine, suspicious Papanicolaou smear, dyspepsia, rhinitis, acne, gastroenteritis, bronchitis, pharyngitis, skin disorder, intermenstrual bleeding, decreased libido, weight gain, pain, depression, increased cough, dizziness, menstrual disorder, pain in extremity, pelvic pain, and asthenia.
The most frequent (> 1%) treatment-emergent adverse events, uled in descending order, reported with the use of drospirenone and ethinyl estradiol tablets in the acne clinical trials, which may or not be drug related, included: upper respiratory infection, metrorrhagia, headache, suspicious Papanicolaou smear, nausea, sinusitis, vaginal moniliasis, flu syndrome, menorrhagia, depression, emotional lability, abdominal pain, gastroenteritis, urinary tract infection, tooth disorder, infection, vomiting, pharyngitis, breast pain, dysmenorrhea, menstrual disorder, accidental injury, asthenia, sore throat, weight gain, arthralgia, bronchitis, rhinitis, amenorrhea, and urine abnormality.
Overdosage
Serious ill effects have not been reported following acute ingestion of large doses of other oral contraceptives by young children. Overdosage may cause nausea, and withdrawal bleeding may occur in females. Drospirenone, however, is a spironolactone analogue which has antimineralocorticoid properties. Serum concentration of potassium and sodium, and evidence of metabolic acidosis, should be monitored in cases of overdose.
Non-contraceptive Health Benefits
The following non-contraceptive health benefits related to the use of oral contraceptives are supported by epidemiological studies which largely utilized oral contraceptive formulations containing doses exceeding 0.035 mg of ethinyl estradiol or 0.05 mg mestranol.
Effects on menses:
- increased menstrual cycle regularity
- decreased blood loss and decreased incidence of iron-deficiency anemia
- decreased incidence of dysmenorrhea
Effects related to inhibition of ovulation:
- decreased incidence of functional ovarian cysts
- decreased incidence of ectopic pregnancies
Effects from long-term use:
- decreased incidence of fibroadenomas and fibrocystic disease of the breast
- decreased incidence of acute pelvic inflammatory disease
- decreased incidence of endometrial cancer
- decreased incidence of ovarian cancer
Dosage And Administration
Oral Contraception
To achieve maximum contraceptive effectiveness, Gianvi tablets must be taken exactly as directed at intervals not exceeding 24 hours.
Gianvi tablets consist of 24 pink active tablets of a monophasic combined hormonal preparation plus 4 inert white tablets. The dosage of Gianvi tablets is one pink tablet daily for 24 consecutive days followed by 4 white inert tablets per menstrual cycle. A patient should begin to take Gianvi tablets either on the first day of her menstrual period (Day 1 Start) or on the first Sunday after the onset of her menstrual period (Sunday Start).
Day 1 Start
During the first cycle of Gianvi tablet use, the patient should be instructed to take one pink Gianvi tablet daily, beginning on Day one (1) of her menstrual cycle. (The first day of menstruation is Day one.) She should take one pink Gianvi tablet daily for 24 consecutive days, followed by one white inert tablet daily on menstrual cycle days 25 through 28. It is recommended that Gianvi tablets be taken at the same time each day, preferably after the evening meal or at bedtime. Gianvi tablets can be taken without regard to meals. If Gianvi tablets are first taken later than the first day of the menstrual cycle, Gianvi tablets should not be considered effective as a contraceptive until after the first 7 consecutive days of product administration. The possibility of ovulation and conception prior to initiation of medication should be considered.
Sunday Start
During the first cycle of Gianvi tablet use, the patient should be instructed to take one pink Gianvi tablet daily, beginning on the first Sunday after the onset of her menstrual period. She should take one pink Gianvi tablet daily for 24 consecutive days, followed by one white inert tablet daily on menstrual cycle days 25 through 28. It is recommended that Gianvi tablets be taken at the same time each day, preferably after the evening meal or at bedtime. Gianvi tablets can be taken without regard to meals. Gianvi tablets should not be considered effective as a contraceptive until after the first 7 consecutive days of product administration. The possibility of ovulation and conception prior to initiation of medication should be considered.
The patient should begin her next and all subsequent 28-day regimens of Gianvi tablets on the same day of the week that she began her first regimen, following the same schedule. She should begin taking her pink tablets on the next day after ingestion of the last white tablet, regardless of whether or not a menstrual period has occurred or is still in progress. Anytime a subsequent cycle of Gianvi tablets is started later than the day following administration of the last white tablet, the patient should use another method of contraception until she has taken a pink Gianvi tablet daily for seven consecutive days.
When switching from another oral contraceptive, Gianvi tablets should be started on the same day that a new pack of the previous oral contraceptive would have been started.
Withdrawal bleeding usually occurs within 3 days following the last pink tablet. If spotting or breakthrough bleeding occurs while taking Gianvi, the patient should be instructed to continue taking her Gianvi tablets as instructed and by the regimen described above. She should be instructed that this type of bleeding is usually transient and without significance; however, if the bleeding is persistent or prolonged, the patient should be advised to consult her physician.
Although the occurrence of pregnancy is low if Gianvi tablets are taken according to directions, if withdrawal bleeding does not occur, the possibility of pregnancy must be considered. If the patient has not adhered to the prescribed dosing schedule (missed one or more active tablets or started taking them on a day later than she should have), the possibility of pregnancy should be considered at the time of the first missed period and appropriate diagnostic measures taken. If the patient has adhered to the prescribed regimen and misses two consecutive periods, pregnancy should be ruled out. Hormonal contraceptives should be discontinued if pregnancy is confirmed.
The risk of pregnancy increases with each active pink tablet missed. For additional patient instructions regarding missed pills, see the “WHAT TO DO IF YOU MISS PILLS” section in the DETAILED PATIENT LABELING, which follows. If breakthrough bleeding occurs following missed tablets, it will usually be transient and of no consequence. If the patient misses one or more white tablets, she should still be protected against pregnancy provided she begins taking pink tablets again on the proper day.
In the nonlactating mother, Gianvi tablets may be initiated 4 to 6 weeks postpartum, for contraception. When the tablets are administered in the postpartum period, the increased risk of thromboembolic disease associated with the postpartum period must be considered. (See CONTRAINDICATIONS, WARNINGS, and PRECAUTIONS concerning thromboembolic disease.)
Acne
The timing and initiation of dosing with Gianvi tablets in women with acne should follow the guideline for use of Gianvi tablets as an oral contraceptive. The 28-day dosage regimen for Gianvi tablets for treating facial acne consists of one active tablet daily for 24 consecutive days followed by one inert tablet daily for 4 days. After 28 tablets are taken, a new course is started the next day.
How Supplied
Gianvi™ (drospirenone and ethinyl estradiol tablets) 3 mg/0.02 mg – 28-Day Regimen are available in 1 buler pack (NDC 54868-6162-0).
Each buler card contains 24 active pink, round, unscored, film-coated tablets, debossed with stylized b on one side and 257 on the other side, each containing 3 mg of drospirenone and 0.02 mg of ethinyl estradiol, and 4 inert white, round, unscored tablets debossed with stylized b on one side and 208 on the other side.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Store at 20Âş to 25ÂşC (68Âş to 77ÂşF) [See USP Controlled Room Temperature].
References
1. Dinger JC, Heinemann LAJ, et al: The safety of a drospirenone-containing oral contraceptive: final results from the European active surveillance study on oral contraceptives based on 142,475 women-years of observation. Contraception 2007;75:344-354.
2. Seeger JD, Loughlin J, Eng PM, et al: Risk of thromboembolism in women taking ethinyl estradiol/drospirenone and other oral contraceptives. Obstetrics & Gynecology 2007;110(3):587-593.
3. van Hylckama Vlieg A, Helmerhorst FM, Vandenbroucke JP, et al: The venous thrombotic risk of oral contraceptives, effects of oestrogen dose and progestogen type: results of the MEGA case-control study. BMJ 2009;339:b2921.
4. Lidegaard O, Lokkegaard E, Svendsen AL, et al: Hormonal contraception and risk of venous thromboembolism: national follow-up study. BMJ 2009; 339:b2890.
Brief Summary Patient Package Insert
Gianvi™ (drospirenone and ethinyl estradiol tablets)
containing the following:
24 pink - “active” tablets
4 white – “inert” tablets
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Gianvi™ (drospirenone and ethinyl estradiol tablets) is different from other birth control pills because it contains the progestin drospirenone. Drospirenone may increase potassium. Therefore, you should not take drospirenone and ethinyl estradiol tablets if you have kidney, liver or adrenal disease because this could cause serious heart and health problems. Other drugs may also increase potassium. If you are currently on daily, long-term treatment for a chronic condition with any of the medications below, you should consult your healthcare provider about whether drospirenone and ethinyl estradiol tablets is right for you, and during the first month that you take drospirenone and ethinyl estradiol tablets, you should have a blood test to check your potassium level.
- NSAIDs (ibuprofen [Motrin*, Advil*], naprosyn [Aleve* and others] when taken long-term and daily for treatment of arthritis or other problems)
- Potassium-sparing diuretics (spironolactone and others)
- Potassium supplementation
- ACE inhibitors (Capoten*, Vasotec*, Zestril* and others)
- Angiotensin-II receptor antagonists (Cozaar*, Diovan*, Avapro* and others)
- Heparin
- Aldosterone antagonists
Gianvi™ (drospirenone and ethinyl estradiol tablets) is an oral contraceptive, also known as a “birth control pill” or “the pill.” Oral contraceptives are taken to prevent pregnancy, and, when taken correctly without missing any pills, have a failure rate of approximately 1% per year (1 pregnancy per 100 women per year of use). The typical failure rate in pill users is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. Forgetting to take pills considerably increases the chances of pregnancy.
Gianvi™ (drospirenone and ethinyl estradiol tablets) may also be taken to treat moderate acne in women who are able to and wish to use the pill for birth control.
Any woman who needs contraception (birth control) and chooses to use an oral contraceptive should understand the benefits and risks of using the pill. This leaflet will give you much of the information you will need to help you decide if you should use the pill for contraception and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this leaflet is not a replacement for a careful discussion between you and your healthcare professional. You should discuss the information provided in this leaflet with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare professional’s advice with regard to regular check-ups while you are on the pill.
For the majority of women, oral contraceptives can be taken safely. But there are some women who are at high risk of developing certain serious diseases that can be life-threatening or may cause temporary or permanent disability or death. The risks associated with taking oral contraceptives increase significantly if you:
- smoke
- have high blood pressure, diabetes, high cholesterol, or are obese
- have or have had clotting disorders, heart attack, stroke, angina pectoris (severe chest pains), cancer of the breast or sex organs, jaundice, or malignant or benign liver tumors.
You should not take the pill if you suspect you are pregnant or have unexplained vaginal bleeding.
Although cardiovascular disease risks may be increased with oral contraceptive use after age 40 in healthy, non-smoking women (even with the newer low-dose formulations), there are also greater potential health risks associated with pregnancy in older women.
Boxed Warning section
Cigarette smoking increases the risk of serious adverse effects on the heart and blood vessels from oral contraceptive use. This risk increases with age and with heavy smoking (15 or more cigarettes per day) and is quite marked in women over 35 years of age. Women who use oral contraceptives should not smoke.
Most side effects of the pill are not serious. The most common such effects are nausea, vomiting, bleeding between menstrual periods, weight gain, breast tenderness, and difficulty wearing contact lenses. These side effects, especially nausea and vomiting may subside within the first three months of use.
The serious side effects of the pill occur very infrequently, especially if you are in good health and are young. However, you should know that the following medical conditions have been associated with or made worse by the pill:
1. Blood clots in the legs (thrombophlebitis), lungs (pulmonary embolism), blockage or rupture of a blood vessel in the brain (stroke), blockage of blood vessels in the heart (heart attack and angina pectoris) or other organs of the body. As mentioned above, smoking increases the risk of heart attacks and strokes and subsequent serious medical consequences. Women with migraine headaches also may be at increased risk of stroke when taking the pill.
2. Liver tumors, which may rupture and cause severe bleeding. A possible but not definite association has been found with the pill and liver cancer. However, liver cancers are extremely rare. The chance of developing liver cancer from using the pill is thus even rarer.
3. High blood pressure, although blood pressure usually returns to normal when the pill is stopped.
4. Cancer of the breast. Various studies give conflicting reports on the relationship between breast cancer and oral contraceptive use. Oral contraceptive use may slightly increase your chance of having breast cancer diagnosed, particularly after using hormonal contraceptives at a younger age. After you stop using hormonal contraceptives, the chances of getting breast cancer begin to go back down. You should have regular breast examinations by a healthcare provider and examine your own breasts monthly. Tell your healthcare provider if you have a family history of breast cancer or if you have had breast nodules or an abnormal mammogram. Women who currently have or have had breast cancer should not use oral contraceptives because breast cancer is a hormone-sensitive tumor.
Some studies have found an increase in the incidence of cancer or precancerous lesions of the cervix in women who use the pill. However, this finding may be related to factors other than the use of the pill.
The symptoms associated with these serious side effects are discussed in the detailed leaflet given to you with your supply of pills. Notify your doctor or healthcare provider if you notice any unusual physical disturbances while taking the pill. In addition, drugs such as rifampin, as well as some anticonvulsants, some antibiotics and some herbal products such as St. John’s Wort, may decrease oral contraceptive effectiveness.
Taking the pill may provide some important non-contraceptive benefits. These include less painful menstruation, less menstrual blood loss and anemia, fewer pelvic infections, and fewer cancers of the ovary and the lining of the uterus.
Be sure to discuss any medical condition you may have with your healthcare provider. Your healthcare provider will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare provider believes that it is appropriate to postpone it. You should be reexamined at least once a year while taking oral contraceptives. The detailed patient information booklet gives you further information, which you should read and discuss with your healthcare provider.
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against HIV infection (AIDS) and other sexually transmitted diseases such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
INSTRUCTIONS TO PATIENTS
HOW TO TAKE THE PILL
IMPORTANT POINTS TO REMEMBER
BEFORE YOU START TAKING YOUR PILLS:
1. BE SURE TO READ THESE DIRECTIONS:
- Before you start taking your pills.
- Anytime you are not sure what to do.
2. THE RIGHT WAY TO TAKE THE PILL IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME. GIANVI™ TABLETS CAN BE TAKEN WITHOUT REGARD TO MEALS.
If you miss pills you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant. See “WHAT TO DO IF YOU MISS PILLS” below.
3. MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1 TO 3 PACKS OF PILLS.
If you do have spotting or light bleeding or feel sick to your stomach, do not stop taking the pill. The problem will usually go away. If it does not go away, check with your healthcare provider.
4. MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills.
On the days you take two pills, to make up for missed pills, you could also feel a little sick to your stomach.
5. IF YOU HAVE VOMITING (within 3 to 4 hours after you take your pill), you should follow the instructions for “WHAT TO DO IF YOU MISS PILLS”. IF YOU HAVE DIARRHEA, or IF YOU TAKE CERTAIN MEDICINES, including some antibiotics and some herbal products such as St. John’s Wort, your pills may not work as well.
Use a back-up method (such as condoms or spermicides) until you check with your healthcare provider.
6. IF YOU HAVE TROUBLE REMEMBERING TO TAKE THE PILL, talk to your healthcare provider about how to make pill-taking easier or about using another method of birth control.
7. IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your healthcare provider.
BEFORE YOU START TAKING YOUR PILLS
1. DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL.
It is important to take Gianvi tablets at about the same time every day. Gianvi tablets can be taken without regard to meals.
2. LOOK AT YOUR PILL PACK: – IT HAS 28 PILLS:
The Gianvi tablets-pill pack has 24 pink “active” pills (with hormones) to be taken for 24 days, followed by 4 white “reminder” pills (without hormones) to be taken for four days.
3. ALSO FIND:
1) Where on the pack to start taking pills,
2) In what order to take the pills (follow the arrows)
3) The week numbers are shown on the buler card picture below

4. BE SURE YOU HAVE READY AT ALL TIMES:
ANOTHER KIND OF BIRTH CONTROL (such as condoms or spermicides) to use as a back-up in case you miss pills.
AN EXTRA, FULL PILL PACK.
WHEN TO START THE FIRSTÂ PACK OF PILLS
You have a choice for which day to start taking your first pack of pills. Decide with your healthcare provider, which is the best day for you. Pick a time of day, which will be easy to remember.
DAY 1 START:
1. Take the first pink “active” pill of the first pack during the first 24 hours of your period.
2. You will not need to use a back-up method of birth control, since you are starting the pill at the beginning of your period.
SUNDAY START:
1. Take the first pink “active” pill of the first pack on the Sunday after your period starts, even if you are still bleeding. If your period begins on Sunday, start the pack that same day.
2. Use another method of birth control (such as condoms or spermicides) as a back-up method if you have sex anytime from the Sunday you start your first pack until the next Sunday (7 days).
WHEN YOU SWITCH FROM A DIFFERENT BIRTH CONTROL PILL
When switching from another birth control pill, Gianvi tablets should be started on the same day that a new pack of the previous birth control pills would have been started.
WHAT TO DO DURING THE MONTH
1. TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY
Do not skip pills even if you are spotting or bleeding between monthly periods or feel sick to your stomach (nausea).
Do not skip pills even if you do not have sex very often.
2. WHEN YOU FINISH A PACK OF PILLS:
Start the next pack on the day after your last white “reminder” pill. Do not wait any days between packs.
WHAT TO DO IF YOU MISS PILLS
If you MISS 1 pink “active” pill in Week 1 of your pack:
1. Take it as soon as you remember. Take the next pill at your regular time. This means you may take two pills in one day.
2. You do not need to use a back-up birth control method if you have sex.
If you MISS 2 pink “active” pills in a row in WEEK 1 or WEEK 2 of your pack:
1. Take two pills on the day you remember and two pills the next day.
2. Then take one pill a day until you finish the pack.
3. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicides) as a back-up for those 7 days.
If you MISS 2 pink “active” pills in a row in WEEK 3 or WEEK 4 of your pack:
1 . If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
If you are a Sunday Starter:
Keep taking one pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
2. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicide) as a back-up for those 7 days.
3. You may not have your period this month but this is expected. However, if you miss your period two months in a row, call your healthcare provider because you might be pregnant.
If you MISS 3 OR MORE pink “active” pills in a row during ANY WEEK:
1. If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
If you are a Sunday Starter:
Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
2. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicides) as a back-up for those 7 days.
3. You may not have your period this month but this is expected. However, if you miss your period two months in a row, call your healthcare provider because you might be pregnant.
If you MISS ANY of the 4 white “reminder” pills in WEEK 4:
- THROW AWAY the pills you missed.
- Keep taking one pill each day until the pack is empty.
- You do not need a back-up method of birth control.
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED:
Use a BACK-UP METHOD (such as condoms or spermicides) anytime you have sex.
KEEP TAKING ONE ACTIVE PINK PILL EACH DAY until you can contact your healthcare provider.
For additional information see “Detailed Patient Labeling”
Detailed Patient Package Insert
This product (like all oral contraceptives) is intended to prevent pregnancy. Oral contraceptives do not protect against HIV infection (AIDS) and other sexually transmitted diseases.
Gianvi™ (drospirenone and ethinyl estradiol tablets) is different from other birth control pills because it contains the progestin drospirenone. Drospirenone may increase potassium. Therefore, you should not take drospirenone and ethinyl estradiol tablets if you have kidney, liver or adrenal disease because this could cause serious heart and health problems. Other drugs may also increase potassium. If you are currently on daily, long-term treatment for a chronic condition with any of the medications below, you should consult your healthcare provider about whether drospirenone and ethinyl estradiol tablets is right for you, and during the first month that you take drospirenone and ethinyl estradiol tablets, you should have a blood test to check your potassium level.
- NSAIDs (ibuprofen [Motrin*, Advil*], naprosyn [Aleve* and others] when taken long-term and daily for treatment of arthritis or other problems)
- Potassium-sparing diuretics (spironolactone and others)
- Potassium supplementation
- ACE inhibitors (Capoten*, Vasotec*, Zestril* and others)
- Angiotensin-II receptor antagonists (Cozaar*, Diovan*, Avapro* and others)
- Heparin
- Aldosterone antagonists
Gianvi™ (drospirenone and ethinyl estradiol tablets) is an oral contraceptive, also known as a “birth control pill” or “the pill”. Oral contraceptives are taken to prevent pregnancy, and, when taken correctly without missing any pills, have a failure rate of approximately 1% per year (1 pregnancy per 100 women per year of use). The typical failure rate in pill users is approximately 5% per year (5 pregnancies per 100 women per year of use) when women who miss pills are included. Forgetting to take pills considerably increases the chances of pregnancy.
Gianvi™ (drospirenone and ethinyl estradiol tablets) may also be taken to treat moderate acne in women who are able to and wish to use the pill for birth control.
INTRODUCTION
Any woman who needs contraception (birth control) and chooses to use an oral contraceptive should understand the benefits and risks of using the pill. This leaflet will give you much of the information you will need to help you decide if you should use the pill for contraception and will also help you determine if you are at risk of developing any of the serious side effects of the pill. It will tell you how to use the pill properly so that it will be as effective as possible. However, this leaflet is not a replacement for a careful discussion between you and your healthcare professional. You should discuss the information provided in this leaflet with him or her, both when you first start taking the pill and during your revisits. You should also follow your healthcare professional's advice with regard to regular check-ups while you are on the pill.
EFFECTIVENESS OF ORAL CONTRACEPTIVES
Oral contraceptives or “birth control pills” or “the pill” are used to prevent pregnancy and are more effective than most other nonsurgical methods of birth control. When they are taken correctly, the chance of becoming pregnant is less than 1% (one pregnancy per 100 women per year of use) when used perfectly, without missing any pills. Typical failure rates, including women who don’t always follow the instructions exactly, are about 5% per year. The chance of becoming pregnant increases with each missed pill during a menstrual cycle.
In comparison, typical failure rates for other nonsurgical methods of birth control during the first year of use are as follows:
PERCENTAGE OF WOMEN EXPERIENCING AN UNINTENDED PREGNANCY DURING THE FIRST YEAR OF TYPICAL USE AND FIRST YEAR OF PERFECT USE OF CONTRACEPTION AND THE PERCENTAGE CONTINUING USE AT THE END OF THE FIRST YEAR: UNITED STATES.
Â
Â% of Women Experiencing an Unintended Pregnancy Within the First Year of Use % of Women Continuing Use at One Year Method (1) Typical Use (2) Perfect Use (3) (4) Chance 85 85 Spermicides 26 6 40 Periodic abstinence 25 63 Calendar 9 Ovulation method 3 Sympto-thermal 2 Post-ovulation 1 Withdrawal 19 4 Cap With spermicidal cream or jelly. Parous women 40 26 42 Nulliparous women 20 9 56 Sponge Parous women 40 20 42 Nulliparous women 20 9 56 Diaphragm 20 6 56 Condom Female (Reality) 21 5 56 Male 14 3 61 Pill 5 71 progestin only 0.5 combined 0.1 IUD Progesterone T 2 1.5 81 Copper T 380A 0.8 0.6 78 Lng 20 0.1 0.1 81 Depo Provera 0.3 0.3 70 Norplant and Norplant-2 0.05 0.05 88 Female sterilization 0.5 0.5 100 Male sterilization 0.15 0.10 100 Emergency Contraceptive Pills: Treatment initiated within 72 hours after unprotected intercourse reduces the risk of pregnancy by at least 75%. Lactational Amenorrhea Method: LAM is highly effective, temporary method of contraception. Source: Trussell J, Contraceptive efficacy. In Hatcher RA, Trussell J, Stewart F, Cates W, Stewart GK, Guest F, Kowal D, Contraceptive Technology: Seventeenth Revised Edition. New York NY: Irvington Publishers, 1998.
 Gianvi™ (drospirenone and ethinyl estradiol tablets) may also be taken to treat moderate acne if all of the following are true:
- Your doctor says it is safe for you to use the pill.
- You are at least 14 years old.
- You have started having menstrual periods.
- You want to use the pill for birth control.
Â
 WHO SHOULD NOT TAKE ORAL CONTRACEPTIVES
Boxed Warning section
Cigarette smoking increases the risk of serious adverse effects on the heart and blood vessels from oral contraceptive use. This risk increases with age and with heavy smoking (15 or more cigarettes per day) and is quite marked in women over 35 years of age. Women who use oral contraceptives should not smoke.
Some women should not use Gianvi tablets. For example, you should not take Gianvi tablets if you are pregnant or think you may be pregnant. You should also not use Gianvi tablets if you have had any of the following conditions:
- A history of heart attack or stroke
- A history of blood clots in the legs (deep vein thrombosis), lungs (pulmonary embolism), or eyes (retinal thrombosis)
- Chest pain (angina pectoris)
- Known or suspected breast cancer or cancer of the lining of the uterus, cervix or vagina
- Unexplained vaginal bleeding (until a diagnosis is reached by your doctor)
- Yellowing of the whites of the eyes or of the skin (jaundice) during pregnancy or during previous use of the pill or other hormonal contraceptives
- Liver tumor (benign or cancerous)
- Known or suspected pregnancy
- Heart valve or heart rhythm disorders that may be associated with formation of blood clots
- Diabetes with complications of the kidneys, eyes, nerves, or blood vessels
- Severe high blood pressure
- A need for surgery with prolonged bedrest
- Headaches with neurological symptoms
- Allergy or hypersensitivity to any of the components of drospirenone and ethinyl estradiol tablets
In addition, you should not use Gianvi tablets if you have any of the following conditions:
- Kidney Disease
- Liver Disease
- Adrenal Disease
Tell your healthcare provider if you have ever had any of the above conditions (Your healthcare provider can recommend another method of birth control). If you are currently on daily, long-term treatment for a chronic condition with any of the following medications, you should consult your healthcare provider before taking Gianvi tablets:
- NSAIDs (ibuprofen, naprosyn and others)
- Potassium-sparing diuretics (spironolactone and others)
- Potassium supplementation
- ACE inhibitors (captopril, enalapril, lisinopril and others)
- Angiotensin-II receptor antagonists (Cozaar*, Diovan*, Avapro* and others)
- Heparin
- Aldosterone antagonists
OTHER CONSIDERATIONS BEFORE TAKING ORAL CONTRACEPTIVES
Tell your healthcare provider if you have or ever had:
- Breast nodules, fibrocystic disease of the breast, an abnormal breast X-ray or mammogram
- Diabetes
- Elevated cholesterol or triglycerides
- High blood pressure
- A blood test indicating a higher risk of having blood clots
- Migraine or other headaches or epilepsy
- Mental depression
- Gallbladder, heart or kidney disease
- History of scanty or irregular menstrual periods
Women with any of these conditions should be checked often by their healthcare provider if they choose to use oral contraceptives.
Also, be sure to inform your doctor or healthcare provider if you smoke, are on any medications, recently had a baby or miscarriage, or are breast feeding.
RISKS OF TAKING ORAL CONTRACEPTIVES
1. Risk of Developing Blood Clots
Blood clots and blockage of blood vessels are the most serious side effects of taking oral contraceptives and can be fatal. In particular, a clot in the legs (deep vein thrombosis) can cause pain and swelling, and a clot that travels to the lungs can cause sudden blocking of the vessel carrying blood to the lungs. Rarely, clots occur in the blood vessels of the eye and may cause blindness, double vision, or impaired vision.
If you take oral contraceptives and need elective surgery, need to stay in bed for a prolonged illness or have recently delivered a baby, you may be at risk of developing blood clots. You should consult your doctor about stopping oral contraceptives three to four weeks before surgery and not taking oral contraceptives for two weeks after surgery or during bed rest. You should also not take oral contraceptives soon after delivery of a baby or a mid-trimester pregnancy loss or termination. It is advisable to wait for at least four to six weeks after delivery if you are not breast feeding. If you are breast feeding, you should wait until you have weaned your child before using the pill. (See also the section on Breast Feeding in GENERAL PRECAUTIONS.)
2. Heart Attacks and Strokes
Oral contraceptives may increase the tendency to develop strokes (stoppage or rupture of blood vessels in the brain) and angina pectoris and heart attacks (blockage of blood vessels in the heart). Any of these conditions can cause death or serious disability.
Smoking greatly increases the possibility of suffering heart attacks and strokes. Furthermore, smoking and the use of oral contraceptives greatly increase the chances of developing and dying of heart disease.
3. Gallbladder Disease
Oral contraceptive users probably have a greater risk than nonusers of having gallbladder disease, although this risk may be related to pills containing high doses of estrogens.
4. Liver Tumors
In rare cases, oral contraceptives can cause benign but dangerous liver tumors. These benign liver tumors can rupture and cause fatal internal bleeding. In addition, a possible but not definite association has been found with the pill and liver cancers in two studies, in which a few women who developed these very rare cancers were found to have used oral contraceptives for long periods. However, liver cancers are extremely rare. The chance of developing liver cancer from using the pill is thus even rarer.
5. Cancer of the Reproductive Organs and Breasts
Various studies give conflicting reports on the relationship between breast cancer and oral contraceptive use. Oral contraceptive use may slightly increase your chance of having breast cancer diagnosed, particularly after using hormonal contraceptives at a younger age. After you stop using hormonal contraceptives, the chances of getting breast cancer begin to go back down. You should have regular breast examinations by a healthcare provider and examine your own breasts monthly. Tell your healthcare provider if you have a family history of breast cancer or if you have had breast nodules or an abnormal mammogram. Women who currently have or have had breast cancer should not use oral contraceptives because breast cancer is a hormone-sensitive tumor.
Some studies have found an increase in the incidence of cancer of the cervix in women who use oral contraceptives. However, this finding may be related to factors other than the use of oral contraceptives.
ESTIMATED RISK OF DEATH FROM A BIRTH CONTROL METHOD OR PREGNANCY
All methods of birth control and pregnancy are associated with a risk of developing certain diseases, which may lead to disability or death. An estimate of the number of deaths associated with different methods of birth control and pregnancy has been calculated and is shown in the following table.
ANNUAL NUMBER OF BIRTH-RELATED OR METHOD-RELATED DEATHS ASSOCIATED WITH CONTROL OF FERTILITY PER 100,000 NONSTERILE WOMEN, BY FERTILITY-CONTROL METHOD ACCORDING TO AGE Adapted from H.W. Ory, Family Planning Perspectives, 15:57-63, 1983. Method of Control and Outcome 15 to 19 years 20 to 24 years 25 to 29 years 30 to 34 years 35 to 39 years 40 to 44 years No fertility control methods Deaths are birth-related 7 7.4 9.1 14.8 25.7 28.2 Oral contraceptives non-smoker Deaths are method-related 0.3 0.5 0.9 1.9 13.8 31.6 Oral contraceptives smoker 2.2 3.4 6.6 13.5 51.1 117.2 IUD 0.8 0.8 1 1 1.4 1.4 Condom 1.1 1.6 0.7 0.2 0.3 0.4 Diaphragm/spermicide 1.9 1.2 1.2 1.3 2.2 2.8 Periodic abstinence 2.5 1.6 1.6 1.7 2.9 3.6
In the above table, the risk of death from any birth control method is less than the risk of childbirth, except for oral contraceptive users over the age of 35 who smoke and pill users over the age of 40 even if they do not smoke. It can be seen in the table that for women aged 15 to 39, the risk of death was highest with pregnancy (7 to 26 deaths per 100,000 women, depending on age). Among pill users who do not smoke, the risk of death was always lower than that associated with pregnancy for any age group, except for those women over the age of 40, when the risk increases to 32 deaths per 100,000 women, compared to 28 associated with pregnancy at that age. However, for pill users who smoke and are over the age of 35, the estimated number of deaths exceeds those for other methods of birth control. If a woman is over the age of 40 and smokes, her estimated risk of death is four times higher (117/100,000 women) than the estimated risk associated with pregnancy (28/100,000 women) in that age group.
The suggestion that women over 40 who do not smoke should not take oral contraceptives is based on information from older high-dose pills and on less-selective use of pills than is practiced today. An Advisory Committee of the FDA discussed this issue in 1989 and recommended that the benefits of oral contraceptive use by healthy, non-smoking women over 40 years of age may outweigh the possible risks. However, all women, especially older women, are cautioned to use the lowest-dose pill that is effective.
WARNING SIGNALS
If any of these adverse effects occur while you are taking oral contraceptives, call your doctor immediately:
- Sharp chest pain, coughing of blood, or sudden shortness of breath (indicating a possible clot in the lung)
- Pain in the calf (indicating a possible clot in the leg)
- Crushing chest pain or heaviness in the chest (indicating a possible heart attack)
- Sudden severe headache or vomiting, dizziness or fainting, disturbances of vision or speech, weakness, or numbness in an arm or leg (indicating a possible stroke)
- Sudden partial or complete loss of vision (indicating a possible clot in the eye)
- Breast lumps (indicating possible breast cancer or fibrocystic disease of the breast; ask your doctor or healthcare provider to show you how to examine your breasts)
- Severe pain or tenderness in the stomach area (indicating a possibly ruptured liver tumor)
- Difficulty in sleeping, weakness, lack of energy, fatigue, or change in mood (possibly indicating severe depression)
- Jaundice or a light yellowing of the skin or eyeballs, accompanied frequently by fever, fatigue, loss of appetite, dark-colored urine, or light-colored bowel movements (indicating possible liver problems)
SIDE EFFECTS OF ORAL CONTRACEPTIVES
1. Vaginal Bleeding
Irregular vaginal bleeding or spotting may occur while you are taking the pills. Irregular bleeding may vary from slight staining between menstrual periods to breakthrough bleeding, which is a flow much like a regular period. Irregular bleeding occurs most often during the first few months of oral contraceptive use, but may also occur after you have been taking the pill for some time. Such bleeding may be temporary and usually does not indicate any serious problems. It is important to continue taking your pills on schedule. If the bleeding occurs in more than one cycle or lasts for more than a few days, talk to your doctor or healthcare provider.
2. Contact Lenses
If you wear contact lenses and notice a change in vision or an inability to wear your lenses, contact your doctor or healthcare provider.
3. Fluid Retention
Oral contraceptives may cause edema (fluid retention) with swelling of the fingers or ankles and may raise your blood pressure. If you experience fluid retention, contact your doctor or healthcare provider.
4. Melasma
A spotty darkening of the skin is possible, particularly of the face.
5. Other Side Effects
Other side effects may include nausea, vomiting, change in appetite, headache, nervousness, depression, dizziness, loss of scalp hair, rash, and vaginal infections.
If any of these side effects bother you, call your doctor or healthcare provider.
GENERAL PRECAUTIONS
1. Missed Periods and Use of Oral Contraceptives Before or During Early Pregnancy
There may be times when you may not menstruate regularly after you have completed taking a cycle of pills. If you have taken your pills regularly and miss one menstrual period, continue taking your pills for the next cycle but be sure to inform your healthcare provider. If you have not taken the pills daily as instructed and missed a menstrual period, or if you missed two consecutive menstrual periods, you may be pregnant. Check with your healthcare provider immediately to determine whether you are pregnant. Stop taking oral contraceptives if pregnancy is confirmed. There is no conclusive evidence that oral contraceptive use is associated with an increase in birth defects when taken inadvertently during early pregnancy. Previously, a few studies had reported that oral contraceptives might be associated with birth defects, but these studies have not been confirmed. Nevertheless, oral contraceptives should not be used during pregnancy. You should check with your doctor about risks to your unborn child of any medication taken during pregnancy.
2. While Breast Feeding
If you are breast feeding, consult your doctor before starting oral contraceptives. Some of the drug will be passed on to the child in the milk. A few adverse effects on the child have been reported, including light yellowing of the skin (jaundice) and breast enlargement. In addition, oral contraceptives may decrease the amount and quality of your milk. If possible, do not use oral contraceptives while breast feeding. You should use another method of contraception since breast feeding provides only partial protection from becoming pregnant, and this partial protection decreases significantly as you breast feed for longer periods of time. You should consider starting oral contraceptives only after you have weaned your child completely.
3. Laboratory Tests
If you are scheduled for any laboratory tests, tell your doctor you are taking birth control pills. Certain blood tests may be affected by birth control pills.
4. Drug Interactions
Certain drugs may interact with birth control pills to make them less effective in preventing pregnancy or cause an increase in breakthrough bleeding. Such drugs include rifampin, drugs used for epilepsy such as barbiturates (for example, phenobarbital) and phenytoin (Dilantin is one brand of this drug), phenylbutazone (Butazolidin is one brand) and possibly certain antibiotics. Herbal products containing St. John’s Wort (hypericum perforatum) may reduce the effectiveness of oral contraceptives. This may also result in breakthrough bleeding. You may need to use an additional method of contraception during any cycle in which you take drugs that can make oral contraceptives less effective (See BOLDED TEXT AT BEGINNING).
5. Sexually Transmitted Diseases
This product (like all oral contraceptives) is intended to prevent pregnancy. It does not protect against transmission of HIV (AIDS) and other sexually transmitted diseases such as chlamydia, genital herpes, genital warts, gonorrhea, hepatitis B, and syphilis.
INSTRUCTIONS TO PATIENTS
HOW TO TAKE THE PILL
IMPORTANT POINTS TO REMEMBER
BEFORE YOU START TAKING YOUR PILLS:
1. BE SURE TO READ THESE DIRECTIONS:
- Before you start taking your pills.
- Anytime you are not sure what to do.
2. THE RIGHT WAY TO TAKE THE PILL IS TO TAKE ONE PILL EVERY DAY AT THE SAME TIME. GIANVI™ TABLETS CAN BE TAKEN WITHOUT REGARD TO MEALS.
If you miss pills you could get pregnant. This includes starting the pack late. The more pills you miss, the more likely you are to get pregnant. See “WHAT TO DO IF YOU MISS PILLS” below.
3. MANY WOMEN HAVE SPOTTING OR LIGHT BLEEDING, OR MAY FEEL SICK TO THEIR STOMACH DURING THE FIRST 1 TO 3 PACKS OF PILLS.
If you do have spotting or light bleeding or feel sick to your stomach, do not stop taking the pill. The problem will usually go away. If it does not go away, check with your healthcare provider.
4. MISSING PILLS CAN ALSO CAUSE SPOTTING OR LIGHT BLEEDING, even when you make up these missed pills.
On the days you take two pills, to make up for missed pills, you could also feel a little sick to your stomach.
5. IF YOU HAVE VOMITING (within 3 to 4 hours after you take your pill), you should follow the instructions for “WHAT TO DO IF YOU MISS PILLS”. IF YOU HAVE DIARRHEA or IF YOU TAKE CERTAIN MEDICINES, including some antibiotics and some herbal products such as St. John’s Wort, your pills may not work as well.
Use a back-up method (such as condoms or spermicides) until you check with your healthcare provider.
6. IF YOU HAVE TROUBLE REMEMBERING TO TAKE THE PILL, talk to your healthcare provider about how to make pill-taking easier or about using another method of birth control.
7. IF YOU HAVE ANY QUESTIONS OR ARE UNSURE ABOUT THE INFORMATION IN THIS LEAFLET, call your healthcare provider.
BEFORE YOU START TAKING YOUR PILLS
1. DECIDE WHAT TIME OF DAY YOU WANT TO TAKE YOUR PILL.
It is important to take Gianvi tablets at about the same time every day. Gianvi tablets can be taken without regard to meals.
2. LOOK AT YOUR PILL PACK: – IT HAS 28 PILLS
The Gianvi tablets-pill pack has 24 pink “active” pills (with hormones) to be taken for 24 days, followed by 4 white “reminder” pills (without hormones) to be taken for four days.
3. ALSO FIND:
1) Where on the pack to start taking pills,
2) In what order to take the pills (follow the arrows)
3) The week numbers are shown on the buler card picture below

4. BE SURE YOU HAVE READY AT ALL TIMES:
ANOTHER KIND OF BIRTH CONTROL (such as condoms or spermicides) to use as a back-up in case you miss pills.
AN EXTRA, FULL PILL PACK.
WHEN TO START THE FIRST PACK OF PILLS
You have a choice for which day to start taking your first pack of pills. Decide with your healthcare provider which is the best day for you. Pick a time of day, which will be easy to remember.
DAY 1 START:
1. Take the first pink “active” pill of the first pack during the first 24 hours of your period.
2. You will not need to use a back-up method of birth control, since you are starting the pill at the beginning of your period.
SUNDAY START:
1. Take the first pink “active” pill of the first pack on the Sunday after your period starts, even if you are still bleeding. If your period begins on Sunday, start the pack that same day.
2. Use another method of birth control (such as condoms or spermicides) as a back-up method if you have sex anytime from the Sunday you start your first pack until the next Sunday (7 days).
WHEN YOU SWITCH FROM A DIFFERENT BIRTH CONTROL PILL
When switching from another birth control pill, Gianvi tablets should be started on the same day that a new pack of the previous birth control pill would have been started.
WHAT TO DO DURING THE MONTH
1. TAKE ONE PILL AT THE SAME TIME EVERY DAY UNTIL THE PACK IS EMPTY
Do not skip pills even if you are spotting or bleeding between monthly periods or feel sick to your stomach (nausea).
Do not skip pills even if you do not have sex very often.
2. WHEN YOU FINISH A PACK OF PILLS:
Start the next pack on the day after your last white “reminder” pill. Do not wait any days between packs.
WHAT TO DO IF YOU MISS PILLS
If you MISS 1 pink “active” pill:
1. Take it as soon as you remember. Take the next pill at your regular time. This means you may take two pills in one day.
2. You do not need to use a back-up birth control method if you have sex.
If you MISS 2 pink “active” pills in a row in WEEK 1 OR WEEK 2 of your pack:
1. Take two pills on the day you remember and two pills the next day.
2. Then take one pill a day until you finish the pack.
3. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicides) as a back-up for those 7 days.
If you MISS 2 pink “active” pills in a row in WEEK 3 or WEEK 4 of your pack:
1. If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
If you are a Sunday Starter:
Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
2. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicide) as a back-up for those 7 days.
3. You may not have your period this month but this is expected. However, if you miss your period two months in a row, call your doctor or clinic because you might be pregnant.
If you MISS 3 OR MORE pink “active” pills in a row during ANY WEEK:
1. If you are a Day 1 Starter:
THROW OUT the rest of the pill pack and start a new pack that same day.
If you are a Sunday Starter:
Keep taking 1 pill every day until Sunday. On Sunday, THROW OUT the rest of the pack and start a new pack of pills that same day.
2. You COULD BECOME PREGNANT if you have sex in the 7 days after you restart your pills. You MUST use another birth control method (such as condoms or spermicides) as a back-up for those 7 days.
3. You may not have your period this month but this is expected. However, if you miss your period two months in a row, call your doctor or clinic because you might be pregnant.
If you MISS ANY of the 4 white “reminder” pills in WEEK 4:
- THROW AWAY the pills you missed.
- Keep taking one pill each day until the pack is empty.
- You do not need a back-up method.
FINALLY, IF YOU ARE STILL NOT SURE WHAT TO DO ABOUT THE PILLS YOU HAVE MISSED:
Use a BACK-UP METHOD (such as condoms or spermicides) anytime you have sex.
KEEP TAKING ONE ACTIVE PINK PILL EACH DAY until you contact your healthcare provider.
PREGNANCY AFTER STOPPING THE PILL
There may be some delay in becoming pregnant after you stop using oral contraceptives, especially if you had irregular menstrual cycles before you used oral contraceptives. It may be advisable to postpone conception until you begin menstruating regularly once you have stopped taking the pill and desire pregnancy.
There does not appear to be any increase in birth defects in newborn babies when pregnancy occurs soon after stopping the pill.
OVERDOSAGE
Serious ill effects have not been reported following ingestion of large doses of other oral contraceptives by young children. Overdosage of drospirenone and ethinyl estradiol tablets may cause nausea and withdrawal bleeding in females and may increase blood levels of potassium or decrease blood levels of sodium, which could be dangerous. In case of overdosage, contact your healthcare provider.
OTHER INFORMATION
Your healthcare provider will take a medical and family history before prescribing oral contraceptives and will examine you. The physical examination may be delayed to another time if you request it and the healthcare provider believes that it is appropriate to postpone it. You should be re-examined at least once a year. Be sure to inform your healthcare provider if there is a family history of any of the conditions uled previously in this leaflet. Be sure to keep all appointments with your healthcare provider, because this is a time to determine if there are early signs of side effects of oral contraceptive use.
Do not use the drug for any condition other than the one for which it was prescribed. This drug has been prescribed specifically for you; do not give it to others who may want birth control pills.
HEALTH BENEFITS FROM ORAL CONTRACEPTIVES
In addition to preventing pregnancy, use of oral contraceptives may provide certain benefits. They are:
- Menstrual cycles may become more regular.
- Blood flow during menstruation may be lighter and less iron may be lost. Therefore, anemia due to iron deficiency is less likely to occur.
- Pain or other symptoms during menstruation may be encountered less frequently.
- Ovarian cysts may occur less frequently.
- Ectopic (tubal) pregnancy may occur less frequently.
- Noncancerous cysts or lumps in the breast may occur less frequently.
- Acute pelvic inflammatory disease may occur less frequently.
- Oral contraceptive use may provide some protection against developing two forms of cancer: cancer of the ovaries and cancer of the lining of the uterus.
If you want more information about birth control pills, ask your doctor or pharmacist. They have a more technical leaflet called the Prescribing Information which you may wish to read.
Call your doctor for medical advice about side effects. You may report side effects to FDA at 1-800-FDA-1088.
*Other trademarks are the properties of their respective owners.
KEEP THIS AND ALL MEDICATIONS OUT OF THE REACH OF CHILDREN.
Manufactured By:BARR LABORATORIES, INC.Pomona, NY 10970
Manufactured For: TEVA PHARMACEUTICALS USA Sellersville, PA 18960
Rev. D 6/2010
Relabeling of "Additional Barcode Label" by: Physicians Total Care, Inc.Tulsa, OKÂ Â Â Â Â 74146
Principal Display Panel

Gianvi (drospirenone and ethinyl estradiol tablets) 3 mg/0.02 mg, 28 Day Regimen Pouch Text
NDC 54868-6162-0
Gianvi™
(drospirenone and
ethinyl estradiol tablets)
3 mg/0.02 mg
Contents: One dispenser of 28 tablets, 24 pink tablets and 4 white inert tablets.
Each pink tablet (24) contains 3 mg drospirenone and 0.02 mg ethinyl estradiol.
Each white tablet (4) contains inert ingredients.
28 DAY REGIMEN
Rx only
THIS PRODUCT (LIKE ALL ORAL CONTRACEPTIVES) IS INTENDED TO
PREVENT PREGNANCY. IT DOES NOT PROTECT AGAINST HIV INFECTION
(AIDS) AND OTHER SEXUALLY TRANSMITTED DISEASES.
TEVA
SHAPING WOMEN'S HEALTH®
DISCLAIMER:
"This tool does not provide medical advice, and is for informational and educational purposes only, and is not a substitute for professional medical advice, treatment or diagnosis. Call your doctor to receive medical advice. If you think you may have a medical emergency, please dial 911."
"Do not rely on openFDA to make decisions regarding medical care. While we make every effort to ensure that data is accurate, you should assume all results are unvalidated. We may limit or otherwise restrict your access to the API in line with our Terms of Service."
"This product uses publicly available data from the U.S. National Library of Medicine (NLM), National Institutes of Health, Department of Health and Human Services; NLM is not responsible for the product and does not endorse or recommend this or any other product."
PillSync may earn a commission via links on our site

