Marbeta 25 Kit Dailymed
Generic: betamethasone sodium phosphate and betamethasone acetate, bupivacaine hydrochloride, povidine iodine is used for the treatment of Pain Pain, Postoperative
Boxed Warning
Warning: Risk Of Cardiac Arrest With Use Of Bupivacaine Hydrochloride Injection In Obstetrical Anesthesia
Go PRO for all pill images
Warning: Risk Of Cardiac Arrest With Use Of Bupivacaine Hydrochloride Injection In Obstetrical Anesthesia
There have been reports of cardiac arrest with difficult resuscitation or death during use of Bupivacaine Hydrochloride Injection for epidural anesthesia in obstetrical patients. In most cases, this has followed use of the 0.75% (7.5 mg/mL) concentration. Resuscitation has been difficult or impossible despite apparently adequate preparation and appropriate management. Cardiac arrest has occurred after convulsions resulting from systemic toxicity, presumably following unintentional intravascular injection. The 0.75% (7.5 mg/mL) concentration of Bupivacaine Hydrochloride Injection is not recommended for obstetrical anesthesia and should be reserved for surgical procedures where a high degree of muscle relaxation and prolonged effect are necessary [see Warnings and Precautions (5.1)].
WARNING: RISK OF CARDIAC ARREST WITH USE OF BUPIVACAINE HYDROCHLORIDE INJECTION IN OBSTETRICAL ANESTHESIA
See full prescribing information for complete boxed warning.
There have been reports of cardiac arrest with difficult resuscitation or death during use of Bupivacaine Hydrochloride Injection for epidural anesthesia in obstetrical patients. In most cases, this has followed use of the 0.75% (7.5 mg/mL) concentration. Resuscitation has been difficult or impossible despite apparently adequate preparation and appropriate management. Cardiac arrest has occurred after convulsions resulting from systemic toxicity, presumably following unintentional intravascular injection. The 0.75% (7.5 mg/mL) concentration of Bupivacaine Hydrochloride Injection is not recommended for obstetrical anesthesia and should be reserved for surgical procedures where a high degree of muscle relaxation and prolonged effect are necessary (5.1 ).
1 Indications And Usage
Bupivacaine Hydrochloride Injection is indicated in adults for the production of local or regional anesthesia or analgesia for surgery, dental and oral surgery procedures, diagnostic and therapeutic procedures, and for obstetrical procedures. Specific concentrations and presentations of Bupivacaine Hydrochloride Injection are recommended for each type of block indicated to produce local or regional anesthesia or analgesia [see Dosage and Administration (2.2)].
Bupivacaine Hydrochloride Injection contains bupivacaine, an amide local anesthetic. Bupivacaine Hydrochloride Injection is indicated in adults for the production of local or regional anesthesia or analgesia for surgery, dental and oral surgery procedures, diagnostic and therapeutic procedures, and for obstetrical procedures. For each type of block indicated to produce local or regional anesthesia or analgesia, specific concentrations and presentations are recommended. (1 ,2.2 )
Limitations of Use
Not all blocks are indicated for use with Bupivacaine Hydrochloride Injection given clinically significant risks associated with use. (1 ,2.2 ,4 ,5.1 ,5.4 ,5.5 ,5.7 ,5.9 )
Limitations of Use
Not all blocks are indicated for use with Bupivacaine Hydrochloride Injection given clinically significant risks associated with use [see Dosage and Administration (2.2), Contraindications (4), Warnings and Precautions (5.1, 5.4, 5.5, 5.7, 5.9)] .
2 Dosage And Administration
- Not for intrathecal use. (
2.1 )- Avoid use of solutions containing antimicrobial preservatives (i.e., multiple-dose vials) for epidural or caudal anesthesia. (
2.1 ,5.4 )- Three mL of Bupivacaine Hydrochloride and Epinephrine Injection without antimicrobial preservative (0.5% bupivacaine with 1:200,000 epinephrine) is recommended for use as a test dose prior to caudal and lumbar epidural blocks when clinical conditions permit. (
2.4 )- See full prescribing information for:
- Recommended concentrations and dosages of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection according to type of block. (
2.2 )- Additional dosage and administration information pertaining to use in epidural anesthesia, test dose for caudal and lumbar epidural blocks, use in dentistry, and use in ophthalmic surgery. (
2.3 ,2.4 ,2.5 ,2.6 )2.1Important Dosage and Administration Information
- Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is not for intrathecal use.
- Avoid use of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection solutions containing antimicrobial preservatives (i.e., multiple-dose vials) for epidural or caudal anesthesia [see Warnings and Precautions (5.4)] .
- Discard unused portions of solution not containing preservatives, i.e., those supplied in single-dose vials, following initial use.
- Visually inspect this product for particulate matter and discoloration prior to administration whenever solution and container permit. Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection are clear, colorless solutions. Do not administer solutions which are discolored or contain particulate matter.
- Mixing or the prior or intercurrent use of any other local anesthetic with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is not recommended because of insufficient data on the clinical use of such mixtures.
Administration Precautions
- Bupivacaine Hydrochloride Injection Injection/Bupivacaine Hydrochloride and Epinephrine Injection are to be administered in carefully adjusted dosages by or under the supervision of experienced clinicians who are well versed in the diagnosis and management of dose-related toxicity and other acute emergencies which might arise from the block to be employed.
- Use Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection only if the following are immediately available: oxygen, cardiopulmonary resuscitative equipment and drugs, and the personnel resources needed for proper management of toxic reactions and related emergencies [see Warnings and Precautions (5.2), Adverse Reactions (6), Overdosage (10)] .
- The toxic effects of local anesthetics are additive. Monitor for neurologic and cardiovascular effects related to local anesthetic systemic toxicity when additional local anesthetics are administered with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection [see Warnings and Precautions (5.2), Drug Interactions (7.1), Overdosage (10)] .
- Aspirate for blood or cerebrospinal fluid (where applicable) prior to injecting Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, both the initial dose and all subsequent doses, to avoid intravascular or intrathecal injection. However, a negative aspiration for blood or cerebrospinal fluid does not ensure against an intravascular or intrathecal injection [see Warnings and Precautions (5.9)] .
- Avoid rapid injection of a large volume of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection and use fractional (incremental) doses when feasible.
- During major regional nerve blocks, such as those of the brachial plexus or lower extremity, the patient should have an indwelling intravenous catheter to assure adequate intravenous access. The lowest dosage of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection that results in effective anesthesia should be used to avoid high plasma levels and serious adverse reactions.
- Perform careful and constant monitoring of cardiovascular and respiratory (adequacy of oxygenation and ventilation) vital signs and the patient's level of consciousness after each local anesthetic injection.
- Use Bupivacaine Hydrochloride and Epinephrine Injection in carefully restricted quantities in areas of the body supplied by end arteries or having otherwise compromised blood supply such as digits, nose, external ear, or penis [see Warnings and Precautions (5.12)] .
2.2Recommended Concentrations and Dosages of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection
The dosage of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection administered varies with the anesthetic procedure, the area to be anesthetized, the vascularity of the tissues, the number of neuronal segments to be blocked, the depth of anesthesia and degree of muscle relaxation required, the duration of anesthesia desired, individual tolerance, and the physical condition of the patient. Administer the smallest dosage and concentration required to produce the desired result.
The types of block and recommended Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection concentrations are shown in Table 1.
Table 1. Types of Block and Recommended Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection Concentrations Type of Block Bupivacaine Hydrochloride Bupivacaine Hydrochloride and Epinephrine 0.25% (2.5 mg/mL) 0.5% (5 mg/mL) 0.75% (7.5 mg/mL) Bupivacaine Hydrochloride Injection 0.75% (7.5 mg/mL) is not recommended for nonobstetrical surgical procedures in pregnant patients. 0.25% (2.5 mg/mL) 0.5% (5 mg/mL) âś“= indicated use [see Warnings and Precautions (5.1)]. Local infiltration âś“ âś“ Peripheral nerve block âś“ âś“ âś“ âś“ Retrobulbar block âś“ Sympathetic block âś“ Caudal block Avoid use of multiple-dose vials of Bupivacaine Hydrochloride Injection and Bupivacaine Hydrochloride and Epinephrine Injection for caudal or epidural anesthesia [see Warnings and Precautions (5.4)] . âś“ âś“ âś“ âś“ Lumbar epidural block âś“ âś“ âś“ (not for obstetrical anesthesia) âś“ âś“ Epidural test dose âś“ Dental block âś“
At recommended dosages, Bupivacaine Hydrochloride/Bupivacaine Hydrochloride and Epinephrine produces complete sensory block, but the effect on motor function differs among the three concentrations. Table 2 provides information on the expected effect on motor function for the three concentrations.
Table 2. Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection Concentration vs. Motor Function Bupivacaine Hydrochloride Injection Concentration Motor Function 0.25% (2.5 mg/mL) These products include Bupivacaine Hydrochloride Injection and Bupivacaine Hydrochloride and Epinephrine Injection [the epinephrine concentration (1:200,000) is not included in the table]. When used for caudal, epidural, or peripheral nerve block, produces incomplete motor block. Should be used for operations in which muscle relaxation is not important, or when another means of providing muscle relaxation is used concurrently. Onset of action may be slower than with the 0.5% (5 mg/mL) or 0.75% (7.5 mg/mL) solutions. 0.5% (5 mg/mL) Provides motor blockade for caudal, epidural, or nerve block, but muscle relaxation may be inadequate for operations in which complete muscle relaxation is essential. 0.75% (7.5 mg/mL) These are only Bupivacaine Hydrochloride Injection products [there is no 0.75% (7.5 mg/mL) concentration for Bupivacaine Hydrochloride and Epinephrine Injection]. Produces complete motor block. Most useful for epidural block in abdominal operations requiring complete muscle relaxation, and for retrobulbar anesthesia. Not for obstetrical anesthesia.
The duration of anesthesia with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is such that for most indications, a single-dose is sufficient.
The maximum dosage limit within the recommended dosage range must be individualized in each case after evaluating the size and physical status of the patient, as well as the anticipated rate of systemic absorption from a particular injection site.
The dosages in Table 3 are recommended as a guide for use in the average adult. These doses may be repeated once every three hours. Do not exceed a total daily dosage of 400 mg in 24 hours. The duration of anesthetic effect may be prolonged by the addition of epinephrine.
Table 3. Recommended Concentrations and Doses of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection in Adults Type of Block Concentration of Bupivacaine Hydrochloride Injection Each Dose Motor Block With continuous (intermittent) techniques, repeat doses increase the degree of motor block. The first repeat dose of 0.5% (5 mg/mL) may produce complete motor block. Intercostal nerve block with 0.25% (2.5 mg/mL) also may produce complete motor block for intra-thoracic and upper intra-abdominal surgery. mL mg of Bupivacaine Hydrochloride Injection Local infiltration 0.25% (2.5 mg/mL) Solutions with or without epinephrine (i.e., applies to Bupivacaine Hydrochloride Injection and Bupivacaine Hydrochloride and Epinephrine Injection). The Bupivacaine Hydrochloride and Epinephrine Injection products include epinephrine (1:200,000). Up to 70 (without epinephrine) Up to 175 (without epinephrine) ― Up to 90 (with epinephrine) Up to 225 (with epinephrine) Peripheral nerve block 0.5% (5 mg/mL) 5–35 (without epinephrine) 25–175 (without epinephrine) moderate to complete 5–45 (with epinephrine) 25–225 (with epinephrine) 0.25% (2.5 mg/mL) 5–70 (without epinephrine) 12.5–175 (without epinephrine) moderate to complete 5–90 (with epinephrine) 12.5–225 (with epinephrine) Retrobulbar block [see Dosage and Administration (2.6)] 0.75% (7.5 mg/mL) 2–4 15–30 complete Sympathetic block 0.25% (2.5 mg/mL) 20–50 50–125 ― Caudal block [see Dosage and Administration (2.4)] 0.5% (5 mg/mL) 15–30 75–150 moderate to complete 0.25% (2.5 mg/mL) 15–30 37.5–75 moderate Lumbar epidural block [see Dosage and Administration (2.3)] 0.75% (7.5 mg/mL) For single-dose use; not for intermittent epidural technique. Not for obstetrical anesthesia. 10–20 75–150 complete 0.5% (5 mg/mL) 10–20 50–100 moderate to complete 0.25% (2.5 mg/mL) 10–20 25–50 partial to moderate Epidural test dose [see Dosage and Administration (2.4)] 0.5% (5 mg/mL) with epinephrine 2–3 10–15 (10–15 micrograms epinephrine) ― Dental [see Dosage and Administration (2.5)] 0.5% (5 mg/mL) with epinephrine 1.8–3.6 per site 9–18 per site ― 2.3Use in Epidural Anesthesia
During the administration of epidural anesthesia, it is recommended that a test dose of Bupivacaine Hydrochloride and Epinephrine Injection without antimicrobial preservative (0.5% bupivacaine with 1:200,000 epinephrine) be administered initially and the effects monitored before the full dose is given. When using a "continuous" catheter technique, test doses should be given prior to both the initial and all supplemental doses, because a catheter in the epidural space can migrate into a blood vessel or through the dura [see Dosage and Administration (2.4)] .
During epidural administration, administer Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, 0.5% (5 mg/mL) and Bupivacaine Hydrochloride Injection 0.75% (7.5 mg/mL) solutions in incremental doses of 3 mL to 5 mL with sufficient time between doses to detect toxic manifestations of unintentional intravascular or intrathecal injection. Administer injections slowly, with frequent aspirations before and during the injection to avoid intravascular injection. Perform syringe aspirations before and during each supplemental injection in continuous (intermittent) catheter techniques. In obstetrics, use ONLY the 0.5% (5 mg/mL) and 0.25% (2.5 mg/mL) concentrations of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection [see Warnings and Precautions (5.1)]; incremental doses of 3 mL to 5 mL of the 0.5% (5 mg/mL) solution not exceeding 50 mg to 100 mg at any dosing interval are recommended. Repeat doses should be preceded by a test dose containing epinephrine if not clinically contraindicated. Use only the single-dose vials for caudal or epidural anesthesia; avoid use of the multiple-dose vials for these procedures, which contain a preservative [see Dosage and Administration (2.1, 2.4), Warnings and Precautions (5.4, 5.9)] .
2.4Test Dose for Caudal and Lumbar Epidural Blocks
Three mL of Bupivacaine Hydrochloride and Epinephrine Injection without antimicrobial preservative (0.5% bupivacaine with 1:200,000 epinephrine) is recommended for use as a test dose prior to caudal and lumbar epidural blocks when clinical conditions permit. This test dose may serve as a warning of unintended intravascular or intrathecal injection. Closely monitor for early clinical signs of toxicity following each test dose [see Warnings and Precautions (5.9)] . Allot adequate time for onset of spinal block to detect possible intrathecal injection. An intravascular or intrathecal injection is still possible even if results of the test dose are negative. The test dose itself may produce a systemic toxic reaction, high spinal, or cardiovascular effects from the epinephrine [see Warnings and Precautions (5.2, 5.9), Overdosage (10)].
2.5Use in Dentistry
Bupivacaine Hydrochloride and Epinephrine Injection 0.5% (5 mg/mL) is recommended for infiltration and block injection in the maxillary and mandibular area when a longer duration of local anesthesia is desired, such as for procedures generally associated with significant postoperative pain. The average dose of 1.8 mL (9 mg) per injection site will usually suffice; an occasional second dose of 1.8 mL (9 mg) may be used if necessary to produce adequate anesthesia after allowing 2 to 10 minutes for block onset [see Clinical Pharmacology (12.2)]. Use the lowest effective dose and allow time between injections; it is recommended that the total dose for all injection sites, spread out over a single dental sitting, not exceed 90 mg for a healthy adult patient (ten 1.8 mL injections of 0.5% (5 mg/mL) Bupivacaine Hydrochloride and Epinephrine Injection). Inject slowly and with frequent aspirations.
2.6Use in Ophthalmic Surgery
When Bupivacaine Hydrochloride Injection 0.75% (7.5 mg/mL) is used for retrobulbar block, complete corneal anesthesia usually precedes onset of clinically acceptable external ocular muscle akinesia. Therefore, presence of akinesia rather than anesthesia alone should determine readiness of the patient for surgery [see Warnings and Precautions (5.15)] .
3 Dosage Forms And Strengths
Bupivacaine Hydrochloride Injection, USP is a clear, colorless solution available as:
- 0.25% (25 mg/10 mL) (2.5 mg/mL) in single-dose teartop vials.
- 0.25% (75 mg/30 mL) (2.5 mg/mL) in single-dose teartop vials.
- 0.25% (125 mg/50 mL) (2.5 mg/mL) in multiple-dose fliptop vials.
- 0.5% (50 mg/10 mL) (5 mg/mL) in single-dose teartop vials.
- 0.5% (150 mg/30 mL) (5 mg/mL) in single-dose teartop vials.
- 0.5% (250 mg/50 mL) (5 mg/mL) in multiple-dose fliptop vials.
- 0.75% (75 mg/10 mL) (7.5 mg/mL) in single-dose teartop vials.
- 0.75% (225 mg/30 mL) (7.5 mg/mL) in single-dose teartop vials.
Bupivacaine Hydrochloride Injection, USP are available in multiple concentrations. See full prescribing information for detailed description of each formulation. (3 )
4 Contraindications
Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is contraindicated in:
- obstetrical paracervical block anesthesia. Its use in this technique has resulted in fetal bradycardia and death.
- intravenous regional anesthesia (Bier Block) [see Warnings and Precautions (5.7)].
- patients with a known hypersensitivity to bupivacaine or to any local anesthetic agent of the amide-type or to other components of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection.
- Obstetrical paracervical block anesthesia. Its use in this technique has resulted in fetal bradycardia and death. (
4 )- Intravenous regional anesthesia (Bier Block). (
4 )- Known hypersensitivity to bupivacaine or to any local anesthetic agent of the amide-type or to other components of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection. (
4 )
5 Warnings And Precautions
- Dose-Related Toxicity: Monitor cardiovascular and respiratory vital signs and patient's state of consciousness after injection of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection. (
5.2 )- Methemoglobinemia: Cases of methemoglobinemia have been reported in association with local anesthetic use. See full prescribing information for more detail on managing these risks. (
5.3 )- Chondrolysis with Intra-Articular Infusion: Intra-articular infusions of local anesthetics including Bupivacaine Hydrochloride Injection following arthroscopic and other surgical procedures is an unapproved use, and there have been post-marketing reports of chondrolysis in patients receiving such infusions. (
5.5 )- Risk of Cardiac Arrest with Intravenous Regional Anesthesia Use (Bier Block): There have been reports of cardiac arrest and death during the use of bupivacaine for intravenous regional anesthesia (Bier Block). (
5.7 )- Allergic-Type Reactions to Sulfites in Bupivacaine Hydrochloride and Epinephrine Injection: Bupivacaine Hydrochloride and Epinephrine Injection contains sodium metabisulfite, a sulfite that may cause allergic-type reactions including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. (
5.8 )- Risk of Systemic Toxicities with Unintended Intravascular or Intrathecal Injection: Unintended intravascular or intrathecal injection may be associated with systemic toxicities, including CNS or cardiorespiratory depression and coma, progressing ultimately to respiratory arrest. Aspirate for blood or cerebrospinal fluid (where applicable) prior to each dose and consider using a test dose of Bupivacaine Hydrochloride and Epinephrine Injection. (
5.9 )5.1Risk of Cardiac Arrest with Use of Bupivacaine Hydrochloride Injection in Obstetrical Anesthesia
There have been reports of cardiac arrest with difficult resuscitation or death during use of Bupivacaine Hydrochloride Injection for epidural anesthesia in obstetrical patients. In most cases, this has followed use of the 0.75% (7.5 mg/mL) concentration. Resuscitation has been difficult or impossible despite apparently adequate preparation and appropriate management. Cardiac arrest has occurred after convulsions resulting from systemic toxicity, presumably following unintentional intravascular injection. The 0.75% (7.5 mg/mL) concentration of Bupivacaine Hydrochloride Injection is not recommended for obstetrical anesthesia and should be reserved for surgical procedures where a high degree of muscle relaxation and prolonged effect are necessary.
5.2Dose-Related Toxicity
The safety and effectiveness of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection depend on proper dosage, correct technique, adequate precautions, and readiness for emergencies. Careful and constant monitoring of cardiovascular and respiratory (adequacy of ventilation) vital signs and the patient's state of consciousness should be performed after injection of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection solutions.
Possible early warning signs of central nervous system (CNS) toxicity are restlessness, anxiety, incoherent speech, lightheadedness, numbness and tingling of the mouth and lips, metallic taste, tinnitus, dizziness, blurred vision, tremors, twitching, CNS depression, or drowsiness. Delay in proper management of dose-related toxicity, underventilation from any cause, and/or altered sensitivity may lead to the development of acidosis, cardiac arrest, and, possibly, death.
During major regional nerve blocks, such as those of the brachial plexus or lower extremity, the patient should have an indwelling intravenous catheter to assure adequate intravenous access. Use the lowest dosage of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection that results in effective anesthesia to avoid high plasma levels and serious adverse effects. Avoid rapid injection of a large volume of Bupivacaine. Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection solution and administer fractional (incremental) doses when feasible.
Injection of repeated doses of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection may cause significant increases in plasma levels with each repeated dose due to slow accumulation of the drug or its metabolites, or to slow metabolic degradation. Tolerance to elevated blood levels varies with the status of the patient. Debilitated, elderly patients and acutely ill patients should be given reduced doses commensurate with their age and physical status.
5.3Methemoglobinemia
Cases of methemoglobinemia have been reported in association with local anesthetic use. Although all patients are at risk for methemoglobinemia, patients with glucose-6-phosphate dehydrogenase deficiency, congenital or idiopathic methemoglobinemia, cardiac or pulmonary compromise, infants under 6 months of age, and concurrent exposure to oxidizing agents or their metabolites are more susceptible to developing clinical manifestations of the condition [see Drug Interactions (7.5)] . If local anesthetics must be used in these patients, close monitoring for symptoms and signs of methemoglobinemia is recommended.
Signs of methemoglobinemia may occur immediately or may be delayed some hours after exposure, and are characterized by a cyanotic skin discoloration and/or abnormal coloration of the blood. Methemoglobin levels may continue to rise; therefore, immediate treatment is required to avert more serious CNS and cardiovascular adverse effects, including seizures, coma, arrhythmias, and death. Discontinue Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection and any other oxidizing agents. Depending on the severity of the signs and symptoms, patients may respond to supportive care, i.e., oxygen therapy, hydration. A more severe clinical presentation may require treatment with methylene blue, exchange transfusion, or hyperbaric oxygen.
5.4Antimicrobial Preservatives in Multiple-Dose Vials
Avoid use of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection solutions containing antimicrobial preservatives, i.e., those supplied in multiple-dose vials, for epidural or caudal anesthesia because safety has not been established with such use.
5.5Chondrolysis with Intra-Articular Infusion
Intra-articular infusions of local anesthetics including Bupivacaine Hydrochloride Injection following arthroscopic and other surgical procedures is an unapproved use, and there have been post-marketing reports of chondrolysis in patients receiving such infusions. The majority of reported cases of chondrolysis have involved the shoulder joint; cases of gleno-humeral chondrolysis have been described in pediatric and adult patients following intra-articular infusions of local anesthetics with and without epinephrine for periods of 48 to 72 hours. There is insufficient information to determine whether shorter infusion periods are associated with chondrolysis. The time of onset of symptoms, such as joint pain, stiffness and loss of motion can be variable, but may begin as early as the 2 nd month after surgery. Currently, there is no effective treatment for chondrolysis; patients who experienced chondrolysis have required additional diagnostic and therapeutic procedures and some required arthroplasty or shoulder replacement.
5.6Risk of Adverse Reactions Due to Drug Interactions with Bupivacaine Hydrochloride and Epinephrine Injection
Risk of Severe, Persistent Hypertension Due to Drug Interactions Between Bupivacaine Hydrochloride and Epinephrine Injection and Monoamine Oxidase Inhibitors and Tricyclic Antidepressants
Administration of Bupivacaine Hydrochloride and Epinephrine Injection (containing a vasoconstrictor) in patients receiving monoamine oxidase inhibitors (MAOI), or tricyclic antidepressants may result in severe, prolonged hypertension. Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful monitoring of the patient's hemodynamic status is essential [see Drug Interactions (7.2)].
Risk of Severe, Persistent Hypertension or Cerebrovascular Accidents Due to Drug Interactions Between Bupivacaine Hydrochloride and Epinephrine Injection and Ergot-Type Oxytocic Drugs
Concurrent administration of Bupivacaine Hydrochloride and Epinephrine Injection and ergot-type oxytocic drugs may cause severe, persistent hypertension or cerebrovascular accidents. Avoid use of Bupivacaine Hydrochloride and Epinephrine Injection concomitantly with ergot-type oxytocic drugs [see Drug Interactions (7.3)] .
Risk of Hypertension and Bradycardia Due to Drug Interactions Between Bupivacaine Hydrochloride and Epinephrine Injection and Nonselective Beta-Adrenergic Antagonists
Administration of Bupivacaine Hydrochloride and Epinephrine Injection (containing a vasoconstrictor) in patients receiving nonselective beta-adrenergic antagonists may cause severe hypertension and bradycardia. Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful monitoring of the patient's blood pressure and heart rate is essential [see Drug Interactions (7.4)] .
5.7Risk of Cardiac Arrest with Intravenous Regional Anesthesia Use (Bier Block)
There have been reports of cardiac arrest and death during the use of bupivacaine for intravenous regional anesthesia (Bier Block). Information on safe dosages and techniques of administration of Bupivacaine Hydrochloride Injection in this procedure is lacking. Therefore, Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is contraindicated for use with this technique [see Contraindications (4)] .
5.8Allergic-Type Reactions to Sulfites in Bupivacaine Hydrochloride and Epinephrine Injection
Bupivacaine Hydrochloride and Epinephrine Injection contains sodium metabisulfite, a sulfite that may cause allergic-type reactions including anaphylactic symptoms and life-threatening or less severe asthmatic episodes in certain susceptible people. The overall prevalence of sulfite sensitivity in the general population is unknown and probably low. Sulfite sensitivity is seen more frequently in asthmatic than in nonasthmatic people. Bupivacaine Hydrochloride Injection without epinephrine does not contain sodium metabisulfite.
5.9Risk of Systemic Toxicities with Unintended Intravascular or Intrathecal Injection
Unintended intravascular or intrathecal injection of. Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection may be associated with systemic toxicities, including CNS or cardiorespiratory depression and coma, progressing ultimately to respiratory arrest. Unintentional intrathecal injection during the intended performance of caudal or lumbar epidural block or nerve blocks near the vertebral column has resulted in underventilation or apnea ("Total or High Spinal"). A high spinal has been characterized by paralysis of the legs, loss of consciousness, respiratory paralysis, and bradycardia [see Adverse Reactions (6)] .
Aspirate for blood or cerebrospinal fluid (where applicable) before injecting Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, both the initial dose and all subsequent doses, to avoid intravascular or intrathecal injection. However, a negative aspiration for blood or cerebrospinal fluid does not ensure against an intravascular or intrathecal injection.
Use of Test Dose with Epidural Anesthesia
To serve as a warning of unintended intravascular or intrathecal injection, 3 mL of Bupivacaine Hydrochloride and Epinephrine Injection without antimicrobial preservative (0.5% bupivacaine with 1:200,000 epinephrine) may be used as a test dose prior to administration of the full dose in caudal and lumbar epidural blocks [see Dosage and Administration (2.4)] . Three mL of Bupivacaine Hydrochloride and Epinephrine Injection without antimicrobial preservative (0.5% bupivacaine with 1:200,000 epinephrine) contains 15 mg bupivacaine and 15 mcg epinephrine. An intravascular or intrathecal injection is still possible even if results of the test dose are negative.
Signs/symptoms of unintended intravascular or intrathecal injection of the test dose of Bupivacaine Hydrochloride and Epinephrine Injection and monitoring recommendations are described below.
- Unintended intravascular injection: Likely to produce a transient "epinephrine response" within 45 seconds, consisting of an increase in heart rate and/or systolic blood pressure, circumoral pallor, palpitations, and nervousness in the unsedated patient. The sedated patient may exhibit only a pulse rate increase of 20 or more beats per minute for 15 or more seconds. Therefore, following the test dose, the heart rate should be monitored for increases. Patients on beta-blockers may not manifest changes in heart rate, but blood pressure monitoring can detect a transient rise in systolic blood pressure.
- Unintended intrathecal injection: Evidenced within a few minutes by signs of spinal block (e.g., decreased sensation of the buttocks, paresis of the legs, or, in the sedated patient, absent knee jerk).
The test dose itself may produce a systemic toxic reaction, high spinal or epinephrine-induced cardiovascular effects [see Overdosage (10)] .
5.10Risk of Toxicity in Patients with Hepatic Impairment
Because amide local anesthetics such as bupivacaine are metabolized by the liver, consider reduced dosing and increased monitoring for bupivacaine systemic toxicity in patients with moderate to severe hepatic impairment who are treated Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, especially with repeat doses [see Use in Specific Populations (8.6)].
5.11Risk of Use in Patients with Impaired Cardiovascular Function
Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection should be given in reduced doses in patients with impaired cardiovascular function (e.g., hypotension, heartblock) because they may be less able to compensate for functional changes associated with the prolongation of AV conduction produced by Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection. Monitor patients closely for blood pressure, heart rate, and ECG changes.
5.12Risk of Ischemic Injury or Necrosis in Body Areas with Limited Blood Supply
Use Bupivacaine Hydrochloride and Epinephrine Injection in carefully restricted quantities in areas of the body supplied by end arteries or having otherwise compromised blood supply such as digits, nose, external ear, or penis. Patients with hypertensive vascular disease may exhibit exaggerated vasoconstrictor response. Ischemic injury or necrosis may result.
5.13Risk of Cardiac Arrhythmias with Concomitant Use of Potent Inhalation Anesthetics
Serious dose-related cardiac arrhythmias may occur if preparations containing a vasoconstrictor such as epinephrine (e.g., Bupivacaine Hydrochloride and Epinephrine Injection) are used in patients during or following the administration of potent inhalation anesthetics [see Drug Interactions (7.6)] . In deciding whether to concurrently use Bupivacaine Hydrochloride and Epinephrine Injection with potent inhalation anesthetics in the same patient, the combined action of both agents upon the myocardium, the concentration and volume of vasoconstrictor used, and the time since injection, when applicable, should be taken into account.
5.14Risk of Adverse Reactions with Use in Head and Neck Area
Small doses of local anesthetics (e.g., Bupivacaine Hydrochloride Injection) injected into the head and neck area, including retrobulbar, dental, and stellate ganglion blocks, may produce adverse reactions similar to systemic toxicity seen with unintentional intravascular injections of larger doses. The injection procedures require the utmost care. Confusion, convulsions, respiratory depression, and/or respiratory arrest, and cardiovascular stimulation or depression have been reported. These reactions may be due to intra-arterial injection of the local anesthetic with retrograde flow to the cerebral circulation. They may also be due to puncture of the dural sheath of the optic nerve during retrobulbar block with diffusion of any local anesthetic along the subdural space to the midbrain. Monitor circulation and respiration and constantly observe patients receiving Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection blocks. Resuscitative equipment and drugs, and personnel for treating adverse reactions should be immediately available. Dosage recommendations should not be exceeded [see Dosage and Administration (2.2)].
5.15Risk of Respiratory Arrest with Use in Ophthalmic Surgery
Clinicians who perform retrobulbar blocks should be aware that there have been reports of respiratory arrest following local anesthetic injection. Prior to retrobulbar block (e.g., with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection), as with all other regional procedures, resuscitative equipment and drugs, and personnel to manage respiratory arrest or depression, convulsions, and cardiac stimulation or depression should be immediately available [see Warnings and Precautions (5.14)]. As with other anesthetic procedures, patients should be constantly monitored following ophthalmic blocks for signs of these adverse reactions, which may occur following relatively low total doses.
A concentration of 0.75% bupivacaine is indicated for retrobulbar block; however, this concentration is not indicated for any other peripheral nerve block, including the facial nerve, and not indicated for local infiltration, including the conjunctiva [see Indications and Usage (1)].
5.16Risk of Inadvertent Trauma to Tongue, Lips, and Buccal Mucosa in Dental Applications
Because of the long duration of anesthesia, when Bupivacaine Hydrochloride and Epinephrine Injection [0.5% (5 mg/mL) of bupivacaine] is used for dental injections, warn patients about the possibility of inadvertent trauma to tongue, lips, and buccal mucosa and advise them not to chew solid foods until sensation returns [see Patient Counseling Information (17)] .
6 Adverse Reactions
The following clinically significant adverse reactions have been reported and described in the Warnings and Precautions section of the labeling:
- Cardiac Arrest in Obstetrical Anesthesia [see Warnings and Precautions (5.1)]
- Dose-Related Toxicity [see Warnings and Precautions (5.2)]
- Methemoglobinemia [see Warnings and Precautions (5.3)]
- Chondrolysis with Intra-Articular Infusion [see Warnings and Precautions (5.5)]
- Severe, Persistent Hypertension, Cerebrovascular Accidents, and Bradycardia Due to Drug Interactions [see Warnings and Precautions (5.6)]
- Cardiac Arrest with Intravenous Regional Anesthesia Use [see Contraindications (4), Warnings and Precautions (5.7)]
- Allergic-Type Reactions [see Warnings and Precautions (5.8)]
- Systemic Toxicities with Unintended Intravascular or Intrathecal Injection [see Warnings and Precautions (5.9)]
- Respiratory Arrest Following Retrobulbar Block [see Warnings and Precautions (5.15)]
The following adverse reactions from voluntary reports or clinical studies have been reported with bupivacaine or bupivacaine and epinephrine. Because many of these reactions were reported voluntarily from a population of uncertain size, it is not always possible to reliably estimate their frequency or establish a causal relationship to drug exposure.
Adverse reactions to Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection are characteristic of those associated with other amide-type local anesthetics. A major cause of adverse reactions to this group of drugs is excessive plasma levels, which may be due to overdosage, unintentional intravascular injection, or slow metabolic degradation.
The most commonly encountered acute adverse reactions that demand immediate counter-measures were related to the CNS and the cardiovascular system. These adverse reactions were generally dose-related and due to high plasma levels which may have resulted from overdosage, rapid absorption from the injection site, diminished tolerance, or from unintentional intravascular injection of the local anesthetic solution. In addition to systemic dose-related toxicity, unintentional intrathecal injection of drug during the intended performance of caudal or lumbar epidural block or nerve blocks near the vertebral column (especially in the head and neck region) has resulted in underventilation or apnea ("Total or High Spinal"). Also, hypotension due to loss of sympathetic tone and respiratory paralysis or underventilation due to cephalad extension of the motor level of anesthesia have occurred. This has led to secondary cardiac arrest when untreated.
Most common adverse reactions are related to the central nervous system and the cardiovascular system. (6 )
To report SUSPECTED ADVERSE REACTIONS, contact Pfizer Inc. at 1-800-438-1985 or FDA at 1-800-FDA-1088 or www.fda.gov/medwatch.
Nervous System Disorders
Adverse reactions were characterized by excitation and/or depression of the central nervous system and included restlessness, anxiety, dizziness, tinnitus, blurred vision, tremors, convulsions, drowsiness, unconsciousness, respiratory arrest, nausea, vomiting, chills, pupillary constriction.
In the practice of caudal or lumbar epidural block, unintentional penetration of the subarachnoid space by the catheter or needle has occurred. Subsequent adverse effects may have depended partially on the amount of drug administered intrathecally and the physiological and physical effects of a dural puncture. A high spinal has been characterized by paralysis of the legs, loss of consciousness, respiratory paralysis, and bradycardia.
Neurologic effects following epidural or caudal anesthesia have included spinal block of varying magnitude (including high or total spinal block); hypotension secondary to spinal block; urinary retention; fecal and urinary incontinence; loss of perineal sensation and sexual function; persistent anesthesia, paresthesia, weakness, paralysis of the lower extremities and loss of sphincter control, all of which had slow, incomplete, or no recovery; headache; backache; septic meningitis; meningismus; slowing of labor; increased incidence of forceps delivery; and cranial nerve palsies due to traction on nerves from loss of cerebrospinal fluid.
Neurologic effects following other procedures or routes of administration have included persistent anesthesia, paresthesia, weakness, paralysis, all with slow, incomplete, or no recovery.
Convulsions: Incidence varied with the procedure used and the total dose administered. In a survey of studies of epidural anesthesia, overt toxicity progressing to convulsions occurred in approximately 0.1% of local anesthetic administrations. The incidences of adverse neurologic reactions associated with the use of local anesthetics may be related to the total dose of local anesthetic administered and are also dependent upon the particular drug used, the route of administration, and the physical status of the patient.
Cardiac Disorders
High doses or unintentional intravascular injection have led to high plasma levels and related depression of the myocardium, decreased cardiac output, heartblock, hypotension, bradycardia, ventricular arrhythmias, including ventricular tachycardia and ventricular fibrillation, and cardiac arrest [see Warnings and Precautions (5.9)].
Immune System Disorders
Allergic-type reactions have occurred as a result of sensitivity to bupivacaine or to other formulation ingredients, such as the antimicrobial preservative methylparaben contained in multiple-dose vials or sulfites in epinephrine-containing solutions. These reactions were characterized by signs such as urticaria, pruritus, erythema, angioneurotic edema (including laryngeal edema), tachycardia, sneezing, nausea, vomiting, dizziness, syncope, excessive sweating, elevated temperature, and severe hypotension. Cross sensitivity among members of the amide-type local anesthetic group has been reported [see Warnings and Precautions (5.8)] .
7 Drug Interactions
- Local Anesthetics: The toxic effects of local anesthetics are additive. Monitor for neurologic and cardiovascular effects when additional local anesthetics are administered. (
7.1 )- Monoamine Oxidase Inhibitors and Tricyclic Antidepressants: Administration of Bupivacaine Hydrochloride and Epinephrine Injection to patients receiving monoamine oxidase inhibitors or tricyclic antidepressants may produce severe, prolonged hypertension. Concurrent use of these agents should generally be avoided. (
5.6 ,7.2 )- Ergot-Type Oxytocic Drugs: Concurrent administration of Bupivacaine Hydrochloride and Epinephrine Injection and ergot-type oxytocic drugs may cause severe, persistent hypertension or cerebrovascular accidents. (
5.6 ,7.3 )- Nonselective Beta-Adrenergic Antagonists: Administration of Bupivacaine Hydrochloride and Epinephrine Injection (containing a vasoconstrictor) in patients receiving nonselective beta-adrenergic antagonists may cause severe hypertension and bradycardia. Concurrent use of these agents should generally be avoided. (
5.6 ,7.4 )- Drugs Associated with Methemoglobinemia: Patients are at increased risk of developing methemoglobinemia when concurrently exposed to nitrates, nitrites, local anesthetics, antineoplastic agents, antibiotics, antimalarials, anticonvulsants, and other drugs. (
7.5 )- Potent Inhalation Anesthetics: Serious dose-related cardiac arrhythmias may occur if preparations containing a vasoconstrictor such as epinephrine are used in patients during or following the administration of potent inhalation anesthetics. (
5.13 ,7.6 )7.1Local Anesthetics
The toxic effects of local anesthetics are additive. If coadministration of other local anesthetics with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection cannot be avoided, monitor patients for neurologic and cardiovascular effects related to local anesthetic systemic toxicity [see Dosage and Administration (2.1), Warnings and Precautions (5.2)] .
7.2Monoamine Oxidase Inhibitors and Tricyclic Antidepressants
The administration Bupivacaine Hydrochloride and Epinephrine Injection to patients receiving monoamine oxidase inhibitors, or tricyclic antidepressants may produce severe, prolonged hypertension. Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful monitoring of the patient's hemodynamic status is essential [see Warnings and Precautions (5.6)] .
7.3Ergot-Type Oxytocic Drugs
Concurrent administration of Bupivacaine Hydrochloride and Epinephrine Injection and ergot-type oxytocic drugs may cause severe, persistent hypertension or cerebrovascular accidents. Avoid use of Bupivacaine Hydrochloride and Epinephrine concomitantly with ergot-type oxytocic drugs [see Warnings and Precautions (5.6)].
7.4Nonselective Beta-Adrenergic Antagonists
Administration of Bupivacaine Hydrochloride and Epinephrine Injection (containing a vasoconstrictor) in patients receiving nonselective beta-adrenergic antagonists may cause severe hypertension and bradycardia. Concurrent use of these agents should generally be avoided. In situations when concurrent therapy is necessary, careful monitoring of the patient's blood pressure and heart rate is essential [see Warnings and Precautions (5.6)].
7.5Drugs Associated with Methemoglobinemia
Patients who are administered Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection are at increased risk of developing methemoglobinemia when concurrently exposed to following drugs, which could include other local anesthetics [see Warnings and Precautions (5.3)] .
Examples of Drugs Associated with Methemoglobinemia: Class Examples Nitrates/Nitrites nitric oxide, nitroglycerin, nitroprusside, nitrous oxide Local anesthetics articaine, benzocaine, bupivacaine, lidocaine, mepivacaine, prilocaine, procaine, ropivacaine, tetracaine Antineoplastic agents cyclophosphamide, flutamide, hydroxyurea, isofamide, rasburicase Antibiotics dapsone, nitrofurantoin, para-aminosalicylic acid, sulfonamides Antimalarials chloroquine, primaquine Anticonvulsants phenobarbital, phenytoin, sodium valproate Other drugs acetaminophen, metoclopramide, quinine, sulfasalazine 7.6Potent Inhalation Anesthetics
Serious dose-related cardiac arrhythmias may occur if preparations containing a vasoconstrictor such as epinephrine (e.g., Bupivacaine Hydrochloride and Epinephrine Injection) are used in patients during or following the administration of potent inhalation anesthetics [see Warnings and Precautions (5.13)] .
7.7Phenothiazines and Butyrophenones
Phenothiazines and butyrophenones may reduce or reverse the pressor effect of epinephrine. Concurrent use of Bupivacaine Hydrochloride and Epinephrine Injection and these agents should generally be avoided. In situations when concurrent therapy is necessary, careful patient monitoring is essential.
8 Use In Specific Populations
- Pediatric Use: Administration of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection in pediatric patients younger than 12 years is not recommended. (
8.4 )- Geriatric Use: Patients 65 years and over, particularly those with hypertension, may be at increased risk for developing hypotension while undergoing anesthesia with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection. (
8.5 )- Moderate to Severe Hepatic Impairment: Consider increased monitoring for bupivacaine systemic toxicity. (
8.6 )8.1Pregnancy
Risk Summary
Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is contraindicated for obstetrical paracervical block anesthesia. Its use in this technique has resulted in fetal bradycardia and death [see Contraindications (4), Warnings and Precautions (5.1)].
There are no available data on use of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection in pregnant women to inform a drug-associated risk of adverse developmental outcomes.
In animal studies, embryo-fetal lethality was noted when bupivacaine was administered subcutaneously to pregnant rabbits during organogenesis at clinically relevant doses. Decreased pup survival was observed in a rat pre- and post-natal developmental study (dosing from implantation through weaning) at a dose level comparable to the daily maximum recommended human dose (MRHD) on a body surface area (BSA) basis. Based on animal data, advise pregnant women of the potential risks to a fetus (see Data).
Local anesthetics rapidly cross the placenta, and when used for epidural, caudal, or pudendal block anesthesia, can cause varying degrees of maternal, fetal, and neonatal toxicity [see Clinical Pharmacology (12.3)]. The incidence and degree of toxicity depend upon the procedure performed, the type, and amount of drug used, and the technique of drug administration. Adverse reactions in the parturient, fetus, and neonate involve alterations of the CNS, peripheral vascular tone, and cardiac function.
If this drug is used during pregnancy, or if the patient becomes pregnant while taking this drug, inform the patient of the potential hazard to the fetus. The estimated background risk of major birth defects and miscarriage for the indicated populations are unknown. In the U.S. general population, the estimated background risk of major birth defects and miscarriage in clinically recognized pregnancies is 2–4% and 15–20%, respectively.
Clinical Considerations
Maternal Adverse Reactions
Maternal hypotension has resulted from regional anesthesia. Local anesthetics produce vasodilation by blocking sympathetic nerves. The supine position is dangerous in pregnant women at term because of aortocaval compression by the gravid uterus. Therefore, during treatment of systemic toxicity, maternal hypotension or fetal bradycardia following regional block, the parturient should be maintained in the left lateral decubitus position if possible, or manual displacement of the uterus off the great vessels be accomplished. Elevating the patient's legs will also help prevent decreases in blood pressure. The fetal heart rate also should be monitored continuously and electronic fetal monitoring is highly advisable.
Labor or Delivery
Epidural, caudal, or pudendal anesthesia may alter the forces of parturition through changes in uterine contractility or maternal expulsive efforts. Epidural anesthesia has been reported to prolong the second stage of labor by removing the parturient's reflex urge to bear down or by interfering with motor function. The use of obstetrical anesthesia may increase the need for forceps assistance.
The use of some local anesthetic drug products during labor and delivery may be followed by diminished muscle strength and tone for the first day or two of life. This has not been reported with bupivacaine.
It is extremely important to avoid aortocaval compression by the gravid uterus during administration of regional block to parturients. To do this, the patient must be maintained in the left lateral decubitus position or a blanket roll or sandbag may be placed beneath the right hip and gravid uterus displaced to the left.
Data
Animal Data
Bupivacaine hydrochloride produced developmental toxicity when administered subcutaneously to pregnant rats and rabbits at clinically relevant doses.
Bupivacaine hydrochloride was administered subcutaneously to rats at doses of 4.4, 13.3, & 40 mg/kg and to rabbits at doses of 1.3, 5.8, & 22.2 mg/kg during the period of organogenesis (implantation to closure of the hard palate). The high doses are comparable to the daily MRHD of 400 mg/day on a mg/m 2 BSA basis. No embryo-fetal effects were observed in rats at the high dose which caused increased maternal lethality. An increase in embryo-fetal deaths was observed in rabbits at the high dose in the absence of maternal toxicity with the fetal No Observed Adverse Effect Level representing approximately 0.3 times the MRHD on a BSA basis.
In a rat pre-and post-natal developmental study (dosing from implantation through weaning) conducted at subcutaneous doses of 4.4, 13.3, & 40 mg/kg, decreased pup survival was observed at the high dose. The high dose is comparable to the daily MRHD of 400 mg/day on a BSA basis.
8.2Lactation
Risk Summary
Lactation studies have not been conducted with bupivacaine. Bupivacaine has been reported to be excreted in human milk suggesting that the nursing infant could be theoretically exposed to a dose of the drug. Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection should be administered to lactating women only if clearly indicated. Studies assessing the effects of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection in breastfed children have not been performed. Studies to assess the effect of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection on milk production or excretion have not been performed. The developmental and health benefits of breastfeeding should be considered along with the mother's clinical need for bupivacaine and any potential adverse effects on the breastfed child from bupivacaine or from the underlying maternal condition.
8.4Pediatric Use
Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection is approved for use in adults. Administration of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection in pediatric patients younger than 12 years is not recommended.
Continuous infusions of bupivacaine in pediatric patients have been reported to result in high systemic levels of bupivacaine and seizures; high plasma levels may also be associated with cardiovascular abnormalities.
8.5Geriatric Use
Patients 65 years and over, particularly those with hypertension, may be at increased risk for developing hypotension while undergoing anesthesia with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection.
In clinical studies of bupivacaine, elderly patients reached the maximal spread of analgesia and maximal motor blockade more rapidly than younger adult patients.
Differences in various pharmacokinetic parameters have been observed between elderly and younger adult patients [see Clinical Pharmacology (12.3)].
This product is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with impaired renal function. Because elderly patients are more likely to have decreased renal function, care should be taken in dose selection, and it may be useful to monitor renal function. Elderly patients may require lower doses of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection.
8.6Hepatic Impairment
Amide-type local anesthetics, such as bupivacaine, are metabolized by the liver. Patients with severe hepatic impairment, because of their inability to metabolize local anesthetics normally, are at a greater risk of developing toxic plasma concentrations, and potentially local anesthetic systemic toxicity. Therefore, consider reduced dosing and increased monitoring for local anesthetic systemic toxicity in patients with moderate to severe hepatic impairment treated with Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, especially with repeat doses [see Warnings and Precautions (5.10)] .
8.7Renal Impairment
Bupivacaine is known to be substantially excreted by the kidney, and the risk of adverse reactions to this drug may be greater in patients with renal impairment. This should be considered when selecting the Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection dosage [see Use in Specific Populations (8.5)] .
10overdosage
Clinical Presentation
Acute emergencies from use of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection are generally related to high plasma levels encountered during therapeutic use or to unintended intrathecal injection [see Warnings and Precautions (5.2, 5.9), Adverse Reactions (6)].
If not treated immediately, convulsions with simultaneous hypoxia, hypercarbia, and acidosis plus myocardial depression from the direct effects of bupivacaine may result in cardiac arrhythmias, bradycardia, asystole, ventricular fibrillation, or cardiac arrest. Respiratory abnormalities, including apnea, may occur. Hypoventilation or apnea due to unintentional intrathecal injection of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection may produce these same signs and also lead to cardiac arrest if ventilatory support is not instituted. If cardiac arrest should occur, successful outcome may require prolonged resuscitative efforts.
Management
The first step in the management of systemic toxic reactions, as well as hypoventilation or apnea due to unintentional intrathecal injection of Bupivacaine Hydrochloride Injection/Bupivacaine Hydrochloride and Epinephrine Injection, consists of immediate attention to the establishment and maintenance of a patent airway and effective assisted or controlled ventilation with 100% oxygen with a delivery system capable of permitting immediate positive airway pressure by mask. Endotracheal intubation, using drugs and techniques familiar to the clinician, may be indicated after initial administration of oxygen by mask if difficulty is encountered in the maintenance of a patent airway, or if prolonged ventilatory support (assisted or controlled) is indicated.
If necessary, use drugs to manage the convulsions. A bolus intravenous dose of a benzodiazepine will counteract CNS stimulation related to Bupivacaine Hydrochloride Injection. Immediately after the institution of ventilatory measures, evaluate the adequacy of the circulation. Supportive treatment of circulatory depression may require Advance Cardiac Life Support measures.
11description
Bupivacaine Hydrochloride Injection contains bupivacaine hydrochloride, an amide local anesthetic, as the active pharmaceutical ingredient. The route of administration for Bupivacaine Hydrochloride Injection (without epinephrine) is by injection, for infiltration, perineural, caudal, epidural, or retrobulbar use. Multiple-dose vials contain methylparaben [see Warnings and Precautions (5.4)] .
Bupivacaine hydrochloride is 2-piperidinecarboxamide, 1-butyl- N-(2,6-dimethylphenyl)-, monohydrochloride, monohydrate. It is a white crystalline powder that is freely soluble in 95 percent ethanol, soluble in water, and slightly soluble in chloroform or acetone. It has the following structural formula:
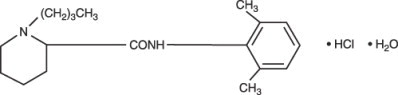
Bupivacaine Hydrochloride Injection, USP is a clear and colorless sterile isotonic solution. Each mL of single-dose vial contains 2.5 mg, 5 mg, or 7.5 mg of bupivacaine hydrochloride (equivalent to 2.22 mg, 4.44 mg, or 6.66 mg of bupivacaine, respectively), sodium chloride for isotonicity, sodium hydroxide or hydrochloric acid to adjust the pH between 4 and 6.5, in water for injection.
For the multiple-dose vials, each mL also contains 1 mg methylparaben as preservative.
12clinical Pharmacology
12.1Mechanism of Action
Bupivacaine blocks the generation and the conduction of nerve impulses, presumably by increasing the threshold for electrical excitation in the nerve, by slowing the propagation of the nerve impulse, and by reducing the rate of rise of the action potential. In general, the progression of anesthesia is related to the diameter, myelination, and conduction velocity of affected nerve fibers. Clinically, the order of loss of nerve function is as follows: (1) pain, (2) temperature, (3) touch, (4) proprioception, and (5) skeletal muscle tone.
Epinephrine is a vasoconstrictor added to bupivacaine to slow absorption into the general circulation and thus prolong maintenance of an active tissue concentration.
12.2Pharmacodynamics
Systemic absorption of bupivacaine produces effects on the cardiovascular system and CNS. At blood concentrations achieved with normal therapeutic doses, changes in cardiac conduction, excitability, refractoriness, contractility, and peripheral vascular resistance are minimal. However, toxic blood concentrations depress cardiac conduction and excitability, which may lead to atrioventricular block, ventricular arrhythmias, and cardiac arrest, sometimes resulting in fatalities. In addition, myocardial contractility is depressed and peripheral vasodilation occurs, leading to decreased cardiac output and arterial blood pressure. These cardiovascular changes are more likely to occur after unintended intravascular injection of bupivacaine [see Warnings and Precautions (5.9)] .
Following systemic absorption, bupivacaine can produce CNS stimulation, CNS depression, or both. Apparent central stimulation is manifested as restlessness, tremors, and shivering, progressing to convulsions, followed by CNS depression and coma progressing ultimately to respiratory arrest. However, bupivacaine has a primary depressant effect on the medulla and on higher centers. The depressed stage may occur without a prior excited state.
The duration of local anesthesia after administration of Bupivacaine Hydrochloride Injection is longer than that observed after administration of other commonly used short-acting local anesthetics. There appears to be period of analgesia that persists after the resolution of the block and return of sensation.
The onset of action following dental injections is usually 2 to 10 minutes and may last up to 7 hours. The duration of anesthetic effect is prolonged by the addition of epinephrine 1:200,000.
12.3Pharmacokinetics
Systemic plasma levels of bupivacaine following administration of Bupivacaine Hydrochloride Injection do not correlate with local efficacy.
Absorption
The rate of systemic absorption of bupivacaine is dependent upon the total dose and concentration of drug administered, the route of administration, the vascularity of the administration site, and the presence or absence of epinephrine in the anesthetic solution. A dilute concentration of epinephrine (1:200,000) usually reduces the rate of absorption and peak plasma concentration of bupivacaine, permitting the use of moderately larger total doses and sometimes prolonging the duration of action [see Dosage and Administration (2)] .
After injection of Bupivacaine Hydrochloride Injection for caudal, epidural, or peripheral nerve block, peak levels of bupivacaine in the blood are reached in 30 to 45 minutes, followed by a decline to insignificant levels during the next three to six hours.
Distribution
Bupivacaine appears to cross the placenta by passive diffusion. The rate and degree of diffusion is governed by (1) the degree of plasma protein binding, (2) the degree of ionization, and (3) the degree of lipid solubility. Fetal/maternal ratios of bupivacaine appear to be inversely related to the degree of plasma protein binding, because only the free, unbound drug is available for placental transfer. Bupivacaine with a high protein binding capacity (95%) has a low fetal/maternal ratio (0.2 to 0.4). The extent of placental transfer is also determined by the degree of ionization and lipid solubility of the drug. Lipid soluble, nonionized drugs readily enter the fetal blood from the maternal circulation.
Depending upon the route of administration, bupivacaine is distributed to some extent to all body tissues, with high concentrations found in highly perfused organs such as the liver, lungs, heart, and brain.
Pharmacokinetic studies on the plasma profile of bupivacaine after direct intravenous injection (Bupivacaine Hydrochloride Injection is not approved for intravenous use) suggest a three-compartment open model. The first compartment is represented by the rapid intravascular distribution of the drug. The second compartment represents the equilibration of the drug throughout the highly perfused organs such as the brain, myocardium, lungs, kidneys, and liver. The third compartment represents an equilibration of the drug with poorly perfused tissues, such as muscle and fat.
Elimination
The half-life of bupivacaine in adults is 2.7 hours.
Metabolism
Amide-type local anesthetics such as bupivacaine are metabolized primarily in the liver via conjugation with glucuronic acid. Pipecoloxylidine is the major metabolite of bupivacaine. The elimination of drug from tissue distribution depends largely upon the availability of binding sites in the circulation to carry it to the liver where it is metabolized.
Excretion
The kidney is the main excretory organ for most local anesthetics and their metabolites. Urinary excretion is affected by urinary perfusion and factors affecting urinary pH. Only 6% of bupivacaine is excreted unchanged in the urine.
Specific Populations
Geriatric Patients
Elderly patients exhibited higher peak plasma concentrations than younger patients following administration of Bupivacaine Hydrochloride Injection. The total plasma clearance was decreased in these patients [see Use in Specific Populations (8.5)] .
Patients with Hepatic Impairment
Various pharmacokinetic parameters of the local anesthetics can be significantly altered by the presence of hepatic disease. Patients with hepatic disease, especially those with severe hepatic disease, may be more susceptible to the potential toxicities of the amide-type local anesthetics [see Use in Specific Populations (8.6)] .
Patients with Renal Impairment
Various pharmacokinetic parameters of the local anesthetics can be significantly altered by the presence of renal disease, factors affecting urinary pH, and renal blood flow [see Use in Specific Populations (8.5, 8.7)] .
13nonclinical Toxicology
13.1Carcinogenesis, Mutagenesis, Impairment of Fertility
Carcinogenesis
Long-term studies in animals to evaluate the carcinogenic potential of bupivacaine hydrochloride have not been conducted.
Mutagenesis
The mutagenic potential of bupivacaine hydrochloride has not been determined.
Impairment of Fertility
The effect of bupivacaine on fertility has not been determined.
16how Supplied/storage And Handling
STORAGE AND HANDLING SECTION
Store at 20 °C to 25 °C (68 °F to 77 °F); excursions permitted between 15 °C to 30 °C (59 °F to 86 °F). [See USP Controlled Room Temperature.]
Bupivacaine Hydrochloride Injection, USP ─ Solutions of bupivacaine hydrochloride that do not contain epinephrine may be autoclaved. Autoclave at 15-pound pressure, 121 °C (250 °F) for 15 minutes. This product is clear and colorless. Do not use the solution if it is discolored or if it contains a precipitate.
Unit of Sale Concentration NDC 0409-1159-01 Tray of 25 single-dose teartop vials 0.25% 25 mg/10 mL (2.5 mg/mL) NDC 0409-1159-02 Tray of 25 single-dose teartop vials 0.25% 75 mg/30 mL (2.5 mg/mL) NDC 0409-1160-01 Tray of 25 multiple-dose fliptop vials 0.25% 125 mg/50 mL (2.5 mg/mL) NDC 0409-1163-01 Tray of 25 multiple-dose fliptop vials 0.5% 250 mg/50 mL (5 mg/mL) NDC 0409-1162-01 Tray of 25 single-dose teartop vials 0.5% 50 mg/10 mL (5 mg/mL) NDC 0409-1162-02 Tray of 25 single-dose teartop vials 0.5% 150 mg/30 mL (5 mg/mL) NDC 0409-1165-01 Tray of 25 single-dose teartop vials 0.75% 75 mg/10 mL (7.5 mg/mL) NDC 0409-1165-02 Tray of 25 single-dose teartop vials 0.75% 225 mg/30 mL (7.5 mg/mL)
For single-dose vials: Discard unused portion.
17patient Counseling Information
Allergic-Type Reactions
Assess if the patient has had allergic-type reactions to amide-type local anesthetics or to other formulation ingredients, such as the antimicrobial preservative methylparaben contained in multiple-dose vials or sulfites in epinephrine-containing solutions [see Contraindications (4), Warnings and Precautions (5.8), Adverse Reactions (6)].
Temporary Loss of Sensation and Motor Activity After Caudal or Epidural Anesthesia
When appropriate, patients should be informed in advance that they may experience temporary loss of sensation and motor activity, usually in the lower half of the body, following proper administration of caudal or epidural anesthesia.
Instructions After Dental Injection of Bupivacaine Hydrochloride Injection
Advise patients receiving dental injections of Bupivacaine Hydrochloride Injection not to chew solid foods or to test the anesthetized area by biting or probing until anesthesia has worn off (up to 7 hours) [see Warnings and Precautions (5.16)].
Methemoglobinemia
Inform patients that use of local anesthetics may cause methemoglobinemia, a serious condition that must be treated promptly. Advise patients or caregivers to seek immediate medical attention if they or someone in their care experience the following signs or symptoms: pale, gray, or blue colored skin (cyanosis); headache; rapid heart rate; shortness of breath; lightheadedness; or fatigue [see Warnings and Precautions (5.3)].
This product's labeling may have been updated. For the most recent prescribing information, please visit www.pfizer.com.
Distributed by Hospira, Inc., Lake Forest, IL 60045 USA
LAB-1176-5.0
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension, USP, 6 mg/mL
30 mg/5 mL (6 mg/mL)
Description
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is a sterile aqueous suspension containing 3 mg per milliliter betamethasone, as betamethasone sodium phosphate, and 3 mg per milliliter betamethasone acetate. Inactive ingredients per mL: 7.1 mg dibasic sodium phosphate anhydrous; 3.4 mg monobasic sodium phosphate monohydrate; 0.1 mg edetate disodium; and 0.2 mg benzalkonium chloride as a preservative. The pH is adjusted to between 6.8 and 7.2.
The formula for betamethasone sodium phosphate is C 22H 28FNa 2O 8P and it has a molecular weight of 516.40. Chemically, it is 9-Fluoro-11β,17,21-trihydroxy-16β-methylpregna-1,4-diene-3,20-dione 21-(disodium phosphate).
The formula for betamethasone acetate is C 24H 31FO 6 and it has a molecular weight of 434.50. Chemically, it is 9-Fluoro-11β,17,21-trihydroxy-16β-methylpregna-1,4-diene-3,20-dione 21-acetate.
The chemical structures for betamethasone sodium phosphate and betamethasone acetate are as follows:
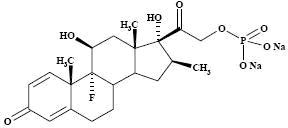
Structural Formula
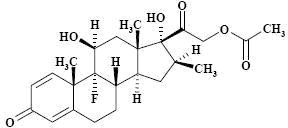
Structural Formula
Betamethasone sodium phosphate is a white to practically white, odorless powder, and is hygroscopic. It is freely soluble in water and in methanol, but is practically insoluble in acetone and in chloroform.
Betamethasone acetate is a white to creamy white, odorless powder that sinters and resolidifies at about 165ÂşC, and remelts at about 200ÂşC to 220ÂşC with decomposition. It is practically insoluble in water, but freely soluble in acetone, and is soluble in alcohol and in chloroform.
Clinical Pharmacology
Glucocorticoids, naturally occurring and synthetic, are adrenocortical steroids that are readily absorbed from the gastrointestinal tract.
Naturally occurring glucocorticoids (hydrocortisone and cortisone), which also have salt-retaining properties, are used as replacement therapy in adrenocortical deficiency states. Their synthetic analogs are primarily used for their anti-inflammatory effects in disorders of many organ systems. A derivative of prednisolone, betamethasone has a 16β-methyl group that enhances the anti-inflammatory action of the molecule and reduces the sodium- and water-retaining properties of the fluorine atom bound at carbon 9.
Betamethasone sodium phosphate, a soluble ester, provides prompt activity, while betamethasone acetate is only slightly soluble and affords sustained activity.
Indications And Usage
When oral therapy is not feasible, the intramuscular use of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is indicated as follows:
Allergic States Control of severe or incapacitating allergic conditions intractable to adequate trials of conventional treatment in asthma, atopic dermatitis, contact dermatitis, drug hypersensitivity reactions, perennial or seasonal allergic rhinitis, serum sickness, transfusion reactions.
Dermatologic Diseases Bullous dermatitis herpetiformis, exfoliative erythroderma, mycosis fungoides, pemphigus, severe erythema multiforme (Stevens-Johnson syndrome).
Endocrine Disorders Congenital adrenal hyperplasia, hypercalcemia associated with cancer, nonsuppurative thyroiditis.
Hydrocortisone or cortisone is the drug of choice in primary or secondary adrenocortical insufficiency. Synthetic analogs may be used in conjunction with mineralocorticoids where applicable; in infancy mineralocorticoid supplementation is of particular importance.
Gastrointestinal Diseases To tide the patient over a critical period of the disease in regional enteritis and ulcerative colitis.
Hematologic Disorders Acquired (autoimmune) hemolytic anemia, Diamond-Blackfan anemia, pure red cell aplasia, selected cases of secondary thrombocytopenia.
Miscellaneous Trichinosis with neurologic or myocardial involvement, tuberculous meningitis with subarachnoid block or impending block when used with appropriate antituberculous chemotherapy.
Neoplastic Diseases For palliative management of leukemias and lymphomas.
Nervous System Acute exacerbations of multiple sclerosis; cerebral edema associated with primary or metastatic brain tumor or craniotomy.
Ophthalmic Diseases Sympathetic ophthalmia, temporal arteritis, uveitis and ocular inflammatory conditions unresponsive to topical corticosteroids.
Renal Diseases To induce diuresis or remission of proteinuria in idiopathic nephrotic syndrome or that due to lupus erythematosus.
Respiratory Diseases Berylliosis, fulminating or disseminated pulmonary tuberculosis when used concurrently with appropriate antituberculous chemotherapy, idiopathic eosinophilic pneumonias, symptomatic sarcoidosis.
Rheumatic Disorders As adjunctive therapy for short-term administration (to tide the patient over an acute episode or exacerbation) in acute gouty arthritis; acute rheumatic carditis; ankylosing spondylitis; psoriatic arthritis; rheumatoid arthritis, including juvenile rheumatoid arthritis (selected cases may require low-dose maintenance therapy). For the treatment of dermatomyositis, polymyositis, and systemic lupus erythematosus.
The intra-articular or soft tissue administration of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is indicated as adjunctive therapy for short-term administration (to tide the patient over an acute episode or exacerbation) in acute gouty arthritis, acute and subacute bursitis, acute nonspecific tenosynovitis, epicondylitis, rheumatoid arthritis, synovitis of osteoarthritis.
The intralesional administration of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is indicated for alopecia areata; discoid lupus erythematosus; keloids; localized hypertrophic, infiltrated, inflammatory lesions of granuloma annulare, lichen planus, lichen simplex chronicus (neurodermatitis), and psoriatic plaques; necrobiosis lipoidica diabeticorum.
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension may also be useful in cystic tumors of an aponeurosis or tendon (ganglia).
Contraindications
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is contraindicated in patients who are hypersensitive to any components of this product (see DESCRIPTION ). Intramuscular corticosteroid preparations are contraindicated for idiopathic thrombocytopenic purpura.
Warnings
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension should not be administered intravenously.
Serious Neurologic Adverse Reactions with Epidural Administration
Serious neurologic events, some resulting in death, have been reported with epidural injection of corticosteroids. Specific events reported include, but are not limited to, spinal cord infarction, paraplegia, quadriplegia, cortical blindness, and stroke. These serious neurologic events have been reported with and without use of fluoroscopy. The safety and effectiveness of epidural administration of corticosteroids have not been established, and corticosteroids are not approved for this use.
General
Rare instances of anaphylactoid/anaphylactic reactions with a possibility of shock have occurred in patients receiving parenteral corticosteroid therapy (see ADVERSE REACTIONS). Use caution in patients who have a history of allergic reaction to corticosteroids.
In patients on corticosteroid therapy subjected to any unusual stress, hydrocortisone or cortisone is the drug of choice as a supplement during and after the event.
Cardio-Renal
Average and large doses of corticosteroids can cause elevation of blood pressure, salt and water retention, and increased excretion of potassium. These effects are less likely to occur with the synthetic derivatives except when used in large doses. Dietary salt restriction and potassium supplementation may be necessary. All corticosteroids increase calcium excretion.
Literature reports suggest an apparent association between use of corticosteroids and left ventricular free wall rupture after a recent myocardial infarction; therefore, therapy with corticosteroids should be used with great caution in these patients.
Endocrine
Corticosteroids can produce reversible hypothalamic pituitary adrenal (HPA) axis suppression with the potential for glucocorticosteroid insufficiency after withdrawal of treatment.
Metabolic clearance of corticosteroids is decreased in hypothyroid patients and increased in hyperthyroid patients. Changes in thyroid status of the patient may necessitate adjustment in dosage.
Infections
Patients who are on corticosteroids are more susceptible to infections than are healthy individuals. There may be decreased resistance and inability to localize infection when corticosteroids are used. Infection with any pathogen (viral, bacterial, fungal, protozoan, or helminthic) in any location of the body may be associated with the use of corticosteroids alone or in combination with other immunosuppressive agents. These infections may be mild to severe. With increasing doses of corticosteroids, the rate of occurrence of infectious complications increases. Corticosteroids may also mask some signs of current infection.
​​​Corticosteroids may exacerbate systemic fungal infections and therefore should not be used in the presence of such infections unless they are needed to control drug reactions. There have been cases reported in which concomitant use of amphotericin B and hydrocortisone was followed by cardiac enlargement and congestive heart failure (see PRECAUTIONS, Drug Interactions, Amphotericin B Injection and Potassium-Depleting Agents section).
Latent disease may be activated or there may be an exacerbation of intercurrent infections due to pathogens, including those caused by Amoeba, Candida, Cryptococcus, Mycobacterium, Nocardia, Pneumocystis, and Toxoplasma. It is recommended that latent amebiasis or active amebiasis be ruled out before initiating corticosteroid therapy in any patient who has spent time in the tropics or in any patient with unexplained diarrhea.
Similarly, corticosteroids should be used with great care in patients with known or suspected Strongyloides (threadworm) infestation. In such patients, corticosteroid-induced immunosuppression may lead to Strongyloides hyperinfection and dissemination with widespread larval migration, often accompanied by severe enterocolitis and potentially fatal gram-negative septicemia.
Corticosteroids should not be used in cerebral malaria.
​The use of corticosteroids in active tuberculosis should be restricted to those cases of fulminating or disseminated tuberculosis in which the corticosteroid is used for the management of the disease in conjunction with an appropriate antituberculous regimen.
If corticosteroids are indicated in patients with latent tuberculosis or tuberculin reactivity, close observation is necessary as reactivation of the disease may occur. During prolonged corticosteroid therapy, these patients should receive chemoprophylaxis.
Administration of live or live, attenuated vaccines is contraindicated in patients receiving immunosuppressive doses of corticosteroids. Killed or inactivated vaccines may be administered. However, the response to such vaccines cannot be predicted. Immunization procedures may be undertaken in patients who are receiving corticosteroids as replacement therapy, e.g., for Addison’s disease.
Chickenpox and measles can have a more serious or even fatal course in pediatric and adult patients on corticosteroids. In pediatric and adult patients who have not had these diseases, particular care should be taken to avoid exposure. The contribution of the underlying disease and/or prior corticosteroid treatment to the risk is also not known. If exposed to chickenpox, prophylaxis with varicella zoster immune globulin (VZIG) may be indicated. If exposed to measles, prophylaxis with immunoglobulin (IG) may be indicated. (See the respective package inserts for complete VZIG and IG prescribing information.) If chickenpox develops, treatment with antiviral agents should be considered.
Neurologic
Reports of severe medical events have been associated with the intrathecal route of administration (see ADVERSE REACTIONS, Gastrointestinal and Neurologic/Psychiatric sections ).
Results from one multicenter, randomized, placebo-controlled study with methylprednisolone hemisuccinate, an intravenous corticosteroid, showed an increase in early mortality (at 2 weeks) and late mortality (at 6 months) in patients with cranial trauma who were determined not to have other clear indications for corticosteroid treatment. High doses of corticosteroids, including Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension, should not be used for the treatment of traumatic brain injury.
Ophthalmic
Use of corticosteroids may produce posterior subcapsular cataracts, increased intraocular pressure, glaucoma with possible damage to the optic nerves, and may enhance the establishment of secondary ocular infections due to bacteria, fungi, or viruses. Consider referral to an ophthalmologist for patients who develop ocular symptoms or use corticosteroid-containing products for more than 6 weeks. The use of oral corticosteroids is not recommended in the treatment of optic neuritis and may lead to an increase in the risk of new episodes. Corticosteroids should not be used in active ocular herpes simplex.
Precautions
General
This product, like many other steroid formulations, is sensitive to heat. Therefore, it should not be autoclaved when it is desirable to sterilize the exterior of the vial.
The lowest possible dose of corticosteroid should be used to control the condition under treatment. When reduction in dosage is possible, the reduction should be gradual.
Since complications of treatment with glucocorticoids are dependent on the size of the dose and the duration of treatment, a risk/benefit decision must be made in each individual case as to dose and duration of treatment and as to whether daily or intermittent therapy should be used.
Kaposi’s sarcoma has been reported to occur in patients receiving corticosteroid therapy, most often for chronic conditions. Discontinuation of corticosteroids may result in clinical improvement.
Cardio-Renal
As sodium retention with resultant edema and potassium loss may occur in patients receiving corticosteroids, these agents should be used with caution in patients with congestive heart failure, hypertension, or renal insufficiency.
Endocrine
Drug-induced secondary adrenocortical insufficiency may be minimized by gradual reduction of dosage. This type of relative insufficiency may persist for months after discontinuation of therapy. Therefore, in any situation of stress occurring during that period, naturally occurring glucocorticoids (hydrocortisone cortisone), which also have salt-retaining properties, rather than betamethasone, are the appropriate choices as replacement therapy in adrenocortical deficiency states.
Gastrointestinal
Steroids should be used with caution in active or latent peptic ulcers, diverticulitis, fresh intestinal anastomoses, and nonspecific ulcerative colitis, since they may increase the risk of a perforation.
Signs of peritoneal irritation following gastrointestinal perforation in patients receiving corticosteroids may be minimal or absent.
There is an enhanced effect of corticosteroids in patients with cirrhosis.
Intra-Articular and Soft Tissue Administration
Intra-articular injected corticosteroids may be systemically absorbed.
Appropriate examination of any joint fluid present is necessary to exclude a septic process.
A marked increase in pain accompanied by local swelling, further restriction of joint motion, fever, and malaise are suggestive of septic arthritis. If this complication occurs and the diagnosis of sepsis is confirmed, appropriate antimicrobial therapy should be instituted.
Injection of a steroid into an infected site is to be avoided. Local injection of a steroid into a previously injected joint is not usually recommended.
Corticosteroid injection into unstable joints is generally not recommended.
Intra-articular injection may result in damage to joint tissues (see ADVERSE REACTIONS, Musculoskeletal section ).
Musculoskeletal
Corticosteroids decrease bone formation and increase bone resorption both through their effect on calcium regulation (i.e., decreasing absorption and increasing excretion) and inhibition of osteoblast function. This, together with a decrease in the protein matrix of the bone secondary to an increase in protein catabolism, and reduced sex hormone production, may lead to inhibition of bone growth in pediatric patients and the development of osteoporosis at any age. Special consideration should be given to patients at increased risk of osteoporosis (i.e., postmenopausal women) before initiating corticosteroid therapy.
Neuro-Psychiatric
Although controlled clinical trials have shown corticosteroids to be effective in speeding the resolution of acute exacerbations of multiple sclerosis, they do not show that they affect the ultimate outcome or natural history of the disease. The studies do show that relatively high doses of corticosteroids are necessary to demonstrate a significant effect (see DOSAGE AND ADMINISTRATION).
An acute myopathy has been observed with the use of high doses of corticosteroids, most often occurring in patients with disorders with neuromuscular transmission (e.g., myasthenia gravis), or in patients receiving concomitant therapy of neuromuscular blocking drugs (eg, pancuronium). This acute myopathy is generalized, may involve ocular and respiratory muscles, and may result in quadriparesis. Elevation of creatinine kinase may occur. Clinical improvement or recovery after stopping corticosteroids may require weeks to years.
Psychic derangements may appear when corticosteroids are used, ranging from euphoria, insomnia, mood swings, personality changes, and severe depression to frank psychotic manifestations. Also, existing emotional instability or psychotic tendencies may be aggravated by corticosteroids.
Information for Patients
Patients should be warned not to discontinue the use of corticosteroids abruptly or without medical supervision, to advise any medical attendants that they are taking corticosteroids and to seek medical advice at once should they develop fever or other signs of infection.
Persons who are on corticosteroids should be warned to avoid exposure to chickenpox or measles. Patients should also be advised that if they are exposed, medical advice should be sought without delay.
Drug Interactions
Aminoglutethimide may lead to a loss of corticosteroid-induced adrenal suppression.
When corticosteroids are administered concomitantly with potassium-depleting agents (ie, amphotericin B, diuretics), patients should be observed closely for development of hypokalemia. There have been cases reported in which concomitant use of amphotericin B and hydrocortisone was followed by cardiac enlargement and congestive heart failure.
​Macrolide antibiotics have been reported to cause a significant decrease in corticosteroid clearance.
Concomitant use of anticholinesterase agents and corticosteroids may produce severe weakness in patients with myasthenia gravis. If possible, anticholinesterase agents should be withdrawn at least 24 hours before initiating corticosteroid therapy.
Coadministration of corticosteroids and warfarin usually results in inhibition of response to warfarin, although there have been some conflicting reports. Therefore, coagulation indices should be monitored frequently to maintain the desired anticoagulant effect.
Because corticosteroids may increase blood glucose concentrations, dosage adjustments of antidiabetic agents may be required.
Serum concentrations of isoniazid may be decreased.
Cholestyramine may increase the clearance of corticosteroids.
Increased activity of both cyclosporine and corticosteroids may occur when the two are used concurrently. Convulsions have been reported with this concurrent use.
Patients on digitalis glycosides may be at increased risk of arrhythmias due to hypokalemia.
Estrogens may decrease the hepatic metabolism of certain corticosteroids, thereby increasing their effect.
Drugs which induce hepatic microsomal drug-metabolizing enzyme activity may enhance the metabolism of corticosteroids and require that the dosage of the corticosteroid be increased.
Corticosteroids (including betamethasone) are metabolized by CYP3A4.
Ketoconazole has been reported to decrease the metabolism of certain corticosteroids by up to 60%, leading to an increased risk of corticosteroid side effects.
Coadministration with other strong CYP3A4 inhibitors (e.g., itraconazole, clarithromycin, ritonavir, cobicistat-containing products) may lead to increased exposures of corticosteroids and therefore the potential for increased risk of systemic corticosteroid side effects.
Consider the benefit of coadministration versus the potential risk of systemic corticosteroid effects, in which case patients should be monitored for systemic corticosteroid side effects.
Concomitant use of aspirin (or other nonsteroidal anti-inflammatory agents) and corticosteroids increases the risk of gastrointestinal side effects. Aspirin should be used cautiously in conjunction with corticosteroids in hypoprothrombinemia. The clearance of salicylates may be increased with concurrent use of corticosteroids.
Corticosteroids may suppress reactions to skin tests.
Patients on prolonged corticosteroid therapy may exhibit a diminished response to toxoids and live or inactivated vaccines due to inhibition of antibody response. Corticosteroids may also potentiate the replication of some organisms contained in live attenuated vaccines. Route administration of vaccines or toxoids should be deferred until corticosteroid therapy is discontinued if possible (see WARNINGS, Infections, Vaccination section).
Carcinogenesis, Mutagenesis, Impairment of Fertility
No adequate studies have been conducted in animals to determine whether corticosteroids have a potential for carcinogenesis or mutagenesis.
Steroids may increase or decrease motility and number of spermatozoa in some patients.
Pregnancy
Corticosteroids have been shown to be teratogenic in many species when given in doses equivalent to the human dose. Animal studies in which corticosteroids have been given to pregnant mice, rats, and rabbits have yielded an increased incidence of cleft palate in the offspring. There are no adequate and well-controlled studies in pregnant women. Corticosteroids should be used during pregnancy only if the potential benefit justifies the potential risk to the fetus. Infants born to mothers who have received corticosteroids during pregnancy should be carefully observed for signs of hypoadrenalism.
Nursing Mothers
Systemically administered corticosteroids appear in human milk and could suppress growth, interfere with endogenous corticosteroid production, or cause other untoward effects. Caution should be exercised when corticosteroids are administered to a nursing woman.
Pediatric Use
The efficacy and safety of corticosteroids in the pediatric population are based on the well-established course of effect of corticosteroids, which is similar in pediatric and adult populations. Published studies provide evidence of efficacy and safety in pediatric patients for the treatment of nephrotic syndrome (> 2 years of age), and aggressive lymphomas and leukemias (> 1 month of age). Other indications for pediatric use of corticosteroids, e.g., severe asthma and wheezing, are based on adequate and well-controlled trials conducted in adults, on the premises that the course of the diseases and their pathophysiology are considered to be substantially similar in both populations.
The adverse effects of corticosteroids in pediatric patients are similar to those in adults (see ADVERSE REACTIONS). Like adults, pediatric patients should be carefully observed with frequent measurements of blood pressure, weight, height, intraocular pressure, and clinical evaluation for the presence of infection, psychosocial disturbances, thromboembolism, peptic ulcers, cataracts, and osteoporosis. Pediatric patients who are treated with corticosteroids by any route, including systemically administered corticosteroids, may experience a decrease in their growth velocity. This negative impact of corticosteroids on growth has been observed at low systemic doses and in the absence of laboratory evidence of HPA axis suppression (i.e., cosyntropin stimulation and basal cortisol plasma levels). Growth velocity may therefore be a more sensitive indicator of systemic corticosteroid exposure in pediatric patients than some commonly used tests of HPA axis function. The linear growth of pediatric patients treated with corticosteroids should be monitored, and the potential growth effects of prolonged treatment should be weighed against clinical benefits obtained and the availability of treatment alternatives. In order to minimize the potential growth effects of corticosteroids, pediatric patients should be titrated to the lowest effective dose.
Geriatric Use
No overall differences in safety or effectiveness were observed between elderly subjects and younger subjects, and other reported clinical experience has not identified differences in responses between the elderly and young patients, but greater sensitivity of some older individuals cannot be ruled out.
Adverse Reactions
(uled alphabetically, under each subsection)
Allergic Reactions
Anaphylactoid reaction, anaphylaxis, angioedema.
Cardiovascular
Bradycardia, cardiac arrest, cardiac arrhythmias, cardiac enlargement, circulatory collapse, congestive heart failure, fat embolism, hypertension, hypertrophic cardiomyopathy in premature infants, myocardial rupture following recent myocardial infarction (see WARNINGS), pulmonary edema, syncope, tachycardia, thromboembolism, thrombophlebitis, vasculitis.
Dermatologic
Acne, allergic dermatitis, cutaneous and subcutaneous atrophy, dry scaly skin, ecchymoses and petechiae, edema, erythema, hyperpigmentation, hypopigmentation, impaired wound healing, increased sweating, rash, sterile abscess, striae, suppressed reactions to skin tests, thin fragile skin, thinning scalp hair, urticaria.
Endocrine
Decreased carbohydrate and glucose tolerance, development of cushingoid state, glucosuria, hirsutism, hypertrichosis, increased requirements for insulin or oral hypoglycemic adrenocortical and pituitary unresponsiveness (particularly in times of stress, as in trauma, surgery, or illness), suppression of growth in pediatric patients.
Fluid and Electrolyte Disturbances
Congestive heart failure in susceptible patients, fluid retention, hypokalemic alkalosis, potassium loss, sodium retention.
Gastrointestinal
Abdominal distention, bowel/bladder dysfunction (after intrathecal administration), elevation in serum liver enzyme levels (usually reversible upon discontinuation), hepatomegaly, increased appetite, nausea, pancreatitis, peptic ulcer with possible perforation and hemorrhage, perforation of the small and large intestine (particularly in patients with inflammatory bowel disease), ulcerative esophagitis.
Metabolic
Negative nitrogen balance due to protein catabolism.
Musculoskeletal
Aseptic necrosis of femoral and humeral heads, calcinosis (following intra-articular or intralesional use), Charcot-like arthropathy, loss of muscle mass, muscle weakness, osteoporosis, pathologic fracture of long bones, postinjection flare (following intra-articular use), steroid myopathy, tendon rupture, vertebral compression fractures.
Neurologic/Psychiatric
Convulsions, depression, emotional instability, euphoria, headache, increased intracranial pressure with papilledema (pseudotumor cerebri) usually following discontinuation of treatment, insomnia, mood swings, neuritis, neuropathy, paresthesia, personality changes, psychic disorders, vertigo. Arachnoiditis, meningitis, paraparesis/paraplegia, and sensory disturbances have occurred after intrathecal administration (see WARNINGS, Neurologic section).
Ophthalmic
Exophthalmos, glaucoma, increased intraocular pressure, posterior subcapsular cataracts, rare instances of blindness associated with periocular injections, vision blurred.
Other
Abnormal fat deposits, decreased resistance to infection, hiccups, increased or decreased motility and number of spermatozoa, malaise, moon face, weight gain.
Overdosage
Treatment of acute overdose is by supportive and symptomatic therapy. For chronic overdosage in the face of severe disease requiring continuous steroid therapy, the dosage of the corticosteroid may be reduced only temporarily, or alternate day treatment may be introduced.
Dosage And Administration
Benzyl alcohol as a preservative has been associated with a fatal “Gasping Syndrome” in premature infants and infants of low birth weight. Solutions used for further dilution of this product should be preservative-free when used in the neonate, especially the premature infant. The initial dosage of parenterally administered Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension may vary from 0.25 to 9 mg per day depending on the specific disease entity being treated. However, in certain overwhelming, acute, life-threatening situations, administrations in dosages exceeding the usual dosages may be justified and may be in multiples of the oral dosages.
It Should Be Emphasized That Dosage Requirements Are Variable and Must Be Individualized on the Basis of the Disease Under Treatment and the Response of the Patient. After a favorable response is noted, the proper maintenance dosage should be determined by decreasing the initial drug dosage in small decrements at appropriate time intervals until the lowest dosage which will maintain an adequate clinical response is reached. Situations which may make dosage adjustments necessary are changes in clinical status secondary to remissions or exacerbations in the disease process, the patient’s individual drug responsiveness, and the effect of patient exposure to stressful situations not directly related to the disease entity under treatment. In this latter situation it may be necessary to increase the dosage of the corticosteroid for a period of time consistent with the patient’s condition. If after long-term therapy the drug is to be stopped, it is recommended that it be withdrawn gradually rather than abruptly.
In the treatment of acute exacerbations of multiple sclerosis, daily doses of 30 mg of betamethasone for a week followed by 12 mg every other day for 1 month are recommended (see PRECAUTIONS, Neuro-psychiatric section).
In pediatric patients, the initial dose of betamethasone may vary depending on the specific disease entity being treated. The range of initial doses is 0.02 to 0.3 mg/kg/day in three or four divided doses (0.6 to 9 mg/m 2bsa/day).
For the purpose of comparison, the following is the equivalent milligram dosage of the various glucocorticoids: Cortisone, 25 Triamcinolone, 4 Hydrocortisone, 20 Paramethasone, 2 Prednisolone, 5 Betamethasone, 0.75 Prednisone, 5 Dexamethasone, 0.75 Methylprednisolone, 4
These dose relationships apply only to oral or intravenous administration of these compounds. When these substances or their derivatives are injected intramuscularly or into joint spaces, their relative properties may be greatly altered.
If coadministration of a local anesthetic is desired, Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension may be mixed with 1% or 2% lidocaine hydrochloride, using the formulations which do not contain parabens. Similar local anesthetics may also be used. Diluents containing methylparaben, propylparaben, phenol, etc., should be avoided, since these compounds may cause flocculation of the steroid. The required dose of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is first withdrawn from the vial into the syringe. The local anesthetic is then drawn in, and the syringe shaken briefly. Do not inject local anesthetics into the vial of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension.
Bursitis, Tenosynovitis, Peritendinitis
In acute subdeltoid, subacromial, olecranon, and prepatellar bursitis, one intrabursal injection of 1 mL Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension can relieve pain and restore full range of movement. Several intrabursal injections of corticosteroids are usually required in recurrent acute bursitis and in acute exacerbations of chronic bursitis. Partial relief of pain and some increase in mobility can be expected in both conditions after one or two injections. Chronic bursitis may be treated with reduced dosage once the acute condition is controlled. In tenosynovitis and tendinitis, three or four local injections at intervals of 1 to 2 weeks between injections are given in most cases. Injections should be made into the affected tendon sheaths rather than into the tendons themselves. In ganglions of joint capsules and tendon sheaths, injection of 0.5 mL directly into the ganglion cysts has produced marked reduction in the size of the lesions.
Rheumatoid Arthritis and Osteoarthritis
Following intra-articular administration of 0.5 to 2 mL of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension, relief of pain, soreness, and stiffness may be experienced. Duration of relief varies widely in both diseases. Intra-articular Injection of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is well tolerated in joints and periarticular tissues. There is virtually no pain on injection, and the “secondary flare” that sometimes occurs a few hours after intra-articular injection of corticosteroids has not been reported with Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension. Using sterile technique, a 20- to 24-gauge needle on an empty syringe is inserted into the synovial cavity and a few drops of synovial fluid are withdrawn to confirm that the needle is in the joint. The aspirating syringe is replaced by a syringe containing Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension and injection is then made into the joint.
Recommended Doses for Intra-articular Injection Size of Joint Location Dose (mL) Very Large Hip 1 - 2 Large Knee, ankle, shoulder 1 Medium Elbow, wrist 0.5 - 1 Small (metacarpophalangeal, interphalangeal) (sternoclavicular) Hand, chest 0.25 to 0.5
A portion of the administered dose of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is absorbed systemically following intra-articular injection. In patients being treated concomitantly with oral or parenteral corticosteroids, especially those receiving large doses, the systemic absorption of the drug should be considered in determining intra-articular dosage.
Dermatologic Conditions
In intralesional treatment, 0.2 mL/cm 2 of Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension is injected intradermally (not subcutaneously) using a tuberculin syringe with a 25-gauge, 1/2-inch needle. Care should be taken to deposit a uniform depot of medication intradermally. A total of no more than 1 mL at weekly intervals is recommended.
Disorders of the Foot
A tuberculin syringe with a 25-gauge, 3/4-inch needle is suitable for most injections into the foot. The following doses are recommended at intervals of 3 days to a week.
Diagnosis Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension Dose (mL)
Bursitis under heloma durum or heloma molle
0.25 to 0.5 under calcaneal spur 0.5 over hallux rigidus or digiti quinti varus 0.5 Tenosynovitis, periostitis of cuboid 0.5 Acute gouty arthritis 0.5 to 1
How Supplied
NDC 0517-0720-01:
Betamethasone Sodium Phosphate and Betamethasone Acetate Injectable Suspension, 5 mL multiple dose vial; box of one. Inactive ingredients per mL: 7.1 mg dibasic sodium phosphate anhydrous; 3.4 mg monobasic sodium phosphate monohydrate; 0.1 mg edetate disodium; and 0.2 mg benzalkonium chloride as preservative.
SHAKE WELL BEFORE USING.
Store at 20° to 25°C (68° to 77°F); excursions permitted to 15° to 30°C (59° to 86°F) [See USP Controlled Room Temperature]. Protect from light.
Rx only
AMERICAN REGENT, INC. SHIRLEY, NY 11967
Revised July 2018
Povidone-iodine Swabsticks
Otc - Active Ingredient Section
Active Ingredient                                        Purpose
Povidone Iodine 10% w/v (9.85% w/w)Â Â Â Â Â Â Antiseptic
Purpose:
Purpose:
- First aid antiseptic to help prevent skin infection in minor cuts, scrapes and burns.
- For preparation of the skin prior to surgery.
- Helps reduce bacteria that can potentially cause skin infections.
Warnings:
- FOR EXTERNAL USE ONLY
Do Not Use:
- As a first aid antiseptic for more than 1 week.
- In the eyes.
- Over large areas of the body.
Ask A Doctor Before Use If You Have:
- Deep puncture wounds
- Animal bites
- Serious burns
Stop Use:
- If irritation and redness develop
- If condition persists for more than 72 hours, consult a physician.
Keep Out Of Reach Of Children
Keep out of reach of children.If swallowed, get medical help or contact a Poison Control Center.
Directions Povidone Iodine:
Tear at notch, remove applicator, use only once.
As a first aid antiseptic
- clean affected area
- apply 1 to 3 times daily
- may be covered with a sterile bandage, if bandaged let dry.
For preoperative patient skin preparation
- clean area
- apply to operative site prior to surgery using the applicator
Other Information:
Store at room temperature.
Avoid excessive heat
Indications & Usage Section
For use as an
- first aid antiseptic
- pre-operative skin preperation
Inactive Ingredients
Inactive ingredients: Citric acid, glycerin, polysorbate 80, sodium citrate USP, sodium phosphate dibasic, water
Isopropyl Alcohol 70% Prep Pads
Active Ingredient
Isopropyl Alcohol 70% v/v
Purpose
Antiseptic
Uses
For first aid to decrease germs in
- minor cuts
- scrapes
- burns
For preparation of the skin prior to injection
Warnings
For external use only
Flammable - keep away from fire or flame
Do not use
with electrocautery procedures
When using this product do not
- get into eyes
- apply over large areas of the body
- in case of deep or puncture wounds, animal bites or serious burns consult a doctor
Stop use and ask a doctor if
- condition persists or gets worse or lasts for more than 72 hours
- do not use longer than 1 week unless directed by a doctor
Keep out of reach of children.
If swallowed, get medical help or contact a Poison Control Center right away.
Directions
- apply to skin as needed
- discard after single use
Other Information
Protect from freezing and avoid excessive heat
Inactive Ingredient
Water
Package Label.principal Display Panel
PRINCIPAL DISPLAY PANEL
NDC: 76420-785-01
Rx Only
Marbeta-25™
Kit Contains
1 Bupivacaine HCl 0.25% Single Dose Vial (10mL)
1 Betamethasone Sodium Phosphate and Betamethasone Acetate 6mg/mL (5mL)
1 Povidone-Iodine Swabsticks (3 Swabs)
3 Isopropyl Alcohol 70% Prep Pads
1 Pair Nitrile Powder Free Sterile Gloves (M)
1 Drape
1 Adhesive Bandage
5 Non Sterile 4x4 Gauze
Needles and Syringes Not Included
1 Dose
Single Use Only
Distributed by:
Enovachem™
PHARMACEUTICALS
Torrance, CA 90501

DISCLAIMER:
"This tool does not provide medical advice, and is for informational and educational purposes only, and is not a substitute for professional medical advice, treatment or diagnosis. Call your doctor to receive medical advice. If you think you may have a medical emergency, please dial 911."
"Do not rely on openFDA to make decisions regarding medical care. While we make every effort to ensure that data is accurate, you should assume all results are unvalidated. We may limit or otherwise restrict your access to the API in line with our Terms of Service."
"This product uses publicly available data from the U.S. National Library of Medicine (NLM), National Institutes of Health, Department of Health and Human Services; NLM is not responsible for the product and does not endorse or recommend this or any other product."
PillSync may earn a commission via links on our site

