Fanapt (iloperidone 2 mg) Dailymed
Generic: iloperidone is used for the treatment of Schizophrenia
IMPRINT: 12
SHAPE: round
COLOR: white
All Imprints
iloperidone 12 mg - 12 round white
iloperidone 2 mg - 2 round white
iloperidone 6 mg - 6 round white
iloperidone 8 mg - 8 round white
Boxed Warning
Warning: Increased Mortality In Elderly Patients With Dementia-related Psychosis
Go PRO for all pill images
Recent Major Changes Section
Indications and Usage (1 )                                                                4/2024
Dose and Administration (2.1 ,2.2 ,2.3 ,2.4 )                                   4/2024
Warnings and Precautions (5.6 ,5.7 ,5.11 ,5.15 ,5.16 )                     4/2024
Warnings and Precautions, Suicide (5.14)                       Removed 4/2024
Warning: Increased Mortality In Elderly Patients With Dementia-related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death.
FANAPT is not approved for the treatment of patients with dementia-related psychosis[see Warnings and Precautions (5.1)] .
WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS WITH DEMENTIA-RELATED PSYCHOSIS
See full prescribing information for complete boxed warning.
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. FANAPT is not approved for use in patients with dementia-related psychosis. (5.1 )
1 Indications And Usage
FANAPT¬ģ¬†is indicated for:
- Treatment of schizophrenia in adults [see Clinical Studies (14.1)].
- Acute treatment of manic or mixed episodes associated with bipolar I disorder in adults [see Clinical Studies (14.2)].
FANAPT is an atypical antipsychotic indicated for:
- Treatment of schizophrenia in adults. (
1 ,14.1 )- Acute treatment of manic or mixed episodes associated with bipolar I disorder in adults. (
1 ,14.2 )
2 Dosage And Administration
- Administer FANAPT orally twice daily without regard to meals. (
2.1 )- Titrate the dosage of FANAPT to avoid orthostatic hypotension. See Full Prescribing Information for titration schedule. (
2.1 )- Recommended Dosage:
Indication Starting Dosage Recommended Dosage Schizophrenia( 2.1 )1 mg twice daily 6 mg to 12 mg twice daily Bipolar Mania( 2.1 )1 mg twice daily 12 mg twice daily
- CYP2D6 Poor Metabolizers: See Full Prescribing Information for titration schedule and recommended dosage. (
2.2 )2.1 Recommended Dosage
Titrate FANAPT to avoid orthostatic hypotension [see Warnings and Precautions (5.7)].
Administer FANAPT orally with or without food.
Table 1 includes dosage recommendations for FANAPT for the treatment of schizophrenia and the acute treatment of manic or mixed episodes associated with bipolar I disorder in adults.
Table 1: Dosage Recommendations for FANAPT in Adults for the Treatment of Schizophrenia or Acute Treatment of Manic or Mixed Episodes Associated with Bipolar I Disorder
Indication and Population Titration schedule Recommended Dosage Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Schizophrenia 1mgtwicedaily 2 mgtwicedaily 4 mgtwicedaily 6 mgtwicedaily 8 mgtwicedaily 10 mgtwicedaily 12 mgtwicedaily 6 mg to 12 mgtwice daily Bipolar I DisorderManic or Mixed Episodes 1 mgtwicedaily 3 mgtwicedaily 6 mgtwicedaily 9 mgtwicedaily 12 mgtwicedaily Titration complete 12 mgtwice daily 2.2Dosage Recommendations for Use in Patients Who Are Known CYP2D6 Poor Metabolizers
Reduce the dose of FANAPT by one-half for CYP2D6 poor metabolizers [see Clinical Pharmacology (12.3, 12.5)]. Table 2 includes dosage recommendations for FANAPT in adults who are CYP2D6 poor metabolizers.
Table 2: Dosage Recommendations for FANAPT in Adults with Schizophrenia or Bipolar I Disorder Who are CYP2D6 Poor Metabolizers
Indication and Population Titration schedule Recommended Dosage Day 1 Day 2 Day 3 Day 4 Day 5 Day 6 Day 7 Schizophrenia 1mgtwicedaily 2 mgtwicedaily 4 mgtwicedaily 6 mgtwicedaily Titration complete 3 mg to 6 mgtwice daily Bipolar I DisorderManic or Mixed Episodes 1 mgtwicedaily 3 mgtwicedaily 6 mgtwicedaily Titration complete 6 mgtwice daily 2.3Dosage Recommendations in Patients with Hepatic Impairment
No dose adjustment for FANAPT is needed in patients with mild hepatic impairment. Patients with moderate hepatic impairment may require dose reduction, if clinically indicated. FANAPT is not recommended for patients with severe hepatic impairment [see Use in Specific Populations (8.6)].
2.4Dosage Modifications for Concomitant Use with Strong CYP2D6 Inhibitors and Strong CYP3A4 Inhibitors
Coadministration with Strong CYP2D6 Inhibitors
Reduce the dose of FANAPT one-half when administered concomitantly with strong CYP2D6 inhibitors such as fluoxetine or paroxetine. When the CYP2D6 inhibitor is withdrawn from the combination therapy, increase the dose of FANAPT to where it was before [see Drug Interactions (7.1)].
Coadministration with Strong CYP3A4 Inhibitors
Reduce the dose of FANAPT by one-half when administered concomitantly with strong CYP3A4 inhibitors such as ketoconazole or clarithromycin. When the CYP3A4 inhibitor is withdrawn from the combination therapy, increase the dose of FANAPT to where it was before [see Drug Interactions (7.1)].
Coadministration with Strong CYP2D6 and Strong CYP3A4 Inhibitors
Reduce the dose of FANAPT by about one-half if administered concomitantly with inhibitors of CYP2D6 and CYP3A4. When both CYP2D6 and CYP3A4 inhibitors are withdrawn from the combination therapy, increase the dose of FANAPT to where it was before [see Drug Interactions (7.1)].
2.5Reinitiation of Treatment in Patients Previously Discontinued
Although there are no data to specifically address reinitiation of treatment, it is recommended that the initiation titration schedule be followed whenever patients have had an interval off FANAPT of more than 3 days.
3 Dosage Forms And Strengths
FANAPT tablets are available in the following strengths: 1 mg, 2 mg, 4 mg, 6 mg, 8 mg, 10 mg, and 12 mg.¬†The tablets are white, round, flat, beveled-edged and identified with a logo ‚Äú‚ÄĚ debossed on one side and tablet strength ‚Äú1‚ÄĚ, ‚Äú2‚ÄĚ, ‚Äú4‚ÄĚ, ‚Äú6‚ÄĚ, ‚Äú8‚ÄĚ, ‚Äú10‚ÄĚ, or ‚Äú12‚ÄĚ debossed on the other side.
1 mg, 2 mg, 4 mg, 6 mg, 8 mg, 10 mg and 12 mg tablets. (3 )
4 Contraindications
FANAPT is contraindicated in individuals with a known hypersensitivity reaction to the product. Anaphylaxis, angioedema, and other hypersensitivity reactions have been reported [see Adverse Reactions (6.2)].
Known hypersensitivity to FANAPT or to any components in the formulation. (4 ,6.2 ) 
5 Warnings And Precautions
- Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- Related Psychosis: Increased incidence of cerebrovascular adverse reactions (e.g., stroke, transient ischemic attack). (
5.2 )- QT prolongation: Prolongs QT interval and may be associated with arrhythmia and sudden death. Avoid use of FANAPT in combination with other drugs that are known to prolong QTc; use caution and consider dose modification when prescribing FANAPT with other drugs that inhibit FANAPT metabolism. Monitor serum potassium and magnesium in patients at risk for electrolyte disturbances. (
1 ,5.3 ,7.1 ,7.2 ,12.3 )- Neuroleptic Malignant Syndrome (NMS): Manage with immediate discontinuation of drug and close monitoring. (
5.4 )- Tardive dyskinesia: Discontinue if clinically appropriate. (
5.5 )- Metabolic Changes: Monitor for hyperglycemia/diabetes mellitus, dyslipidemia and weight gain. (
5.6 )- Orthostatic hypotension and Syncope: Monitor heart rate and blood pressure and warn patients with known cardiovascular or cerebrovascular disease, and risk of dehydration or syncope. (
5.7 )- Seizures: Use cautiously in patients with a history of seizures or with conditions that lower seizure threshold. (
5.9 )- Leukopenia, Neutropenia, and Agranulocytosis have been reported with antipsychotics. Perform complete blood counts (CBC) in patients with pre-existing low white blood cell count (WBC) or a history of leukopenia/neutropenia. Consider discontinuing FANAPT if clinically significant decline in WBC occurs in the absence of other causative factors. (
5.10 )- Priapism: Cases have been reported in association with FANAPT treatment. Severe priapism may require surgical intervention. (
5.14 )- Potential for cognitive and motor impairment: Use caution when operating machinery. (
5.15 )- Intraoperative Floppy Iris Syndrome (IFIS): IFIS during cataract surgery may require modifications to the surgical technique. (
5.16 )5.1 Increased Mortality in Elderly Patients with Dementia-Related Psychosis
Elderly patients with dementia-related psychosis treated with antipsychotic drugs are at an increased risk of death. Analyses of 17 dementia-related psychosis placebo-controlled trials (modal duration of 10 weeks) largely in patients taking atypical antipsychotic drugs, revealed a risk of death in the drug-treated patients of between 1.6 to 1.7 times that in placebo-treated patients. Over the course of a typical 10-week controlled trial, the rate of death in drug-treated patients was about 4.5%, compared to a rate of about 2.6% in placebo-treated patients.
Although the causes of death were varied, most of the deaths appeared to be either cardiovascular (e.g., heart failure, sudden death) or infectious (e.g., pneumonia) in nature. FANAPT is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning, Warnings and Precautions (5.2)].
5.2 Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis
In placebo-controlled trials in elderly subjects with dementia, patients randomized to risperidone, aripiprazole, and olanzapine had a higher incidence of stroke and transient ischemic attack, including fatal stroke. FANAPT is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning, Warnings and Precautions (5.1)].
5.3 QT Prolongation
In an open-label QTc study in patients with schizophrenia or schizoaffective disorder (n=160), FANAPT was associated with QTc prolongation of 9 msec at an iloperidone dose of 12 mg twice daily. The effect of FANAPT on the QT interval was augmented by the presence of CYP450 2D6 or 3A4 metabolic inhibition (paroxetine 20 mg once daily and ketoconazole 200 mg twice daily, respectively). Under conditions of metabolic inhibition for both 2D6 and 3A4, FANAPT 12 mg twice daily was associated with a mean QTcF increase from baseline of about 19 msec.
No cases of torsade de pointes or other severe cardiac arrhythmias were observed during the pre-marketing clinical program.
The use of FANAPT should be avoided in combination with other drugs that are known to prolong QTc including Class 1A (e.g., quinidine, procainamide) or Class III (e.g., amiodarone, sotalol) antiarrhythmic medications, antipsychotic medications (e.g., chlorpromazine, thioridazine), antibiotics (e.g., gatifloxacin, moxifloxacin), or any other class of medications known to prolong the QTc interval (e.g., pentamidine, levomethadyl acetate, methadone). FANAPT should also be avoided in patients with a known genetic susceptibility to congenital long QT syndrome and in patients with a history of cardiac arrhythmias.
Certain circumstances may increase the risk of torsade de pointes and/or sudden death in association with the use of drugs that prolong the QTc interval, including (1) bradycardia; (2) hypokalemia or hypomagnesemia; (3) concomitant use of other drugs that prolong the QTc interval; and (4) presence of congenital prolongation of the QT interval; (5) recent acute myocardial infarction; and/or (6) uncompensated heart failure.
Caution is warranted when prescribing FANAPT with drugs that inhibit FANAPT metabolism [see Drug Interactions (7.1)], and in patients with reduced activity of CYP2D6 [see Clinical Pharmacology (12.3, 12.5)].
It is recommended that patients being considered for FANAPT treatment who are at risk for significant electrolyte disturbances have baseline serum potassium and magnesium measurements with periodic monitoring. Hypokalemia (and/or hypomagnesemia) may increase the risk of QT prolongation and arrhythmia. FANAPT should be avoided in patients with histories of significant cardiovascular illness, e.g., QT prolongation, recent acute myocardial infarction, uncompensated heart failure, or cardiac arrhythmia. FANAPT should be discontinued in patients who are found to have persistent QTc measurements >500 msec.
If patients taking FANAPT experience symptoms that could indicate the occurrence of cardiac arrhythmias, e.g., dizziness, palpitations, or syncope, the prescriber should initiate further evaluation, including cardiac monitoring.
5.4 Neuroleptic Malignant Syndrome (NMS)
Neuroleptic Malignant Syndrome (NMS), a potentially fatal symptom complex, has been reported in association with administration of antipsychotic drugs, including FANAPT. Clinical manifestations include hyperpyrexia, muscle rigidity, altered mental status (including catatonic signs), and evidence of autonomic instability (irregular pulse or blood pressure, tachycardia, diaphoresis, and cardiac dysrhythmia). Additional signs may include elevated creatine phosphokinase, myoglobinuria (rhabdomyolysis), and acute renal failure.
If NMS is suspected, immediately discontinue FANAPT and provide intensive symptomatic treatment and monitoring.
5.5 Tardive Dyskinesia
Tardive dyskinesia, a syndrome consisting of potentially irreversible, involuntary, dyskinetic movements, may develop in patients treated with antipsychotic drugs. The risk appears to be highest among the elderly, especially elderly women, but it is impossible to predict, which patients will develop the syndrome. Whether antipsychotic drug products differ in their potential to cause tardive dyskinesia is unknown.
The risk of developing tardive dyskinesia and the likelihood that it will become irreversible increase with the duration of treatment and cumulative dose. The syndrome can develop after relatively brief treatment periods at low doses. It may also occur after discontinuation of treatment.
Tardive dyskinesia may remit, partially or completely, if antipsychotic treatment is discontinued. Antipsychotic treatment itself may suppress (or partially suppress) the signs and symptoms of the syndrome, possibly masking the underlying process. The effect that symptomatic suppression has upon the long-term course of the syndrome is unknown.
Given these considerations, FANAPT should be prescribed in a manner that is most likely to reduce the risk of tardive dyskinesia. Chronic antipsychotic treatment should generally be reserved for patients: 1) who suffer from a chronic illness that is known to respond to antipsychotic drugs, and (2) for whom alternative, equally effective, but potentially less harmful treatments are not available or appropriate. In patients who do require chronic treatment, use the lowest dose and the shortest duration of treatment producing a satisfactory clinical response. Periodically reassess the need for continued treatment.
If signs and symptoms of tardive dyskinesia appear in a patient on FANAPT, drug discontinuation should be considered. However, some patients may require treatment with FANAPT despite the presence of the syndrome.
5.6 Metabolic Changes
Atypical antipsychotic drugs have been associated with metabolic changes that may increase cardiovascular/cerebrovascular risk. These metabolic changes include hyperglycemia, dyslipidemia, and body weight gain. While all atypical antipsychotic drugs have been shown to produce some metabolic changes, each drug in the class has its own specific risk profile.
Hyperglycemia and Diabetes Mellitus
Hyperglycemia, in some cases extreme and associated with ketoacidosis or hyperosmolar coma or death, has been reported in patients treated with atypical antipsychotics including FANAPT. Assess fasting plasma glucose before or soon after initiation of antipsychotic medication and monitor periodically during long-term treatment.
Schizophrenia
In a 4-week fixed-dose placebo-controlled study of adults with schizophrenia, the mean change from baseline in serum glucose was 6.6 mg/dL and -0.5 mg/dL for FANAPT and placebo treated patients, respectively. The proportion of patients with shifts in fasting glucose from normal (<100 mg/dL) to high (‚Č•126 mg/dL) were 10.7% and 2.5% for FANAPT and placebo treated patients, respectively.
In pooled analyses from clinical studies, for adults with schizophrenia remaining on treatment with FANAPT 10-16 mg/day glucose increased, on average, from baseline by 1.8 mg/dL at 3-6 months (N=773) and by 5.4 mg/dL at 6-12 months (N=723) and at >12 months (N=425) of treatment. In a smaller group of patients remaining on treatment with FANAPT 20-24 mg/day, glucose decreased by 3.6 mg/dL at 3-6 months (N=34); by 9 mg/dL at 6-12 months (N=31), and by 18 mg/dL at > 12 months (N=20) of treatment.
Bipolar Mania
In a 4-week fixed dose study of adults with bipolar mania, mean changes from baseline in serum glucose and the proportion of patients with shifts in fasting glucose from Normal (<100 mg/dL) to High (‚Č•126 mg/dL) for patients receiving FANAPT were similar to those for patients receiving placebo.
Dyslipidemia
Undesirable alterations in lipids have been observed in patients treated with atypical antipsychotics. Before or soon after initiation of antipsychotic medications, obtain a fasting lipid profile at baseline and monitor periodically during treatment.
Schizophrenia
In a 4-week fixed dose study of adults with schizophrenia, the mean change from baseline in fasted total cholesterol was 8.2 mg/dL and -2.2 mg/dL for FANAPT and placebo treated patients, respectively. The effects on LDL were similar to those on total cholesterol (changes of 9 mg/dL and -1.4 mg/dL for FANAPT and placebo treated patients, respectively). Mean changes from baseline in fasted triglycerides were -0.8 mg/dL and 16.5 mg/dL for FANAPT and placebo treated patients, respectively.
The proportion of patients with shifts from normal to high fasted total cholesterol, LDL, and triglycerides were similar for FANAPT and placebo-treated patients. The proportion of patients with shifts in fasted HDL from normal (‚Č•40 mg/dL) to low (<40 mg/dL) was greater for placebo patients (23.8%) compared to patients treated with FANAPT (12.1%).
In pooled analysis from clinical studies, for adults with schizophrenia remaining on treatment with FANAPT, on average, both cholesterol and triglycerides decreased from baseline for adults with schizophrenia remaining on treatment at 3-6 months, 6-12 months, and >12-month time points in both 10-16 mg/day and 20-24 mg/day dose groups.
Bipolar Mania
In a 4-week fixed dose study of adults with bipolar mania, the mean changes from baseline for fasted total cholesterol, LDL, HDL, and triglycerides for FANAPT were similar to those for placebo-treated patients. The proportion of patients with shifts in fasted total cholesterol from normal (<200 mg/dL) to high (‚Č•240 mg/dL) was greater for FANAPT treated patients (10.7%) than placebo-treated patients (7.2%). Shifts from normal to high LDL and triglycerides and from normal to low HDL occurred at rates for FANAPT similar to those for placebo treated patients.
Weight Gain
Weight gain has been observed with atypical antipsychotic use. Monitor weight at baseline and frequently thereafter.
Schizophrenia
Across all short- and long-term studies of adults with schizophrenia, the overall mean change from baseline at endpoint was 2.1 kg.
In 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies in adults with schizophrenia the mean change in weight (kg) was -0.1, 2, and 2.7 for placebo, FANAPT 10-16 mg/day, and FANAPT 20-24 mg/day groups, respectively. The proportion of patients with weight gain >7% increase from baseline was 4%, 12%, and 18% for placebo, FANAPT 10-16 mg/day, and FANAPT 20-24 mg/day groups, respectively.
Bipolar Mania
In a 4-week fixed dose study of adults with bipolar mania the mean change in weight (kg) was 1.6 and 4.6 kg for placebo and FANAPT 24 mg/day groups, respectively. The proportion of patients with weight gain ‚Č•7% increase from baseline was 14% and 35%, for placebo and FANAPT 24 mg/day groups, respectively.
5.7 Orthostatic Hypotension and Syncope
FANAPT can induce orthostatic hypotension associated with dizziness, tachycardia, and syncope. This reflects its alpha1-adrenergic antagonist properties. In double-blind placebo-controlled short-term studies in patients with schizophrenia, where the dose was increased slowly, as recommended above, syncope was reported in 0.4% (5/1,344) of patients treated with FANAPT, compared with 0.2% (1/587) on placebo. Orthostatic hypotension was reported in 5% of patients given 20 mg to 24 mg/day, 3% of patients given 10 mg to 16 mg/day, and 1% of patients given placebo.
In a double-blind placebo-controlled short-term study in patients with bipolar mania, syncope was reported in 0.5% (1/206) of patients treated with FANAPT, compared with 0% (0/208) on placebo. In this study, orthostatic hypotension was reported in 4% (9/206) of patients treated with FANAPT and 2% (5/208) of patients given placebo.
More rapid titration would be expected to increase the rate of orthostatic hypotension and syncope.
Orthostatic vital signs should be monitored in patients who are vulnerable to hypotension (e.g., elderly patients, patients with dehydration, hypovolemia, and concomitant treatment with antihypertensive medications), patients with known cardiovascular disease (history of myocardial infarction, ischemic heart disease, heart failure, or conduction abnormalities), and patients with cerebrovascular disease.
5.8 Falls
Antipsychotics, including FANAPT, may cause somnolence, postural hypotension, motor and sensory instability, which may lead to falls and, consequently, fractures or other injuries. For patients with diseases, conditions, or medications that could exacerbate these effects, complete fall risk assessments when initiating antipsychotic treatment and recurrently for patients on long-term antipsychotic therapy.
5.9Seizures
Like other antipsychotic drugs, FANAPT may cause seizures. The risk is greatest in patients with a history of seizures or with conditions that lower the seizure threshold. Conditions that lower the seizure threshold may be more prevalent in older patients.
5.10Leukopenia, Neutropenia and Agranulocytosis
In clinical trial and postmarketing experience, leukopenia and neutropenia have been reported temporally related to antipsychotic agents. Agranulocytosis (including fatal cases) has also been reported.
Possible risk factors for leukopenia/neutropenia include preexisting low white blood cell count (WBC) and history of drug induced leukopenia/neutropenia. Patients with a pre-existing low WBC or a history of drug induced leukopenia/neutropenia should have their complete blood count (CBC) monitored frequently during the first few months of therapy and should discontinue FANAPT at the first sign of a decline in WBC in the absence of other causative factors.
Monitor patients with clinically significant neutropenia for fever or other symptoms or signs of infection and treat promptly if such symptoms or signs occur. Discontinue FANAPT in patients with absolute neutrophil count <1000/mm3 and follow their WBC until recovery.
5.11Hyperprolactinemia
As with other drugs that antagonize dopamine D2 receptors, FANAPT elevates prolactin levels.
Hyperprolactinemia may suppress hypothalamic GnRH, resulting in reduced pituitary gonadotropin secretion. This, in turn, may inhibit reproductive function by impairing gonadal steroidogenesis in both female and male patients. Galactorrhea, amenorrhea, gynecomastia, and impotence have been reported with prolactin-elevating compounds. Long-standing hyperprolactinemia when associated with hypogonadism may lead to decreased bone density in both female and male patients.
Tissue culture experiments indicate that approximately one-third of human breast cancers are prolactin-dependent in vitro, a factor of potential importance if the prescription of these drugs is contemplated in a patient with previously detected breast cancer. Mammary gland proliferative changes and increases in serum prolactin were seen in mice and rats treated with FANAPT [see Nonclinical Toxicology (13)]. Neither clinical studies nor epidemiologic studies conducted to date have shown an association between chronic administration of this class of drugs and tumorigenesis in humans; the available evidence is considered too limited to be conclusive at this time.
In a short-term placebo-controlled trial (4-weeks) in patients with schizophrenia, the mean change from baseline to endpoint in plasma prolactin levels for the FANAPT 24 mg/day-treated group was an increase of 2.6 ng/mL compared to a decrease of 6.3 ng/mL in the placebo-group. In placebo-controlled trials in patients with schizophrenia, elevated plasma prolactin levels (‚Č•1.15xULN) were observed in 26% of adults treated with FANAPT compared to 12% in the placebo group. In the short-term trials, FANAPT was associated with modest levels of prolactin elevation compared to greater prolactin elevations observed with some other antipsychotic agents. In pooled analysis from clinical studies including longer term trials, in 3210 adults treated with iloperidone, gynecomastia was reported in 2 male subjects (0.1%) compared to 0% in placebo-treated patients, and galactorrhea was reported in 8 female subjects (0.2%) compared to 3 female subjects (0.5%) in placebo-treated patients.
In a short-term, placebo-controlled trial (4-weeks) in patients with bipolar mania, the mean change from baseline to endpoint in plasma prolactin levels for the FANAPT group was an increase of 15.66 ng/mL compared to a decrease of 0.58 ng/mL for the placebo group. In this trial, elevated plasma prolactin levels (‚Č•1.15xULN) were observed in 35% of adults treated with FANAPT compared to 1% of the placebo group.
5.12Body Temperature Regulation
Atypical antipsychotics may disrupt the body’s ability to reduce core body temperature. Strenuous exercise, exposure to extreme heat, dehydration, and anticholinergic medications may contribute to an elevation in core body temperature; use FANAPT with caution in patients who may experience these conditions.
5.13 Dysphagia
Esophageal dysmotility and aspiration have been associated with antipsychotic drug use. Aspiration pneumonia is a common cause of morbidity and mortality in elderly patients. Antipsychotic drugs, including FANAPT, should be used cautiously in patients at risk for aspiration.
5.14Priapism
Four cases of priapism were reported in the pre-marketing FANAPT program (3 in the clinical studies for schizophrenia and 1 in the clinical study for manic and mixed episodes associated with bipolar I disorder). Drugs with alpha-adrenergic blocking effects have been reported to induce priapism. FANAPT shares this pharmacologic activity. Severe priapism may require surgical intervention.
5.15Potential for Cognitive and Motor Impairment
FANAPT, like other antipsychotics, may cause somnolence and has the potential to impair judgment, thinking or motor skills. In short-term, placebo-controlled trials of schizophrenia, somnolence (including sedation) was reported in 12% (104/874) of adult patients treated with FANAPT at doses of 10 mg/day or greater versus 5.3% (31/587) treated with placebo. In a short-term, placebo-controlled trial of bipolar mania, somnolence (including sedation) was reported in 8% (16/206) of adult patients treated with FANAPT versus 3% (6/208) treated with placebo.
Patients should be cautioned about operating hazardous machinery, including motor vehicles, until they are reasonably certain that therapy with FANAPT does not affect them adversely.
5.16Intraoperative Floppy Iris Syndrome (IFIS)
IFIS has been observed during cataract surgery in some patients on or previously treated with alpha-1 adrenergic blockers. This variant of small pupil syndrome is characterized by the combination of a flaccid iris that billows in response to intraoperative irrigation currents, progressive intraoperative miosis despite preoperative dilation with standard mydriatic drugs, and potential prolapse of the iris toward the phacoemulsification incisions. The patient’s surgeon should be prepared for possible modifications to their surgical technique, such as the utilization of iris hooks, iris dilator rings, or viscoelastic substances. There does not appear to be a benefit of stopping alpha1 blocker therapy prior to cataract surgery. The initiation of therapy with FANAPT in patients for whom cataract or glaucoma surgery is scheduled is not recommended.
6 Adverse Reactions
The following adverse reactions are discussed in more detail in other sections of the labeling:
- Increased Mortality in Elderly Patients with Dementia-Related Psychosis [see Warnings and Precautions (5.1)]
- Cerebrovascular Adverse Reactions, Including Stroke, in Elderly Patients with Dementia-Related Psychosis [see Warnings and Precautions (5.2)]
- QT Prolongation [see Warnings and Precautions (5.3)]
- Neuroleptic Malignant Syndrome (NMS) [see Warnings and Precautions (5.4)]
- Tardive Dyskinesia [see Warnings and Precautions (5.5)]
- Metabolic Changes [see Warnings and Precautions (5.6)]
- Orthostatic Hypotension and Syncope [see Warnings and Precautions (5.7)]
- Falls [see Warnings and Precautions (5.8)]
- Seizures [see Warnings and Precautions (5.9)]
- Leukopenia, Neutropenia and Agranulocytosis [see Warnings and Precautions (5.10)]
- Hyperprolactinemia [see Warnings and Precautions (5.11)]
- Body Temperature Regulation [see Warnings and Precautions (5.12)]
- Dysphagia [see Warnings and Precautions (5.13)]
- Priapism [see Warnings and Precautions (5.14)]
- Potential for Cognitive and Motor Impairment [see Warnings and Precautions (5.15)]
- Intraoperative Floppy Iris Syndrome [see Warnings and Precautions (5.16)]
Commonly observed adverse reactions¬†(incidence ‚Č•5% and 2-fold greater than placebo) were (6.1 ):
- Schizophrenia: dizziness, dry mouth, fatigue, nasal congestion, orthostatic hypotension, somnolence, tachycardia, and weight increased.
- Bipolar mania: tachycardia, dizziness, dry mouth, hepatic enzymes increased, nasal congestion, weight increased, hypotension, and somnolence.
To report SUSPECTED ADVERSE REACTIONS, contact Vanda Pharmaceuticals Inc. at 1-844-GO-VANDA (1-844-468-2632) or FDA at 1-800-FDA-1088 orwww.fda.gov/medwatch .
6.1 Clinical Studies Experience
Because clinical trials are conducted under widely varying conditions, adverse reaction rates observed in the clinical trial of a drug cannot be directly compared to rates in the clinical trials of another drug and may not reflect the rates observed in clinical practice.
The information below is derived from a clinical trial database for FANAPT consisting of 3,229 patients exposed to FANAPT at doses of 10 mg/day or greater, for the treatment of schizophrenia and from a clinical trial database for FANAPT consisting of 312 patients exposed to FANAPT at doses of 24 mg/day, for the treatment of bipolar mania [see Clinical Studies (14.2)]. Of these, 999 received FANAPT for at least 6 months, with 657 exposed to FANAPT for at least 12 months for the treatment of schizophrenia and 69 received FANAPT for at least 6 months, with 28 exposed to FANAPT for at least 12 months for the treatment of bipolar mania. All of these patients who received FANAPT were participating in multiple-dose clinical trials. The conditions and duration of treatment with FANAPT varied greatly and included (in overlapping categories), open-label and double-blind phases of studies, inpatients and outpatients, fixed-dose and flexible-dose studies, and short-term and longer-term exposure.
Schizophrenia
The information presented in this section was derived from pooled data from 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies in patients who received FANAPT at daily doses within a range of 10 to 24 mg (n=874).
Adverse Reactions Occurring at an Incidence of 2% or More among FANAPT-Treated Patients and More Frequent than Placebo
Table 3 enumerates the pooled incidences of adverse reactions that were spontaneously reported in four placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies, uling those reactions that occurred in 2% or more of patients treated with FANAPT in any of the dose groups, and for which the incidence in FANAPT- treated patients in any dose group was greater than the incidence in patients treated with placebo.
Table 3: Percentage of Adverse Reactions in Short-Term, Fixed- or Flexible-Dose, Placebo- Controlled Schizophrenia Trials in Adult Patients*
* Table includes adverse reactions that were reported in 2% or more of patients in any of the FANAPT dose groups and which occurred at greater incidence than in the placebo group. Figures rounded to the nearest integer. Body System or Organ Class Placebo(%) FANAPT 10-16 mg/day(%) FANAPT 20-24 mg/day(%) Dictionary-derived Term (N=587) (N=483) (N=391) Body as a Whole       Arthralgia 2 3 3       Fatigue 3 4 6       Musculoskeletal Stiffness 1 1 3       Weight Increased 1 1 9 Cardiac Disorders       Tachycardia 1 3 12 Eye Disorders       Vision Blurred 2 3 1 Gastrointestinal Disorders       Nausea 8 7 10       Dry Mouth 1 8 10       Diarrhea 4 5 7       Abdominal Discomfort 1 1 3 Infections       Nasopharyngitis 3 4 3       Upper Respiratory Tract Infection 1 2 3 Nervous System Disorders       Dizziness 7 10 20       Somnolence 5 9 15       Extrapyramidal Disorder 4 5 4       Tremor 2 3 3       Lethargy 1 3 1 Reproductive System       Ejaculation Failure <1 2 2 Respiratory       Nasal Congestion 2 5 8       Dyspnea <1 2 2 Skin       Rash 2 3 2 Vascular Disorders       Orthostatic Hypotension 1 3 5       Hypotension <1 <1 3
Bipolar Mania
Table 4 enumerates the adverse reactions that occurred at an incidence of ‚Č•2% and greater than placebo in a placebo-controlled, 4-week bipolar mania trial with FANAPT.
Table 4: Adverse Reactions Occurring in ‚Č•2% of Adult Patients Treated with FANAPT and > Placebo in a Short-Term, Fixed-Dose, Placebo-Controlled Bipolar Mania Trial
*The following terms were combined: Tachycardia includes: heart rate increased, sinus tachycardia, postural orthostatic tachycardia syndrome, and tachycardia Nausea includes: nausea and vomiting Hepatic enzyme increased includes: predominantly alanine aminotransferase increased and including aspartate aminotransferase increased, hepatic enzyme increased, and transaminase increased) Weight increased includes: weight increased and BMI increased. Dizziness includes: dizziness and postural dizziness Headache includes: Headache and Tension headache Somnolence includes: predominantly sedation and including sedation complication and somnolence Urinary urgency and Polyuria includes: hypertonic bladder, micturition urgency, polyuria, and urinary incontinence Sexual Dysfunction includes: ejaculation failure, erectile dysfunction, retrograde ejaculation, and ejaculation delayed Hypotension includes: orthostatic hypotension Fatigue includes: lethargy **Patients with poor CYP2D6 metabolizer status received 12 mg/day. System Organ Class Preferred Terms PlaceboN=208% FANAPT 24 mg/day** N=206% Cardiac disorders       Tachycardia* 5 23 Gastrointestinal disorders       Dry mouth 2 9       Nausea* 3 4 Investigations       Hepatic enzyme increased* 1 8       Weight increased* 1 6 Nervous system disorders       Dizziness* 1 12       Headache* 4 5       Somnolence* 3 8       Akathisia 0 4 Renal and urinary disorders       Urinary urgency and Polyuria* 0 3 Reproductive system and breast disorders       Sexual Dysfunction* 0.5 4 Respiratory, thoracic, and mediastinal disorders       Nasal congestion 1 6 Vascular disorders       Hypotension* 3 6 General disorders and administration site conditions       Fatigue* 1 3
Dose-Related Adverse Reactions in Clinical Trials
Based on the pooled data from 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies, adverse reactions in patients with schizophrenia that occurred with a greater than 2% incidence in the patients treated with FANAPT, and for which the incidence in patients treated with FANAPT 20-24 mg/day were twice than the incidence in patients treated with FANAPT 10-16 mg/day were: abdominal discomfort, dizziness, hypotension, musculoskeletal stiffness, tachycardia, and weight increased. 
Common and Drug-Related Adverse Reactions in Clinical Trials
Based on the pooled data from 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies of patients with schizophrenia, the following adverse reactions occurred in ‚Č•5% incidence in the patients treated with FANAPT and at least twice the placebo rate for at least 1 dose: dizziness, dry mouth, fatigue, nasal congestion, somnolence, tachycardia, orthostatic hypotension, and weight increased. Dizziness, tachycardia, and weight increased were at least twice as common on 20-24 mg/day as on 10-16 mg/day.
In a short-term, placebo-controlled trial in patients with bipolar mania the following adverse reactions occurred in ‚Č•5% incidence in the patients treated with FANAPT and at least twice the placebo rate: tachycardia, dizziness, dry mouth, hepatic enzymes increased, nasal congestion, weight increased, hypotension, and somnolence.
Extrapyramidal Symptoms (EPS) in Clinical Trials
Pooled data from the 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies of patients with schizophrenia provided information regarding EPS. Adverse event data collected from those trials showed the following rates of EPS-related adverse events as shown in Table 5.
Table 5: Percentage of EPS Compared to Placebo in 4- or 6-week Schizophrenia Trials
Placebo (%) FANAPT 10-16 mg/day (%) FANAPT 20-24 mg/day (%) Preferred Term (N=587) (N=483) (N=391) All EPS events 11.6 13.5 15.1 Tremor 1.9 2.5 3.1 Akathisia 2.7 1.7 2.3 Dyskinesia 1.5 1.7 1 Dystonia 0.7 1 0.8 Bradykinesia 0 0.6 0.5 Parkinsonism 0 0.2 0.3
Table 6 shows the rates of EPS-related events in a 4-week bipolar mania trial.
Table 6: Percentage of EPS Compared to Placebo in a 4-week Bipolar Mania Trial
*Patients with poor CYP2D6 metabolizer status received 12 mg/day. Preferred Term Placebo (%) FANAPT 24 mg/day* (%) N=208 N=206 All EPS events 0 8.3 Akathisia 0 4.4 Extrapyramidal Disorder 0 1 Blepharospasm 0 0.5 Dystonia 0 0.5 Muscle Spasm 0 0.5 Restlessness 0 0.5 Torticollis 0 0.5 Tremor 0 0.5
Adverse Reactions Associated with Discontinuation of Treatment in Clinical Trials
Based on the pooled data from 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies in patients with schizophrenia, there was no difference in the incidence of discontinuation due to adverse reactions between FANAPT-treated (5%) and placebo-treated (5%) patients. The types of adverse reactions that led to discontinuation were similar for the FANAPT- and placebo-treated patients.
In a 4-week, placebo-controlled study in patients with bipolar mania, the incidence of discontinuation due to adverse reactions was higher in FANAPT-treated (8.7%) patients than placebo-treated (5.3%) patients. Adverse reactions that led to discontinuation in more than one FANAPT-treated subject were liver enzyme elevations, nausea and vomiting, dizziness and hypotension.
Demographic Differences in Adverse Reactions in Clinical Trials
An examination of population subgroups in the 4 placebo-controlled, 4- or 6-week, fixed- or flexible-dose studies of patients with schizophrenia did not reveal any evidence of differences in safety on the basis of age, sex or race.
Laboratory Test Abnormalities in Clinical Trials
There were no differences between FANAPT and placebo in the incidence of discontinuation due to changes in hematology, or urinalysis.
Serum Transaminases
In a short-term placebo-controlled trial, asymptomatic alanine aminotransferase (ALT) elevations ‚Č•3x ULN occurred in 9.2% of FANAPT-treated patients with acute mania compared to 1.5% of placebo treated subjects. AST elevations were less common.
Hematocrit
In short-term placebo-controlled trials (4- to 6-weeks) in patients with schizophrenia, there were 1.0% (13/1342) FANAPT-treated patients with hematocrit at least one time below the extended normal range during post-randomization treatment, compared to 0.3% (2/585) on placebo. The extended normal range for lowered hematocrit was defined in each of these trials as the value 15% below the normal range for the centralized laboratory that was used in the trial. 
In a short-term placebo-controlled trial (4 weeks) in patients with bipolar mania, there were 3.5% (7/200) FANAPT-treated patients with hematocrit at least one time below the extended normal range (<0.85xLLN) during post-randomization treatment, compared to 0.5% (1/196) on placebo.
Analysis of clinical laboratory data following administration of FANAPT suggested the mechanism of hemodilution based on consistent decreases in hematocrit, hemoglobin, white blood cells, total protein, and albumin. Decreases in hematocrit and total protein have been observed with other alpha receptor antagonists and are attributed to hemodilution [see Clinical Pharmacology (12.2)]
Serum Urate Levels
In a 4-week placebo-controlled trial in patients with bipolar mania, treatment with FANAPT 12 mg twice a day resulted in an increase of serum urate levels of approximately 27.2 umol/L (0.457 mg/dL) compared to 0.1 umol/L (0.002 mg/dL) in placebo group.
Other Reactions During the Pre-marketing Evaluation of FANAPT
Patients with Schizophrenia
The following is a ul of MedDRA terms that reflect adverse reactions in patients treated with FANAPT at multiple doses ‚Č• 4 mg/day during any phase of a trial with the database of 3,210 FANAPT-treated patients with schizophrenia. All reported reactions are included except those already uled in Table 3, or other parts of the Adverse Reactions (6) , those considered in the Warnings and Precautions (5) , those reaction terms which were so general as to be uninformative, reactions reported in fewer than 3 patients and which were neither serious nor life-threatening, reactions that are otherwise common as background reactions, and reactions considered unlikely to be drug related.
Reactions are further categorized by MedDRA system organ class and uled in order of decreasing frequency according to the following definitions: frequent adverse events are those occurring in at least 1/100 patients (only those not uled in Table 3 appear in this uling); infrequent adverse reactions are those occurring in 1/100 to 1/1000 patients; rare events are those occurring in fewer than 1/1000 patients.
Blood and Lymphatic Disorders: Infrequent ‚Äď anemia, iron deficiency anemia; Rare ‚Äď leukopenia
Cardiac Disorders: Frequent ‚Äď palpitations; Rare ‚Äď arrhythmia, atrioventricular block first degree, cardiac failure (including congestive and acute)
Ear and Labyrinth Disorders: Infrequent ‚Ästvertigo, tinnitus
Endocrine Disorders: Infrequent ‚Äď hypothyroidism
Eye Disorders: Frequent ‚Äď conjunctivitis (including allergic); Infrequent ‚Ästdry eye, blepharitis, eyelid edema, eye swelling, lenticular opacities, cataract, hyperemia (including conjunctival)
Gastrointestinal Disorders: Infrequent ‚Ästgastritis, salivary hypersecretion,¬†fecal incontinence, mouth ulceration;¬†Rare¬†‚Ästaphthous stomatitis, duodenal ulcer, hiatus hernia, hyperchlorhydria, lip ulceration, reflux esophagitis, stomatitis
General Disorders and Administrative Site Conditions: Infrequent ‚Äď edema (general, pitting, due to cardiac disease), difficulty in walking, thirst; Rare ‚Äď hyperthermia
Hepatobiliary Disorders: Infrequent ‚Äď cholelithiasis
Investigations: Frequent: weight decreased; Infrequent ‚Ästhemoglobin decreased, neutrophil count increased, hematocrit decreased
Metabolism and Nutrition Disorders:¬†Infrequent ‚Äď increased appetite, dehydration, hypokalemia, fluid retention
Musculoskeletal and Connective Tissue Disorders: Frequent ‚Ästmyalgia, muscle spasms; Rare ‚Äď torticollis
Nervous System Disorders:¬†Infrequent¬†‚Ästparesthesia, psychomotor hyperactivity, restlessness, amnesia, nystagmus; Rare ‚Ästrestless legs syndrome
Psychiatric Disorders: Frequent ‚Äď restlessness, aggression, delusion; Infrequent ‚Äď hostility, libido decreased, paranoia, anorgasmia, confusional state, mania, catatonia, mood swings, panic attack, obsessive-compulsive disorder, bulimia nervosa, delirium, polydipsia psychogenic, impulse-control disorder, major depression
Renal and Urinary Disorders: Frequent ‚Äď urinary incontinence; Infrequent ‚Äď dysuria, pollakiuria, enuresis, nephrolithiasis; Rare ‚Äď urinary retention, renal failure acute
Reproductive System and Breast Disorders: Frequent ‚Äď erectile dysfunction; Infrequent ‚Äď testicular pain, amenorrhea, breast pain;¬†Rare ‚Äď menstruation irregular, gynecomastia, menorrhagia, metrorrhagia, postmenopausal hemorrhage, prostatitis
Respiratory, Thoracic and Mediastinal Disorders: Infrequent ‚Äď epistaxis, asthma, rhinorrhea, sinus congestion, nasal dryness; Rare ‚Äď dry throat, sleep apnea syndrome, dyspnea exertional
6.2 Postmarketing Experience
The following adverse reactions have been identified during post-approval use of FANAPT. Because these reactions are reported voluntarily from a population of uncertain size, it is not always possible to estimate their frequency or establish a causal relationship to drug exposure: retrograde ejaculation and hypersensitivity reactions (including anaphylaxis; angioedema; throat tightness; oropharyngeal swelling; swelling of the face, lips, mouth, and tongue; urticaria; rash; and pruritus).
7 Drug Interactions
The dose of FANAPT should be reduced in patients co-administered a strong CYP2D6 or CYP3A4 inhibitor. (2.2 ,7.1 )
7.1 Clinically Important Drug Interactions with FANAPT
Table 7 presents clinically important drug interactions with FANAPT.
Table 7: Clinically Important Drug Interactions with FANAPT
Strong CYP2D6 Inhibitors Clinical Impact
Coadministration of fluoxetine with iloperidone increased exposure (area under curve, [AUC]) of iloperidone and its metabolite P88, by about 2- to 3- fold, and decreased the AUC of its metabolite P95 by one-half [see Clinical Pharmacology (12.3, 12.5)].
Coadministration of paroxetine with iloperidone resulted in increased mean steady-state peak concentrations of iloperidone and its metabolite P88, by about 1.6- fold, and decreased mean steady-state peak concentrations of its metabolite P95 by one-half [see Clinical Pharmacology (12.3, 12.5)].Intervention
Reduce the dose of FANAPT by one-half when administered with strong CYP2D6 inhibitors. When a strong CYP2D6 inhibitor is withdrawn from the combination therapy, the iloperidone dose should be returned to the previous level [see Dosage and Administration (2.4)].
Strong CYP3A4 Inhibitors Clinical Impact
Co-administration of ketoconazole with iloperidone, increased the AUC of iloperidone and its metabolites P88 and P95 by 57%, 55%, and 35%, respectively [see Clinical Pharmacology (12.3)].
Intervention
Reduce the dose of FANAPT by one-half when administered with strong CYP3A4 inhibitors. When the CYP3A4 inhibitor is withdrawn from the combination therapy, the FANAPT dose should be returned to the previous level [see Dosage and Administration (2.4)].
Concomitant use of Strong CYP2D6 and Strong CYP3A4 Inhibitors Clinical Impact
Coadministration of iloperidone with paroxetine and ketoconazole resulted in a 1.4- fold increase in steady-state concentrations of iloperidone and its metabolite P88 and a 1.4- fold decrease in the P95 in the presence of paroxetine [see Clinical Pharmacology (12.3)].
Intervention
Coadministration of FANAPT with inhibitors of both CYP2D6 and CYP3A4 did not add to the effect of either inhibitor given alone. Reduce the dose of FANAPT by about one-half if administered concomitantly with both a CYP2D6 and CYP3A4 inhibitor same as if it is coadministered with only one inhibitor. When the inhibitors of CYP2D6 and CYP3A4 are withdrawn from the combination therapy, the FANAPT dose should be returned to the previous level [see Dosage and Administration (2.4)].
7.2 Drugs that Prolong the QT Interval
Concomitant use of drugs that prolong the QT interval may add to the QT effects of FANAPT and increase the risk of cardiac arrhythmia. Avoid the use of FANAPT in combination with any other drugs that prolong the QT interval [see Warnings and Precautions (5.3)].
7.3Drugs that Lower Blood Pressure
Concomitant use of FANAPT with medications that lower blood pressure could potentially cause symptomatic hypotension. Avoid coadministration of FANAPT with alpha-adrenergic blocking agents and adjust medications that affect blood pressure as needed [see Warnings and Precautions (5.7)].
8 Use In Specific Populations
- Pregnancy: May cause extrapyramidal and/or withdrawal symptoms in neonates with third trimester exposure. (
8.1 )- Lactation: Advise not to breast feed. (
8.2 )- Pediatric Use: Safety and effectiveness not established in children and adolescents. (
8.4 )- Hepatic Impairment: FANAPT is not recommended for patients with severe hepatic impairment. (
2.3 ,8.6 )8.1 Pregnancy
Pregnancy Exposure Registry
There is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to FANAPT during pregnancy. For more information contact the National Pregnancy Registry for Atypical Antipsychotics at 1-866-961-2388 or visit http://womensmentalhealth.org/clinical-and-research-programs/pregnancyregistry/.
Risk Summary
Neonates whose mothers are exposed to antipsychotic drugs, including FANAPT, during the third trimester of pregnancy are at risk for extrapyramidal and/or withdrawal symptoms following delivery [see Clinical Considerations]. The limited available data with FANAPT in pregnant women are not sufficient to inform a drug-associated risk for major birth defects and miscarriage. Iloperidone was not teratogenic when administered orally to pregnant rats during organogenesis at doses up to 26 times the maximum recommended human dose of 24 mg/day on mg/m2 basis. However, it prolonged the duration of pregnancy and parturition, increased still births, early intrauterine deaths, increased incidence of developmental delays, and decreased post-partum pup survival. Iloperidone was not teratogenic when administered orally to pregnant rabbits during organogenesis at doses up to 20-times the MRHD on mg/m2 basis. However, it increased early intrauterine deaths and decreased fetal viability at term at the highest dose which was also a maternally toxic dose [see Data] .
The background risk of major birth defects and miscarriage for the indicated population is unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2 to 4% and 15 to 20%, respectively.
Clinical Considerations
Fetal/Neonatal Adverse Reactions
Extrapyramidal and/or withdrawal symptoms, including agitation, hypertonia, hypotonia, tremor, somnolence, respiratory distress and feeding disorder have been reported in neonates whose mothers were exposed to antipsychotic drugs during the third trimester of pregnancy. These symptoms have varied in severity. Some neonates recovered within hours or days without specific treatment; others required prolonged hospitalization. Monitor neonates for extrapyramidal and/or withdrawal symptoms and manage symptoms appropriately.
Data
Animal Data
In an embryo-fetal development study, pregnant rats were given 4, 16, or 64 mg/kg/day (1.6, 6.5, and 26 times the maximum recommended human dose (MRHD) of 24 mg/day on a mg/m2 basis) of iloperidone orally during the period of organogenesis. The highest dose caused increased early intrauterine deaths, decreased fetal weight and length, decreased fetal skeletal ossification, and an increased incidence of minor fetal skeletal anomalies and variations; this dose also caused decreased maternal food consumption and weight gain.
In an embryo-fetal development study, pregnant rabbits were given 4, 10, or 25 mg/kg/day (3, 8, and 20 times the MRHD on a mg/m2 basis) of iloperidone during the period of organogenesis. The highest dose caused increased early intrauterine deaths and decreased fetal viability at term; this dose also caused maternal toxicity.
In additional studies in which rats were given iloperidone at doses similar to the above beginning from either pre-conception or from day 17 of gestation and continuing through weaning, adverse reproductive effects included prolonged pregnancy and parturition, increased stillbirth rates, increased incidence of fetal visceral variations, decreased fetal and pup weights, and decreased post-partum pup survival. There were no drug effects on the neurobehavioral or reproductive development of the surviving pups. No-effect doses ranged from 4 to 12 mg/kg except for the increase in stillbirth rates which occurred at the lowest dose tested of 4 mg/kg, which is 1.6 times the MRHD on a mg/m2 basis. Maternal toxicity was seen at the higher doses in these studies.
The iloperidone metabolite P95, which is a major circulating metabolite of iloperidone in humans but is not present in significant amounts in rats, was given to pregnant rats during the period of organogenesis at oral doses of 20, 80, or 200 mg/kg/day. No teratogenic effects were seen. Delayed skeletal ossification occurred at all doses. No significant maternal toxicity was produced. Plasma levels of P95 (AUC) at the highest dose tested were 2 times those in humans receiving the MRHD of iloperidone.
8.2Lactation
Risk Summary
There is no information regarding the presence of iloperidone or its metabolites in human milk, the effects of iloperidone on a breastfed child, nor the effects of iloperidone on human milk production. Iloperidone is present in rat milk [seeData ]. Because of the potential for serious adverse reactions in breastfed infants, advise a woman not to breastfeed during treatment with FANAPT.
Data
The transfer of radioactivity into the milk of lactating rats was investigated following a single dose of [14C] iloperidone at 5 mg/kg. The concentration of radioactivity in milk at 4 hours post-dose was near 10-fold greater than that in plasma at the same time. However, by 24 hours after dosing, concentrations of radioactivity in milk had fallen to values slightly lower than plasma. The metabolic profile in milk was qualitatively similar to that in plasma.
8.4Pediatric Use
Safety and effectiveness of FANAPT have not been established in pediatric patients.
8.5Geriatric Use
Clinical Studies of FANAPT in the treatment of schizophrenia did not include sufficient numbers of patients aged 65 years and over to determine whether or not they respond differently than younger adult patients. Of the 3,210 patients with schizophrenia treated with FANAPT in clinical trials, 25 (0.5%) were ‚Č•65 years old and there were no patients ‚Č•75 years old. Of the 206 patients with bipolar mania treated with FANAPT in a clinical trial, 2 (0.1%) were 65 years old and there were no patients were >65 years old.
Elderly patients with dementia-related psychosis treated with FANAPT are at an increased risk of death compared to placebo. FANAPT is not approved for the treatment of patients with dementia-related psychosis [see Boxed Warning and Warnings and Precautions (5.1, 5.2)].
8.6 Hepatic Impairment
No dose adjustment to FANAPT is needed in patients with mild hepatic impairment (Child-Pugh class A). Patients with moderate hepatic impairment (Child-Pugh class B) may require dose reduction. FANAPT is not recommended for patients with severe hepatic impairment (Child-Pugh class C) [see Dosage and Administration (2.3), Clinical Pharmacology (12.3)].
9 Drug Abuse And Dependence
9.1 Controlled Substance
FANAPT is not a controlled substance.
9.2 Abuse
FANAPT has not been systematically studied in animals or humans for its potential for abuse, tolerance, or physical dependence. While the clinical trials did not reveal any tendency for drug-seeking behavior, these observations were not systematic and it is not possible to predict on the basis of this experience the extent to which a CNS active drug, FANAPT, will be misused, diverted, and/or abused once marketed. Consequently, patients should be evaluated carefully for a history of drug abuse, and such patients should be observed closely for signs of FANAPT misuse or abuse (e.g. development of tolerance, increases in dose, drug-seeking behavior).
10 Overdosage
10.1 Human Experience
In pre-marketing trials involving over 3,522 patients, accidental or intentional overdose of FANAPT was documented in 8 patients ranging from 48 mg to 576 mg taken at once and 292 mg taken over a 3-day period. No fatalities were reported from these cases. The largest confirmed single ingestion of FANAPT was 576 mg; no adverse physical effects were noted for this patient. The next largest confirmed ingestion of FANAPT was 438 mg over a 4-day period; extrapyramidal symptoms and a QTc interval of 507 msec were reported for this patient with no cardiac sequelae. This patient resumed FANAPT treatment for an additional 11 months. In general, reported signs and symptoms were those resulting from an exaggeration of the known pharmacological effects (e.g., drowsiness and sedation, tachycardia and hypotension) of FANAPT.
10.2 Management of Overdose
There is no specific antidote for FANAPT. Therefore appropriate supportive measures should be instituted. In case of acute overdose, the healthcare provider should establish and maintain an airway and ensure adequate oxygenation and ventilation. Gastric lavage (after intubation, if patient is unconscious) and administration of activated charcoal together with a laxative should be considered. The possibility of obtundation, seizures or dystonic reaction of the head and neck following overdose may create a risk of aspiration with induced emesis. Cardiovascular monitoring should commence immediately and should include continuous ECG monitoring to detect possible arrhythmias. If antiarrhythmic therapy is administered, disopyramide, procainamide and quinidine should not be used, as they have the potential for QT-prolonging effects that might be additive to those of FANAPT. Similarly, it is reasonable to expect that the alpha-blocking properties of bretylium might be additive to those of FANAPT, resulting in problematic hypotension. Hypotension and circulatory collapse should be treated with appropriate measures such as intravenous fluids or sympathomimetic agents (epinephrine and dopamine should not be used, since beta stimulation may worsen hypotension in the setting of FANAPT-induced alpha blockade). In cases of severe extrapyramidal symptoms, anticholinergic medication should be administered. Close medical supervision should continue until the patient recovers.
Consider contacting the Poison Help Line (1-800-222-1222) or a medical toxicologist for additional overdose management recommendations.
11 Description
FANAPT is an atypical antipsychotic belonging to the chemical class of piperidinyl-benzisoxazole derivatives. Its chemical name is 4’-[3-[4-(6-Fluoro-1,2-benzisoxazol-3-yl)piperidino]propoxy]-3’-methoxyacetophenone. Its molecular formula is C24H27FN2O4 and its molecular weight is 426.48. The structural formula is:
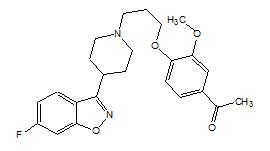
Iloperidone is a white to off-white finely crystalline powder. It is practically insoluble in water, very slightly soluble in 0.1 N HCl and freely soluble in chloroform, ethanol, methanol, and acetonitrile.
FANAPT tablets are intended for oral administration only.¬†Each round, uncoated tablet contains 1 mg, 2 mg, 4 mg, 6 mg, 8 mg, 10 mg, or 12 mg of iloperidone.¬†Inactive ingredients are: lactose monohydrate, microcrystalline cellulose, hydroxypropylmethylcellulose, crospovidone, magnesium stearate, colloidal silicon dioxide, and purified water (removed during processing). The tablets are white, round, flat, beveled-edged, and identified with a logo ‚Äú‚ÄĚ debossed on one side and tablet strength ‚Äú1‚ÄĚ, ‚Äú2‚ÄĚ, ‚Äú4‚ÄĚ, ‚Äú6‚ÄĚ, ‚Äú8‚ÄĚ, ‚Äú10‚ÄĚ, or ‚Äú12‚ÄĚ debossed on the other side.
12 Clinical Pharmacology
12.1 Mechanism of Action
The mechanism of action of iloperidone in schizophrenia and bipolar I disorder is unknown. However, the efficacy of iloperidone could be mediated through a combination of dopamine type 2 (D2) and serotonin type 2 (5-HT2) antagonism. Iloperidone forms an active metabolite, P88, that has an in vitro receptor binding profile similar to the parent drug.
12.2 Pharmacodynamics
Iloperidone acts as an antagonist with high (nM) affinity binding to serotonin 5-HT2A,dopamine D2 and D3 receptors, and norepinephrine NEőĪ1 receptors (Ki values of 5.6, 6.3, 7.1, and 0.36 nM, respectively). Iloperidone has moderate affinity for dopamine D4, and serotonin 5-HT6 and 5-HT7 receptors (Ki values of 25, 43, and 22, nM respectively), and low affinity for the serotonin 5-HT1A, dopamine D1, and histamine H1 receptors (Ki values of 168, 216, and 437 nM, respectively). Iloperidone has no appreciable affinity (Ki >1000 nM) for cholinergic muscarinic receptors. The affinity of iloperidone metabolite P88 is generally equal to or less than that of the parent compound, while the metabolite P95 only shows affinity for 5-HT2A (Ki value of 3.91) and the NEőĪ1A, NEőĪ1B, NEőĪ1D, and NEőĪ2 C receptors (Ki values of 4.7, 2.7, 8.8, and 4.7 nM respectively).¬†
12.3 Pharmacokinetics
The pharmacokinetics of iloperidone is more than dose proportional. Steady-state concentrations are attained within 3 to 4 days of dosing. Iloperidone accumulation is predictable from single-dose pharmacokinetics.
Absorption
Iloperidone is well absorbed after administration of the tablet with time to peak plasma concentrations (Tmax) occurring within 2 to 4 hours. The relative bioavailability of the tablet formulation compared to oral solution is 96%.
Effect of Food
Administration of iloperidone with a standard high-fat meal did not significantly affect the Cmax or AUC of iloperidone, P88, or P95, but delayed Tmax by 1 hour for iloperidone, 2 hours for P88 and 6 hours for P95. FANAPT can be administered without regard to meals.
Distribution
Iloperidone has an apparent volume of distribution of 1340-2800 L. At therapeutic concentrations, the unbound fraction of iloperidone in plasma is ~3% and of each metabolite (P88 and P95) it is ~8%.
Elimination
The observed mean elimination half-lives for iloperidone, P88, and P95 in CYP2D6 extensive metabolizers (EM) are 18, 26, and 23 hours, respectively, and in poor metabolizers (PM) are 33, 37, and 31 hours, respectively.
Iloperidone has an apparent clearance (clearance / bioavailability) of 47 to 102 L/h.
Metabolism
Elimination of iloperidone is mainly through hepatic metabolism. Iloperidone is metabolized primarily by 3 biotransformation pathways: carbonyl reduction, hydroxylation (mediated by CYP2D6) and O-demethylation (mediated by CYP3A4). There are 2 predominant iloperidone metabolites, P95 and P88. The iloperidone metabolite P95 represents 47.9% of the AUC of iloperidone and its metabolites in plasma at steady-state for extensive metabolizers (EM) and 25% for poor metabolizers (PM). The active metabolite P88 accounts for 19.5% and 34.0% of total plasma exposure in EM and PM, respectively.
Approximately 7% - 10% of Caucasians and 3% - 8% of black/African Americans lack the capacity to metabolize CYP2D6 substrates and are classified as poor metabolizers (PM), whereas the rest are intermediate, extensive, or ultrarapid metabolizers.
Excretion
The bulk of the radioactive materials were recovered in the urine (mean 58.2% and 45.1% in EM and PM, respectively), with feces accounting for 19.9% (EM) to 22.1% (PM) of the dosed radioactivity.
Specific Populations
Patients with Renal Impairment
Renal impairment (creatinine clearance <30 mL/min) had minimal effect on Cmax of iloperidone (given in a single dose of 3 mg) and its metabolites P88 and P95 in any of the 3 analytes measured. AUC0‚Äď‚ąě was increased by 24%, decreased by 6%, and increased by 52% for iloperidone, P88 and P95, respectively, in subjects with renal impairment.
Patients with Hepatic Impairment
In adult subjects with mild hepatic impairment, no relevant difference in pharmacokinetics of iloperidone, P88 or P95 (total or unbound) was observed compared to healthy adult controls. In subjects with moderate hepatic impairment a higher (2-fold) and more variable free exposure to the active metabolites P88 was observed compared to healthy controls, whereas exposure to iloperidone and P95 was generally similar (less than 50% change compared to control). Studies with severe liver impaired subjects have not been conducted [see Dosage and Administration (2.3), Use in Specific Populations (8.6)].
Effect of Smoking
Based on in vitro studies utilizing human liver enzymes, FANAPT is not a substrate for CYP1A2; smoking should therefore not have an effect on the pharmacokinetics of FANAPT.
Drug Interactions Studies
CYP2D6 and CYP3A4 Inhibitors
The effects of fluoxetine and ketoconazole on the exposures of FANAPT, P88, and P95 are summarized in Figure 1.
Figure 1: Effect of CYP3A4 and CYP2D6 Inhibitors on the Pharmacokinetics of FANAPT and its Metabolites
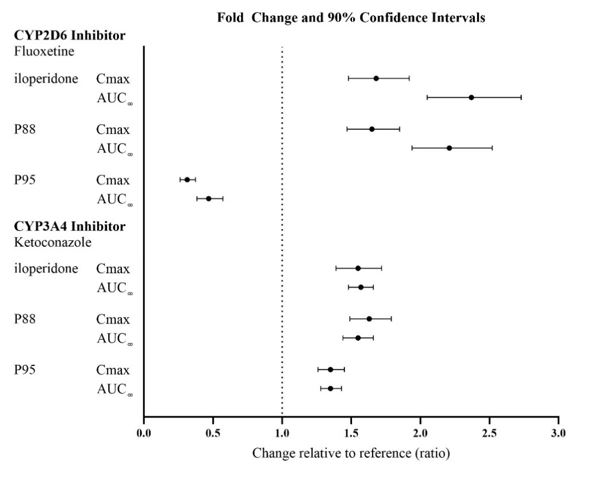
Ketoconazole: Co-administration of ketoconazole (200 mg twice daily for 4 days), a potent inhibitor of CYP3A4, with a 3 mg single dose of iloperidone to 19 healthy volunteers, ages 18-45 years, increased the area under the curve (AUC) of iloperidone and its metabolites P88 and P95 by 57%, 55% and 35%, respectively. Weaker inhibitors (e.g., erythromycin, grapefruit juice) have not been studied.
Fluoxetine: Coadministration of fluoxetine (20 mg twice daily for 21 days), a potent inhibitor of CYP2D6, with a single 3 mg dose of iloperidone to 23 healthy volunteers, ages 29-44 years, who were classified as CYP2D6 extensive metabolizers, increased the AUC of iloperidone and its metabolite P88, by about 2- to 3- fold, and decreased the AUC of its metabolite P95 by one-half.
Paroxetine: Coadministration of paroxetine (20 mg/day for 5-8 days), a potent inhibitor of CYP2D6, with multiple doses of iloperidone (8 or 12 mg twice daily) to patients with schizophrenia ages 18-65 years resulted in increased mean steady-state peak concentrations of iloperidone and its metabolite P88, by about 1.6 fold, and decreased mean steady-state peak concentrations of its metabolite P95 by one-half.
Paroxetine and Ketoconazole: Coadministration of paroxetine (20 mg once daily for 10 days), a CYP2D6 inhibitor, and ketoconazole (200 mg twice daily) with multiple doses of iloperidone (8 or 12 mg twice daily) to patients with schizophrenia ages 18-65 years resulted in a 1.4 fold increase in steady-state concentrations of iloperidone and its metabolite P88 and a 1.4 fold decrease in the P95 in the presence of paroxetine.
Dextromethorphan: A study in healthy volunteers showed that changes in the pharmacokinetics of dextromethorphan (80 mg dose) when a 3 mg dose of iloperidone was co-administered resulted in a 17% increase in total exposure and a 26% increase in the maximum plasma concentrations Cmax of dextromethorphan. Thus, an interaction between iloperidone and other CYP2D6 substrates is unlikely.
Fluoxetine: A single 3 mg dose of iloperidone had no effect on the pharmacokinetics of fluoxetine (20 mg twice daily).
Midazolam (a sensitive CYP 3A4 substrate): A study in patients with schizophrenia showed a less than 50% increase in midazolam total exposure at iloperidone steady state (14 days of oral dosing at up to 10 mg iloperidone twice daily) and no effect on midazolam Cmax. Thus, an interaction between iloperidone and other CYP3A4 substrates is unlikely.
In Vitro Studies
Based on the in vitro data, iloperidone is not a substrate for CYP1A1, CYP1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, CYP2C19, or CYP2E1 enzymes. This suggests that an interaction of iloperidone with inhibitors or inducers of these enzymes, or other factors, like smoking, is unlikely.
In vitro studies in human liver microsomes showed that iloperidone does not substantially inhibit the metabolism of drugs metabolized by the following cytochrome P450 isozymes: CYP1A1, CYP1A2, CYP2A6, CYP2B6, CYP2C8, CYP2C9, or CYP2E1. Furthermore, in vitro studies in human liver microsomes showed that iloperidone does not have enzyme inducing properties, specifically for the following cytochrome P450 isozymes: CYP1A2, CYP2C8, CYP2C9, CYP2C19, CYP3A4 and CYP3A5.
Transporter Interaction: Iloperidone and P88 are not substrates of P-gp and iloperidone is a weak P-gp inhibitor.
12.5 Pharmacogenomics
CYP2D6 Poor Metabolizer (PM): The gene encoding CYP2D6 has polymorphisms that impact protein function. CYP2D6 poor metabolizers are individuals with two non-functioning alleles, resulting in no enzyme activity.
Pharmacokinetic data from CYP2D6 poor metabolizers (n=8) treated with iloperidone demonstrated an increase in the AUC of iloperidone and its metabolite P88 by 47% and 85%, respectively and decrease the AUC of metabolite P95 by 85% compared to normal metabolizers (n=18) [see Dosage and Administration (2.2)].
Approximately 7% of White populations, 2% of Asian populations, and 2% of African-American populations are poor metabolizers.
13 Nonclinical Toxicology
13.1 Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis: Lifetime carcinogenicity studies were conducted in CD-1 mice and Sprague Dawley rats. Iloperidone was administered orally at doses of 2.5, 5.0, and 10 mg/kg/day to CD-1 mice and 4, 8, and 16 mg/kg/day to Sprague Dawley rats (0.5, 1.0, and 2.0 times and 1.6, 3.2, and 6.5 times, respectively, the MRHD of 24 mg/day on a mg/m2 basis). There was an increased incidence of malignant mammary gland tumors in female mice treated with the lowest dose (2.5 mg/kg/day) only. There were no treatment-related increases in neoplasia in rats.
The carcinogenic potential of the iloperidone metabolite P95, which is a major circulating metabolite of iloperidone in humans but is not present at significant amounts in mice or rats, was assessed in a lifetime carcinogenicity study in Wistar rats at oral doses of 25, 75, and 200 mg/kg/day in males and 50, 150, and 250 (reduced from 400) mg/kg/day in females. Drug-related neoplastic changes occurred in males, in the pituitary gland (pars distalis adenoma) at all doses and in the pancreas (islet cell adenoma) at the high dose. Plasma levels of P95 (AUC) in males at the tested doses (25, 75, and 200 mg/kg/day) were approximately 0.4, 3, and 23 times, respectively, the human exposure to P95 at the MRHD of iloperidone.
Mutagenesis: Iloperidone was negative in the Ames test and in the in vivo mouse bone marrow and rat liver micronucleus tests. Iloperidone induced chromosomal aberrations in Chinese Hamster Ovary (CHO) cells in vitro at concentrations which also caused some cytotoxicity. 
The iloperidone metabolite P95 was negative in the Ames test, the V79 chromosome aberration test, and an in vivo mouse bone marrow micronucleus test.
Impairment of Fertility: Iloperidone decreased fertility at 12 and 36 mg/kg in a study in which both male and female rats were treated. The no-effect dose was 4 mg/kg, which is 1.6 times the MRHD of 24 mg/day on a mg/m2 basis.
14 Clinical Studies
14.1Schizophrenia
The efficacy of FANAPT in the treatment of schizophrenia was supported by 2 placebo- and active-controlled short-term (4- and 6-week) trials and one long-term placebo-controlled randomized withdrawal trial. All trials enrolled patients who met the DSM-III/IV criteria for schizophrenia. 
Three instruments were used for assessing psychiatric signs and symptoms in these studies. The Positive and Negative Syndrome Scale (PANSS) and Brief Psychiatric Rating Scale (BPRS) are both multi-li inventories of general psychopathology usually used to evaluate the effects of drug treatment in schizophrenia. The Clinical Global Impression (CGI) assessment reflects the impression of a skilled observer, fully familiar with the manifestations of schizophrenia, about the overall clinical state of the patient.
Study 1, a 6-week, placebo-controlled trial (n=706), involved 2 flexible dose ranges of FANAPT (12 mg to 16 mg/day or 20 mg to 24 mg/day) compared to placebo and an active control (risperidone). For the 12 mg to 16 mg/day group, the titration schedule of FANAPT was 1 mg twice daily on Days 1 and 2, 2 mg twice daily on Days 3 and 4, 4 mg twice daily on Days 5 and 6, and 6 mg twice daily on Day 7. For the 20 mg to 24 mg/day group, the titration schedule of FANAPT was 1 mg twice daily on Day 1, 2 mg twice daily on Day 2, 4 mg twice daily on Day 3, 6 mg twice daily on Days 4 and 5, 8 mg twice daily on Day 6, and 10 mg twice daily on Day 7. The primary endpoint was change from baseline on the BPRS total score at the end of treatment (Day 42). Both the 12 mg to 16 mg/day and the 20 mg to 24 mg/day dose ranges of FANAPT were superior to placebo on the BPRS total score. The active control antipsychotic drug appeared to be superior to FANAPT in this trial within the first 2 weeks, a finding that may in part be explained by the more rapid titration that was possible for that drug. In patients in this study who remained on treatment for at least 2 weeks, iloperidone appeared to have had comparable efficacy to the active control.
Study 2 (NCT00254202), a 4-week, placebo-controlled trial (n=604), involved one fixed-dose of FANAPT (24 mg/day) compared to placebo and an active control (ziprasidone). The titration schedule for this study was similar to that for the 6-week study. This study involved titration of FANAPT starting at 1 mg twice daily on Day 1 and increasing to 2, 4, 6, 8, 10, and 12 mg twice daily on Days 2, 3, 4, 5, 6, and 7. The primary endpoint was change from baseline on the PANSS total score at the end of treatment (Day 28). The 24 mg/day FANAPT dose was superior to placebo in the PANSS total score. FANAPT appeared to have similar efficacy to the active control drug which also needed a slow titration to the target dose.
In a longer-term trial (Study 3; NCT01291511), clinically stable adult outpatients (n=303) meeting DSM-IV criteria for schizophrenia who remained stable following 12 weeks of open-label treatment with flexible doses of FANAPT (8 mg to 24 mg/day administered as twice daily doses) were randomized to placebo or to continue on their current FANAPT dose (8 mg to 24 mg/day administered as twice daily doses) for observation for possible relapse during the double-blind relapse prevention phase. Stabilization during the open-label phase was defined as being on an established dose of FANAPT that was unchanged due to efficacy in the 4 weeks prior to randomization, having CGI-Severity score of ‚ȧ4 and PANSS total score ‚ȧ70, a score of ‚ȧ4 on each of the following individual PANSS lis (P1-delusions, P2-conceptual disorganization, P3-hallucinatory behavior, P6-suspiciousness/persecution, P7-hostility, or G8-uncooperativeness), and no hospitalization or increase in level of care to treat exacerbations. Relapse or impending relapse during the double-blind relapse prevention phase was defined as any of the following: hospitalization due to worsening of schizophrenia, increase (worsening) of the PANSS total score ‚Č•30%, CGI-Improvement score ‚Č•6, patient had suicidal, homicidal, or aggressive behavior, or need for any other antipsychotic medication.
Figure 2: Kaplan Meier Estimation of Percent Relapse/Impending Relapse (Study 3)
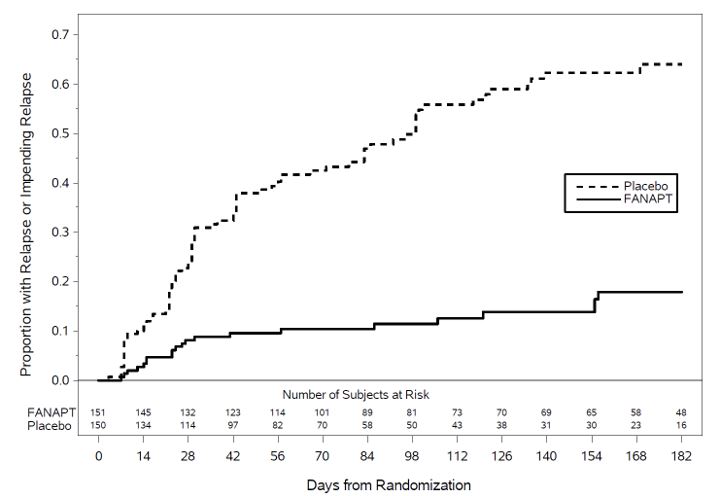
Based on the interim analysis, an independent data monitoring committee decided the study should be discontinued early due to evidence of efficacy. Based on results from the interim analysis, which were confirmed by the final analysis dataset, patients treated with FANAPT experienced a statistically significant longer time to relapse or impending relapse than patients who received placebo. Figure 2 displays the estimated cumulative proportion of patients with relapse or impending relapse based on the final data set.
14.2Manic or Mixed Episodes Associated with Bipolar I Disorder
The efficacy of FANAPT in the acute treatment of manic or mixed episodes associated with bipolar I disorder in adults was supported by one multicenter, randomized, double-blind, placebo-controlled study that enrolled patients who met the DSM-5 criteria for bipolar I disorder, manic or mixed type (Study 1; NCT04819776). Demographic and baseline characteristics were similar for the FANAPT and placebo groups. Median age was 46 (range 18 to 65). 45% were female, 64% were White, and 28% were Black or African-American.
Manic symptoms were assessed with the Young Mania Rating Scale (YMRS). The YMRS is an 11-li clinician rated scale traditionally used to assess the degree of manic symptomatology. YMRS total scores may range from 0 to 60 with a higher score reflecting greater severity.
A 4-week, placebo-controlled trial (n=392) involved one fixed-dose of FANAPT (24 mg/day) compared to placebo. The primary endpoint was change in YMRS total score from baseline to Day 28. The 24 mg/day dose of FANAPT was superior to placebo on the primary endpoint. Examination of subgroups did not reveal clear evidence of differential responsiveness on the basis of age, sex, or race.
The results of the study are shown in Table 8. The LS mean changes from baseline in YMRS total score are shown in Figure 3.
Table 8: Primary Efficacy Results for Change from Baseline in YMRS Total Score in the Acute Treatment of Manic or Mixed Episodes Associated with Bipolar I Disorder in Adults (Study 1)
ITT = intent-to-treat,YMRS = Young Mania Rating Scale, LS mean = Least Squares mean, SD = standard deviation, SE = standard error aDifference (drug minus placebo) in least-squares mean change from baseline *Dose was superior to placebo StudyNumber Treatment Group(# ITT patients) Primary Efficacy Endpoint: Change from Baseline to Day 28 inYMRS Total Score MeanBaselineScore (SD) LS MeanChange fromBaseline (SE) Placebo-substractedDifferencea (95% CI) 1 FANAPT (24 mg/day)* (n=198) 29.2 (5.27) -14.0 (0.64) -4.0 (-5.70, -2.25) Placebo(n=194) 28.8 (4.64) -10.0 (0.63) Figure 3: Change from Baseline in YMRS Total Score by Study Visit (Study 1)
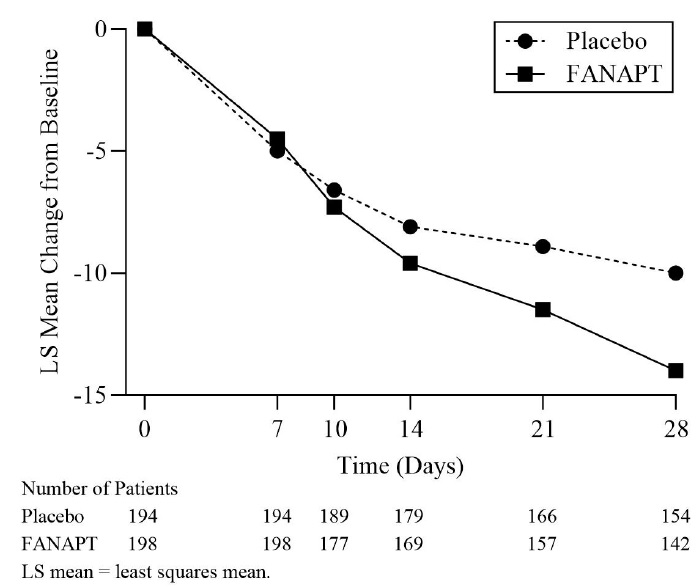
16 How Supplied/storage And Handling
FANAPT tablets are white, round and identified with a logo ‚Äú‚ÄĚ debossed on one side and tablet strength ‚Äú1‚ÄĚ, ‚Äú2‚ÄĚ, ‚Äú4‚ÄĚ, ‚Äú6‚ÄĚ, ‚Äú8‚ÄĚ, ‚Äú10‚ÄĚ, or ‚Äú12‚ÄĚ debossed on the other side. Tablets are supplied in the following strengths and package configurations:
Package Configuration Tablet Strength (mg) NDC Code Bottles of 60 1 mg 43068-101-02 Bottles of 60 2 mg 43068-102-02 Bottles of 60 4 mg 43068-104-02 Bottles of 60 6 mg 43068-106-02 Bottles of 60 8 mg 43068-108-02 Bottles of 60 10 mg 43068-110-02 Bottles of 60 12 mg 43068-112-02 Titration Pack 2x1 mg, 2x2 mg, 2x4 mg, 2x6 mg(Total of 8 tablets) 43068-113-04
Storage
Store FANAPT tablets at controlled room temperature, 25‚ĄÉ (77‚ĄČ); excursions permitted to 15¬į to 30 ‚ĄÉ (59¬į to 86‚ĄČ) [See USP Controlled Room Temperature]. Protect FANAPT tablets from exposure to light and moisture.
17 Patient Counseling Information
QT Interval Prolongation
Patients should be advised to consult their healthcare provider immediately if they feel faint, lose consciousness or have heart palpitations. Patients should be counseled not to take FANAPT with other drugs that cause QT interval prolongation [see Warnings and Precautions (5.3)]. Patients should be told to inform their healthcare provider that they are taking FANAPT before any new drug is taken.
Neuroleptic Malignant Syndrome (NMS)
Counsel patients and caregivers about a potentially fatal adverse reaction, NMS, that has been reported with administration of antipsychotic drugs, including FANAPT. Advise patients and caregivers to contact the healthcare provider or to report to the emergency room if they experience signs and symptoms of NMS [see Warnings and Precautions (5.4)].
Tardive Dyskinesia
Counsel patients on the signs and symptoms of tardive dyskinesia and to contact their healthcare provider if these abnormal movements occur [see Warnings and Precautions (5.5)].
Metabolic Changes
Educate patients of metabolic changes, how to recognize symptoms of hyperglycemia and diabetes mellitus, and the need for specific monitoring, including blood glucose, lipids, and weight. Patients should be counseled that weight gain has occurred during treatment with FANAPT [see Warnings and Precautions (5.6)].
Orthostatic Hypotension and Syncope
Educate patients about the risk of orthostatic hypotension and syncope, particularly at the time of initiating treatment, re-initiating treatment, or increasing the dose [see Warnings and Precautions (5.7)].
Leukopenia/Neutropenia
Advise patients with a pre-existing low WBC or a history of drug induced leukopenia/neutropenia that they should have their CBC monitored while taking FANAPT [see Warnings and Precautions (5.10)].
Heat Exposure and Dehydration
Educate patients regarding appropriate care in avoiding overheating and dehydration [see Warnings and Precautions (5.12)].
Interference with Cognitive and Motor Performance
Caution patients about performing activities requiring mental alertness, such as operating hazardous machinery or operating a motor vehicle, until they are reasonably certain that FANAPT therapy does not affect them adversely [see (Warnings and Precautions (5.15)].
Intraoperative Floppy Iris Syndrome
Instruct patients to tell their ophthalmologist about their use of FANAPT before cataract surgery or other procedures involving the eyes, even if the patient is no longer taking FANAPT [see Warnings and Precautions (5.16)].
Pregnancy
Advise patients that third trimester use of FANAPT may cause extrapyramidal and/or withdrawal symptoms in a neonate. Advise patients to notify their healthcare provider with known or suspected pregnancy [see Use in Specific Populations (8.1)].
Pregnancy Registry
Advise patients that there is a pregnancy exposure registry that monitors pregnancy outcomes in women exposed to FANAPT during pregnancy [see Use in Specific Populations (8.1)].
Lactation
Advise women not to breastfeed during treatment with FANAPT [see Use in Specific Populations (8.2)].
Concomitant Medication
Advise patients to inform their healthcare provider if they are taking, or plan to take, any prescription or over-the-counter drugs, since there is a potential for interactions [see Drug Interactions (7)].
Alcohol
Patients should be advised to avoid alcohol while taking FANAPT.
Distributed by:
Vanda Pharmaceuticals Inc.
Washington, D.C. 20037 USA
Vanda and Fanapt¬ģ are registered trademarks of Vanda Pharmaceuticals Inc. in the United States and other countries.
Principal Display Panel - Ndc: 43068-101-02 - 1mg Label
Principal Display Panel - Ndc: 43068-102-02 - 2mg Label
Principal Display Panel - Ndc: 43068-104-02 - 4mg Label
Principal Display Panel - Ndc: 43068-106-02 - 6mg Label
Principal Display Panel - Ndc: 43068-108-02 - 8mg Label
Principal Display Panel - Ndc: 43068-110-02 - 10mg Label
Principal Display Panel - Ndc: 43068-112-02 - 12mg Label
Principal Display Panel - Ndc: 43068-113-04 Titration Pack
Principal Display Panel - Ndc: 43068-901-14 - 6mg Carton
Principal Display Panel - Ndc: 43068-901-14 - 6mg Bottle
Principal Display Panel - Ndc: 43068-902-14 - 8mg Carton
Principal Display Panel - Ndc: 43068-902-14 - 8mg Bottle
Principal Display Panel - Ndc: 43068-903-08 Titration Pack
Principal Display Panel - Ndc: 43068-905-14 - 1mg Carton
Principal Display Panel - Ndc: 43068-905-14 - 1mg Bottle
Principal Display Panel - Ndc: 43068-904-14 - 2mg Carton
Principal Display Panel - Ndc: 43068-904-14 - 2mg Bottle
DISCLAIMER:
"This tool does not provide medical advice, and is for informational and educational purposes only, and is not a substitute for professional medical advice, treatment or diagnosis. Call your doctor to receive medical advice. If you think you may have a medical emergency, please dial 911."
"Do not rely on openFDA to make decisions regarding medical care. While we make every effort to ensure that data is accurate, you should assume all results are unvalidated. We may limit or otherwise restrict your access to the API in line with our Terms of Service."
"This product uses publicly available data from the U.S. National Library of Medicine (NLM), National Institutes of Health, Department of Health and Human Services; NLM is not responsible for the product and does not endorse or recommend this or any other product."
PillSync may earn a commission via links on our site